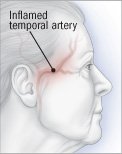
Giant cell arteritis (temporal arteritis)
Medically reviewed by Drugs.com. Last updated on Mar 5, 2025.
What is Giant cell arteritis (temporal arteritis)?

Giant cell arteritis, also called temporal arteritis, is a disease in which the large arteries and their branches, including those that supply the eye, scalp, and face, become inflamed and narrowed. This disease can cause loss of vision, so it is essential that the problem be diagnosed and treated as early as possible. Larger blood vessels, including the aorta and its branches, also may be involved, and can lead to the blood vessel weakening and even rupturing years later.
|
|
This disorder develops almost exclusively in people older than age 55 and most commonly affects people in their 70s and 80s. It is relatively rare: among people over the age of 55, it affects an estimated two people in 1,000.
The cause of giant cell arteritis is unknown, although there has been speculation that in some people, the body's immune system responds incorrectly to an infection, and begins to attack the lining of blood vessels as it would a foreign invader. There may be a genetic contribution as well, as suggested by occasional cases that affect more than one member of the same family. One possibility is that the immune system of certain individuals or family members may be genetically programmed to respond to an infection abnormally, a response that leads to giant cell arteritis.
Symptoms
The most common symptom is a dull, throbbing headache, often at one or both sides of the forehead, although it can be anywhere over the head or into the neck. Other common symptoms include one or more of the following:
- fever
- jaw pain after chewing
- loss of appetite
- fatigue
- dry cough
- tenderness of the scalp or temples
- blurring or loss of vision in one eye
- aching in the shoulders, upper arms, or hips or upper thighs, especially in the morning (typical of polymyalgia rheumatica, an arthritic condition associated with giant cell arteritis).
Diagnosis
Your doctor may suspect you have this disorder if you are an older adult with a new headache. He or she will begin by asking you for a detailed description of your symptoms, past medical problems, and medications. Next, the doctor will examine you, paying particular attention to your temporal arteries, located just in front of the ear, above the jaw, and other blood vessels.
Your doctor will consider other causes of headache or other symptoms and may order tests to check for these conditions. However, if giant cell arteritis is still a strong concern after these tests, blood tests to detect inflammation, called the erythrocyte sedimentation rate (ESR) and c-reactive protein (CRP), may be ordered because they tend to be elevated in this condition.
A biopsy of the temporal artery generally is required to confirm the diagnosis. In this procedure, a small piece of the blood vessel will be removed under local anesthesia and will be examined in a laboratory. New research suggests that other tests, including ultrasound of the temporal arteries, may be useful for the detection of this condition, but a biopsy is still considered the best available test.
Expected duration
Giant cell arteritis typically lasts at least several years. However, improvement usually begins within days of starting therapy. Some people are able to discontinue treatment within six months, but longer treatment over two to three years is more usual. Occasionally, the disease returns after it has gone away for a prolonged period.
Prevention
There is no way to prevent this disease. Vision loss (and, perhaps, other complications) may be prevented by prompt diagnosis and treatment.
Drugs used to treat this and similar conditions
Treatment
Giant cell arteritis is a serious disease that requires prompt medical attention since delay in diagnosis and treatment can lead to vision loss or other complications. The main treatment is high doses of prednisone, a corticosteroid, and most people feel better within a few days. Medication is continued at a high dose for approximately one month and then tapered gradually over the following months to the lowest possible dose, or is discontinued.
It is common for people with this disorder to require at least six months of therapy. Treatment is typically continued for a year or more because many people experience symptoms typical of polymyalgia rheumatica (aching in the shoulders, hips, or both) or recurrent headaches as the prednisone dose is reduced.
In 2017, tocilizumab (Actemra) was approved for the treatment of giant cell arteritis as studies demonstrated that, along with corticosteroids, it was effective for this condition, including a steroid-sparing effect. This medication may be recommended if symptoms repeatedly return as the steroids are reduced, or if there are other conditions for which steroid therapy may be particularly troublesome (including diabetes or osteoporosis).
Some studies have found that another medication, methotrexate (Folex, Rheumatrex), may reduce the dose of corticosteroids required and the length of time they need to be taken, although other studies have not confirmed this. As a result, some physicians prescribe methotrexate as a "steroid-sparing" agent in the hopes of reducing the overall exposure to corticosteroids. However, the evidence to date suggests that tocilizumab is more effective than methotrexate as a steroid-sparing drug.
The use of steroids can lead to complications, including osteoporosis, diabetes, and weight gain; measures to prevent these complications (such as supplemental calcium and vitamin D) are routinely recommended. Bone density testing is also recommended to monitor bone density and identify osteoporosis. Research is ongoing to identify other effective steroid-sparing medications.
Some research suggests that low-dose aspirin may help to prevent complications of giant cell arteritis, including loss of vision. While the true impact of aspirin is uncertain, it is often recommended along with steroid therapy for this condition.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
If you have any symptoms of giant cell arteritis, especially a new headache, unexplained fever, or visual symptoms, you should contact your doctor.
Prognosis
If vision has not been affected, the outlook is excellent. However, once vision loss occurs, it is usually permanent. If the aorta or nearby branches are involved, the prognosis may be worse, because these blood vessels may enlarge or even rupture. However, most complications related to giant cell arteritis are caused by steroid therapy rather the disease itself.
Additional info
American College of Rheumatology
http://www.rheumatology.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.