Retinopathy
Medically reviewed by Drugs.com. Last updated on Sep 29, 2023.
What is Retinopathy?

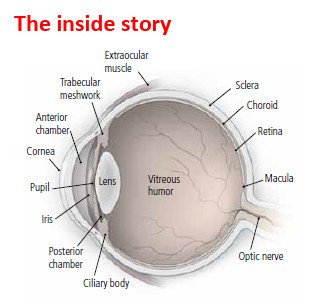
Retinopathy means that disease has damaged the retina. The retina is the part inside the eye that senses light. Different diseases can cause retinopathy. There can be partial or complete loss of vision. Retinopathy can develop slowly or suddenly, can get better on its own or lead to permanent damage.
|
|
The retina contains many blood vessels. Abnormalities in these vessels are a major cause of retinopathy.
There are several types of retinopathy, including:
- Retinopathy of prematurity (ROP). ROP occurs in some infants who are born prematurely or at a low birth weight. When a child is born too early, retinal blood vessels do not have time to finish growing properly. In the early stages of ROP, there are only subtle changes and no obvious symptoms. In more advanced stages, the retina can become detached, causing blindness.
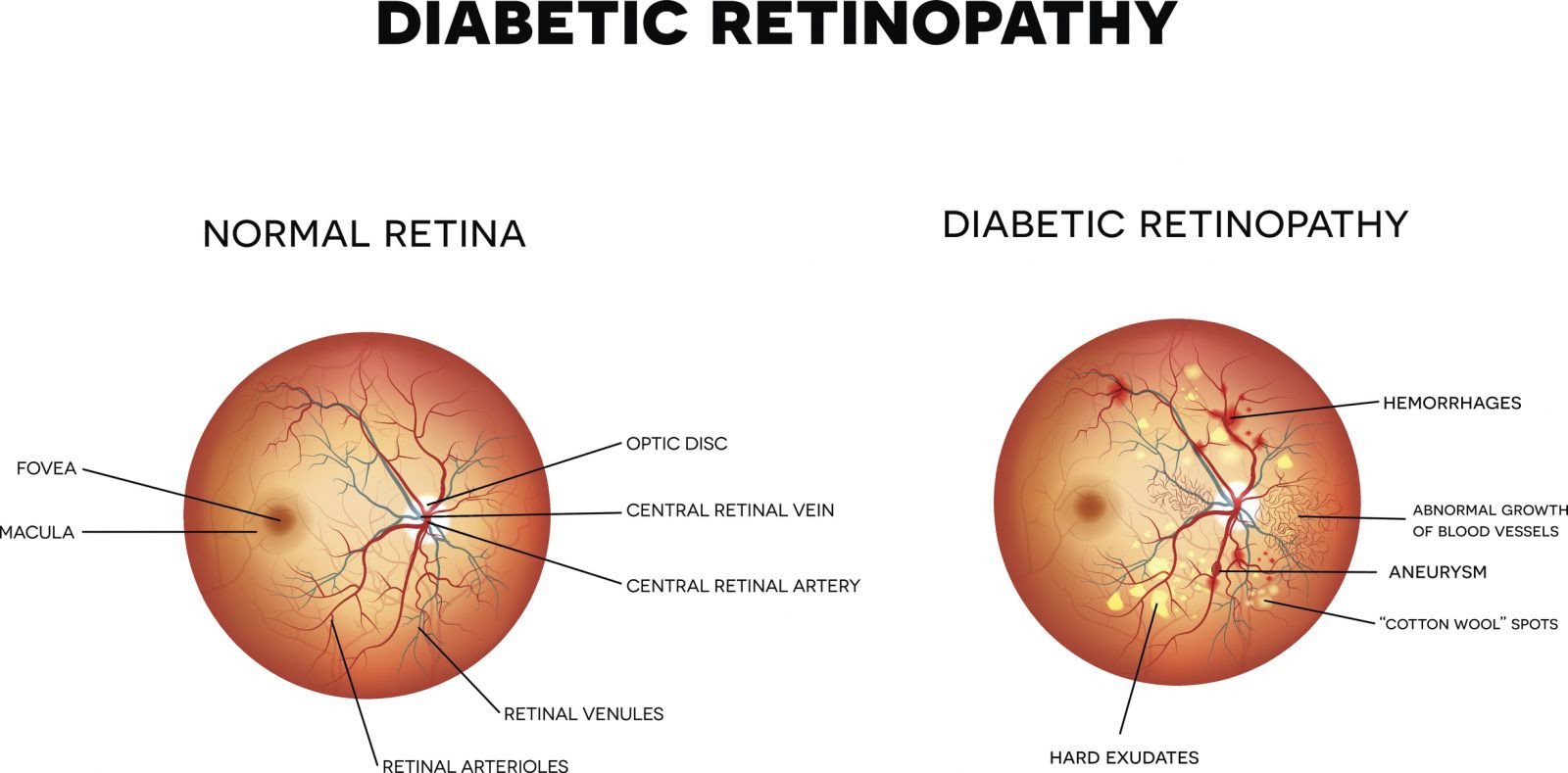
- Diabetic retinopathy. Diabetic retinopathy develops in people with type 1 or type 2 diabetes. It takes years to develop. Two kinds of diabetic retinopathy have the potential to diminish vision:
- In nonproliferative retinopathy, blood vessels in the retina deteriorate. Deteriorating blood vessels can become blocked or deformed. Fluids, fats and proteins leak out of the abnormal blood vessels. Fluid can collect in the retina. This swelling impairs sharp vision.
