Measles in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is measles?
Measles is a disease caused by a virus. The virus is spread when an infected person coughs or sneezes. It is also spread through direct contact, such as sharing cups or toys. Measles can become serious, especially in children 5 years or younger or who have a weak immune system.
What are the signs and symptoms of measles?
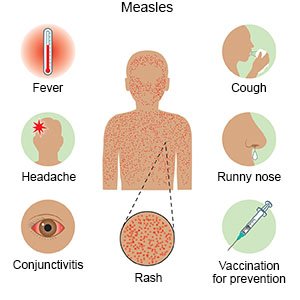
Your child may develop a rash about 2 to 3 days after he or she starts to feel sick. The measles rash usually begins on the face and head and then spreads down to the legs and feet. It may first appear as tiny spots that later join to make large patchy bumps. The rash usually disappears in 5 to 8 days, and may cause the skin to peel. Your child may also have any of the following:
- A fever, cough, runny nose, sore throat, and muscle aches
- Red, irritated eyes that are sensitive to light
- Small white spots that appear inside his or her mouth, usually on the cheeks
- Abdominal pain, vomiting, or diarrhea
 |
How is measles diagnosed?
Your child's healthcare provider may be able to diagnose measles based on your child's symptoms and a physical exam. Your child may need a blood test to confirm the infection.
What can I do to manage my child's symptoms?
Measles cannot be cured. The following may help relieve your child's symptoms:
- Give your child liquids as directed. Liquids help prevent dehydration. Ask how much liquid to give your child each day and which liquids are best for him or her. Give your child water, juice, or broth instead of sports drinks. He or she may need an oral rehydration solution (ORS). An ORS has the right amounts of water, salts, and sugar your child needs to replace body fluids. Ask your child's healthcare provider where you can get an ORS.
- Help your child rest. He or she should rest as much as possible and get plenty of sleep.
- Use a cool mist humidifier. A humidifier helps increase air moisture in your home. This may make it easier for your child to breathe and help decrease his or her cough.
- Give your child a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. This will help your child feel better and have more energy. If he or she is not hungry or gets tired easily, try feeding him or her smaller amounts more often.
- Protect your child's eyes. Keep the lights dim or give your child sunglasses to wear. This will help decrease pain caused by sensitivity to light.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to give your child and how often to give it. Follow directions. Read the labels of all other medicines your child uses to see if they also contain acetaminophen, or ask your child's doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If your child takes blood thinner medicine, always ask if NSAIDs are safe for him or her. Always read the medicine label and follow directions. Do not give these medicines to children younger than 6 months without direction from a healthcare provider.
- Cough medicine is given to decrease your child's urge to cough and help him or her rest.
What can I do to prevent measles?
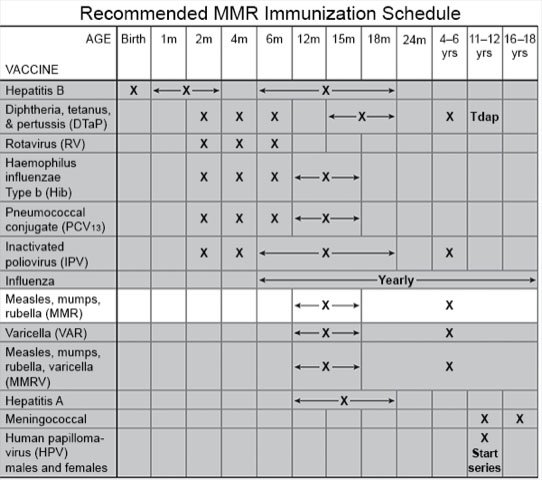
- Ask your child's healthcare provider about the MMR vaccine. This vaccine helps protect your child and others around him or her from measles, mumps, and rubella. Your child's provider will tell you how many doses your child needs. He or she will tell you when to bring your child in to get the vaccine.
- Prevent the spread of the measles virus:
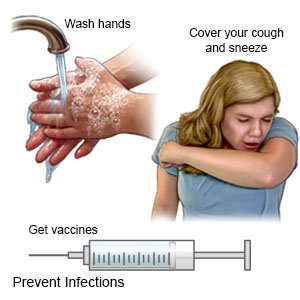
- Have your child wash his or her hands often. He or she should wash after using the bathroom and before preparing or eating food. Have your child use soap and water. Show him or her how to rub soapy hands together, lacing the fingers. Wash the front and back of the hands, and in between the fingers. The fingers of one hand can scrub under the fingernails of the other hand. Teach your child to wash for at least 20 seconds. Use a timer, or sing a song that is at least 20 seconds. An example is the happy birthday song 2 times. Have your child rinse with warm, running water for several seconds. Then dry with a clean towel or paper towel. Your older child can use hand sanitizer with alcohol if soap and water are not available.

- Remind your child to cover a sneeze or cough. Show your child how to use a tissue to cover his or her mouth and nose. Have your child throw the tissue away in a trash can right away. Then your child should wash his or her hands well or use a hand sanitizer. Show your child how to use the bend of his or her arm if a tissue is not available.
- Keep your child away from others, especially anyone who is pregnant or has not had the MMR vaccine. Keep your child home from school, daycare, or work until a healthcare provider says he or she can return.
- Tell your child not to share toys or other items with anyone else.
- Clean surfaces often. Use a disinfecting wipe, a single-use sponge, or a cloth you can wash and reuse. Use disinfecting cleaners if you do not have wipes. You can create a disinfecting cleaner by mixing 1 part bleach with 10 parts water. In the kitchen, clean countertops, cooking surfaces, and the fronts and insides of the microwave and refrigerator. In the bathroom, clean the toilet, the area around the toilet, the sink, the area around the sink, and faucets. Clean surfaces in the person's room, such as a desk or dresser.
- Have your child wash his or her hands often. He or she should wash after using the bathroom and before preparing or eating food. Have your child use soap and water. Show him or her how to rub soapy hands together, lacing the fingers. Wash the front and back of the hands, and in between the fingers. The fingers of one hand can scrub under the fingernails of the other hand. Teach your child to wash for at least 20 seconds. Use a timer, or sing a song that is at least 20 seconds. An example is the happy birthday song 2 times. Have your child rinse with warm, running water for several seconds. Then dry with a clean towel or paper towel. Your older child can use hand sanitizer with alcohol if soap and water are not available.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Call your local emergency number (911 in the US) if:
- Your child has a seizure.
When should I seek immediate care?
- Your child has trouble breathing or is breathing faster than usual.
- Your child has a headache, drowsiness, and stiff neck.
- Your child seems confused or less alert than usual.
When should I call my child's doctor?
- Your child's cough lasts for more than 4 days.
- Your child coughs up thick mucus.
- Your child has an earache.
- Anyone in your household develops a rash.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Measles
Treatment options
- Medications for Encephalomyelitis, Acute Disseminated
- Medications for Eye Conditions
- Medications for Infection
- Medications for Measles
- Medications for Pleuropulmonary Infection
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
