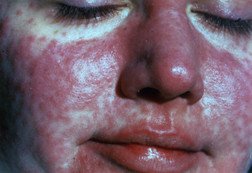
Measles (rubeola)
Medically reviewed by Drugs.com. Last updated on Nov 21, 2023.
What is Measles (rubeola)?

Measles, also known as rubeola, is an infection, mainly of the nose, windpipe and lungs that is very contagious, meaning it spreads easily from person to person. The measles virus usually spreads when someone comes into contact with droplets from another person that contain the virus. This can happen when someone with the virus coughs or sneezes. It also can happen when people touch used tissues, share drinking glasses or touch hands that have infected droplets on them.
|
|
Once the virus gets into the body, the infection spreads throughout the nose, windpipe and lungs, into the skin and other body organs.
A person with measles can spread the virus to others from one to two days before any symptoms begin (or three to five days before the rash) to four days after the rash appears.
Measles typically causes moderate illness. In younger children, complications include middle ear infection (otitis media), pneumonia, croup and diarrhea. In adults, the illness tends to be even more severe. It is not unusual for older patients to require hospital treatment for measles-related pneumonia.
The most serious consequences of measles are rare. In less than 1 of every 1,000 cases, measles produces encephalitis (brain infection), with an immediate risk of seizures, coma and death, and a long-term risk of intellectual disabilities or epilepsy. Subacute sclerosing panencephalitis is an extraordinarily rare chronic form of measles encephalitis that causes brain damage. In unusual cases, measles also can directly attack the digestive organs (including the liver), the heart muscle or the kidneys. A pregnant woman who is infected with measles has an increased risk of premature labor, miscarriage or delivery of a low-birth-weight infant.
Before an effective vaccine was available, there were at least 400,000 cases of measles reported each year in the United States, with probably more than 3 million unreported cases. The number of cases has decreased dramatically since childhood vaccination became routine. However, in recent years, there have been more outbreaks, primarily related to more parents refusing MMR vaccination of their children.
Symptoms
Measles symptoms begin about 8 to 12 days after coming in contact with someone who has measles. The first symptoms include coughing, runny and stuffy nose, a general, sick feeling (malaise), red eyes with tearing (conjunctivitis), and a fever up to 105 degrees Fahrenheit. Within two to four days, these symptoms are followed by Koplik's spots in the mouth, bluish white or gray spots on a red background, seen inside the cheeks.
With a measles rash, you usually see non-itchy pink or bright red spots. The rash begins at the hairline and behind the ears, then spreads downward to the neck, trunk, arms and legs, palms and soles. The rash begins to fade about four days later in the same order that it appeared, first from the head and neck, then the trunk and arms and legs. The fading rash may leave behind a temporary brownish discoloration or flakiness that clears up two to three days later. Some people also have big lymph nodes (swollen glands), diarrhea and vomiting.
Patients with compromised immune systems are more likely to develop severe complications from measles, but they may not develop the typical measles rash.
Diagnosis
Your doctor will check for a congested nose, red eyes, Koplik's spots and the typical measles rash. He or she will ask if you have been traveling outside the country or have been exposed to anyone with measles or an undiagnosed rash. Even if you did not have face-to-face contact with an infected person, your doctor will want to know if you go to the same school, live in the same household or dormitory or work in the same building. Your doctor will check your medical records to see if and when you were immunized against measles, and the number of doses of measles vaccine. These are given as part of the measles-mumps-rubella vaccine (MMR) shot.
To confirm the diagnosis, your doctor may order blood tests to look for specific antibodies that fight against the measles virus. Antibodies are made by the immune system to protect against an infection.
Expected duration
The symptoms of measles usually last about 10 days.
Prevention
You can prevent measles with the measles vaccine, given as part of the MMR combination vaccine. In the United States, most children receive two doses of the MMR vaccine, the first at 12 to 15 months of age and a booster dose at 4 to 6 years. If a person has not been immunized against measles and has been exposed to the disease, the vaccine may provide protection if it is given within 72 hours of the exposure. If the exposure is beyond three days but no longer than six days later, the person can receive an injection of immune globulin (IG), which contains antibodies to protect against the measles virus. It can prevent or at least minimize the symptoms of a measles infection. IG also can be used after exposure to measles in infants less than 6 months of age and in people who have conditions that weaken the immune system.
Drugs used to treat this and similar conditions
Treatment
There is no specific treatment for measles. In people who are otherwise healthy, measles symptoms are treated with bed rest, a cool-mist humidifier to soothe respiratory passages and relieve cough, and acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) to reduce fever and relieve discomfort. Do not use aspirin in children with measles because of the risk of developing a rare liver and brain problem called Reye's syndrome. Children and adults who develop a middle ear infection or bacterial pneumonia are treated with antibiotics.
In people hospitalized with measles and its complications, especially children 6 months to 2 years, some doctors prescribe high doses of vitamin A. Low levels of this vitamin have been found in children with severe cases of measles. The World Health Organization (WHO) recommends that all children with measles who live in communities where vitamin A deficiency is common should receive vitamin A.
In people with weakened immune systems or those who are severely ill from measles, the antiviral medication ribavirin (Virazole) occasionally has been used, but no controlled trials have proven its benefits. The U.S. Food and Drug Administration (FDA) has not approved the use of ribavirin to treat measles.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
Call your doctor if you or your child develops symptoms of measles, even if you or your child was immunized. Not everyone has received the two doses of the MMR vaccine they need to be fully protected. Call your doctor to review the status of your measles immunity if a measles outbreak occurs in your school or workplace. If you are considering becoming pregnant, contact your obstetrician to ensure that you are immunized against measles and other infectious diseases that can affect your unborn child. Always check with your child's doctor at each visit to be sure he or she is up-to-date for all immunizations.
Prognosis
Most healthy people recover completely from measles. About 3% of adults with measles develop symptoms of pneumonia severe enough to require hospital treatment. Death from measles complications such as pneumonia or encephalitis occurs in 1 to 2 of every 1,000 cases, more commonly in infants, older adults or people with weakened immune defenses.
Additional info
Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.