- In proliferative retinopathy, new, structurally unstable blood vessels grow on the surface of the retina. These unstable blood vessels cause frequent minor bleeding. The bleeding causes local irritation and scarring.
- Proliferative retinopathy can cause retinal detachment. This is a separation of the layers of the retina. It is one of the most serious consequences of proliferative retinopathy.
- The vitreous is the clear gel between the lens and the retina. Sudden bleeding into the vitreous can obscure vision, often quite suddenly.
|
|
- Hypertensive retinopathy. Hypertensive retinopathy occurs in people who have high blood pressure. High blood pressure causes blood vessel abnormalities. Abnormalities may include thickening of the small arteries, blockages of retinal blood vessels and bleeding from them. Sudden, severe high blood pressure may cause swelling of the optic nerve. People with this condition frequently have no symptoms in the early stages. It may be discovered during a routine eye exam.
- Central serous retinopathy. Central serous retinopathy begins for reasons that are not well understood. In this condition, fluid accumulates in the membrane behind the retina. The fluid seeps in between layers of the retina and causes them to separate. This results in blurred vision or poor night vision.
Symptoms
Retinopathy of prematurity — There are no outward physical signs. Only an experienced ophthalmologist can find signs of this illness.
Diabetic retinopathy — Symptoms may not be noticed until the late stages of the illness. Symptoms can include:
- Blurred vision
- Sudden loss of vision in one or both eyes
- Black spots
- Flashing lights
- Difficulty reading or seeing detailed work.
Hypertensive retinopathy — There are often no symptoms. Some people complain of blurred vision.
Central serous retinopathy — Symptoms include:
- Blurred or dim vision, sometimes coming on suddenly
- Blind spots
- Distorted shapes
- Reduced visual sharpness.
Diagnosis
Retinopathy of prematurity — An ophthalmologist examines the inside of the eye for abnormalities.
Diabetic retinopathy — An ophthalmologist examines the retina and inside of the eye. He or she uses a lighted instrument called an ophthalmoscope. A dye may be used to reveal leaky blood vessels.
Hypertensive retinopathy — A physician examines the eye with an ophthalmoscope. He or she looks for pale or white areas of the retina. These areas are pale because they are not getting enough blood. The doctor also may see bleeding from ruptured blood vessels or swelling of the retina or optic nerve.
Central serous retinopathy — A doctor or ophthalmologist uses an ophthalmoscope to detect fluid between layers of the retina. This fluid can resemble bubbles.
Expected duration
Retinopathy of prematurity — In most affected babies, this condition gets better on its own. Abnormal vessels disappear. A small number of more serious cases get worse without treatment. Babies who need treatment are treated in the first few months of life. It is usually possible to know within months whether there is any significant long-term damage to vision.
Diabetic retinopathy — Controlling blood sugar and blood pressure can help delay and maybe even prevent the onset of the disease. Treatments can repair existing damage.
Hypertensive retinopathy — Lowering blood pressure often can stop ongoing damage to the retina. However, some existing damage can persist.
Central serous retinopathy — Most cases go away without any treatment within three to four months. Full vision can return within six months.
Prevention
Retinopathy of prematurity — The first line of defense is regular prenatal care. This helps to prevent premature birth. Premature and low-birth-weight infants should be screened for retinopathy of prematurity if they:
- are born at less than 36 weeks of gestation
- weigh less than 4 pounds 6 ounces at birth.
ROP can be caused by or get worse from inadequate or too much oxygen after birth. Therefore, oxygen levels are closely monitored and adjusted.
Diabetic retinopathy — Controlling blood sugar and blood pressure are essential to prevent diabetic retinopathy.
Annual eye exams are crucial for people with diabetes. If you have diabetic retinopathy, you should have more frequent eye exams. Treatment can start before sight is affected, which helps prevent vision loss.
Hypertensive retinopathy — Avoid high blood pressure by:
- Exercising regularly
- Maintaining a healthy body weight
- Eating a healthy diet
- Getting regular checkups
- Taking blood pressure medications as directed.
Central serous retinopathy — The possible causes of this disease are not understood. Therefore, prevention is difficult. Because central serous retinopathy has been associated with corticosteroid treatment, high blood pressure and caffeine use, limiting the amount of corticosteroids and caffeine and maintaining a normal blood pressure are important measures.
Drugs used to treat this and similar conditions
Treatment
Retinopathy of prematurity — No treatment is recommended during the early, milder stages. However, close monitoring is essential. An ophthalmologist should examine high-risk infants before they are discharged from the hospital. Infants should be examined again at 8 weeks of age. If the disease is active, the infant should be examined every 1 to 2 weeks until he or she is 14 weeks old. After that, they should be examined every 1 to 2 months. More advanced disease may require treatment. Vascular endothelial growth factor (VEGF) inhibitors (including bevacizumab, and ranibizumab) can be injected into the eye as the initial treatment. Laser treatments may also be used. A detached retina can be reattached. An older procedure called cryotherapy uses cold to destroy abnormal blood vessels and may be used when laser treatment is not available.
Diabetic retinopathy — No therapy may be needed for mild nonproliferative disease. Otherwise, specific treatment depends on the nature and severity of disease, preferences of the patient and cost. Treatment options include:
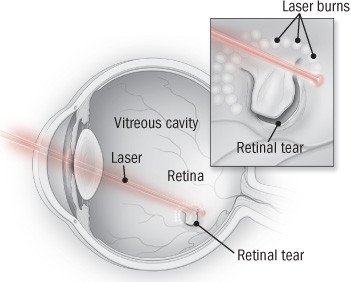
- Laser therapy (also called laser photocoagulation). This creates scars that slow the growth of new blood vessels.
|
Laser photocoagulation is usually done in a doctor's office. The ophthalmologist uses a laser to make a series of tiny burns around the retinal tear. This creates a barrier of scar tissue that stops the tear from getting bigger. |
- Injections of VEGF inhibitors into the eye
- Removing all or part of the vitreous (vitrectomy)
- Surgical reattachment of the retina (for retinal detachment).
For all type of diabetic retinopathy, blood sugar and blood pressure must be controlled to keep the eye disease from getting worse.
Hypertensive retinopathy — Medications can lower blood pressure. This can lead to improvements in the retina. People with very high blood pressure and swelling of the optic nerve require emergency treatment in a hospital.
Central serous retinopathy — This condition usually goes away on its own. If corticosteroid therapy can be safely reduced and discontinued, this may hasten recovery. An ophthalmologist should monitor you closely for three to six months. If the condition does not improve, laser treatment may speed healing.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
When to call a professional
Call a doctor if you notice changes in your vision, particularly if they are sudden. Changes may include:
- Blurring
- Spots
- Flashes
- Blind spots
- Distortion
- Difficulty reading or doing detail work.
Prognosis
The prognosis depends on what's causing the retinopathy, and how far it has progressed.
Retinopathy of prematurity — In most affected babies, this condition gets better on its own. Abnormal vessels disappear. However, more advanced cases can lead to a number of eye problems, including blindness.
Children with retinopathy of prematurity have an increased risk of:
- Retinal detachment
- Cataract
- Glaucoma
- Crossed eyes
- Lazy eye
- Nearsightedness.
Diabetic retinopathy — The outlook depends on:
- How well blood pressure and blood sugar are controlled
- How far the disease has progressed
- How closely it is monitored.
Treatments can repair damage and slow the progress of the disease. Advanced stages of diabetic retinopathy can lead to blindness.
Hypertensive retinopathy — Most changes in the retina caused by hypertensive retinopathy disappear after blood pressure has been lowered. Some signs of damage can remain.
Central serous retinopathy — Most cases go away on their own within three to four months. Full visual acuity usually returns within six months. Lasting symptoms can include:
- Distortion
- Decreased contrast sensitivity
- Difficulty with night vision.
For persistent disease, laser treatment or photodynamic therapy (a treatment using light and a chemical substance that makes certain cells sensitive to light) may be offered. Central serous retinopathy recurs in about half of affected people.
Additional info
American Academy of Ophthalmology
https://www.aao.org
National Eye Institute
https://www.nei.nih.gov/
American Academy of Pediatrics
https://www.aap.org/
National Heart, Lung, and Blood Institute (NHLBI)
https://www.nhlbi.nih.gov/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.