Pituitary tumors
Medically reviewed by Drugs.com. Last updated on Feb 15, 2024.
What are pituitary tumors?

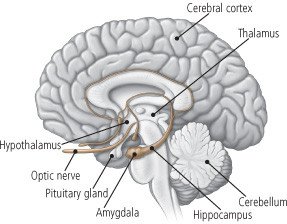
The pituitary gland is a pea-sized structure that is attached to the undersurface of the brain by a thin stalk. It is protected by a cradle of bone called the sella turcica, which is located above the nasal passages, almost directly behind the eyes. The pituitary gland sometimes is called the master gland because it produces hormones that regulate many bodily functions, including the production of:
- thyroid hormone
- sex hormones, such as estrogen and testosterone
- adrenalin
- growth hormone
- breast milk
- anti-diuretic hormone that helps control water balance.
|
|
When tumors develop in the pituitary gland, they are usually small, localized, slow-growing masses that start in one type of hormone-producing pituitary cells. Although these tumors almost always are benign (noncancerous), they have the potential to cause significant symptoms by:
- producing too much of one of the pituitary hormones
- suppressing the normal function of other cells in the pituitary gland
- growing large enough to press on the nearby optic nerves (nerves that carry vision impulses from the eyes to the brain) or on parts of the brain itself.
A pituitary tumor is classified as one of four main types, based on whether it overproduces pituitary hormones and the specific type of hormone produced:
- ACTH-producing tumor — This pituitary tumor, which also is called a basophilic adrenocorticotrophic hormone-secreting adenoma, overproduces adrenocorticotrophic hormone (ACTH). ACTH is the pituitary hormone that regulates hormone production by the adrenal gland. When this type of pituitary tumor releases too much ACTH into the bloodstream, the extra ACTH overstimulates the adrenal glands to pour out high levels of adrenal glucocorticoids (adrenal hormones) and androgens (male hormones) into the blood. In most cases, an ACTH-producing tumor is small and doesn't grow beyond the sella turcica.
- Prolactin-producing tumor — This pituitary tumor, which also is called a prolactin-secreting adenoma, overproduces the hormone prolactin, which stimulates the breasts to make milk. Prolactin-producing pituitary tumors can develop in both men and women, and they sometimes grow so big that they press on the sella turcica and cause it to get larger.
- Growth hormone-producing tumor — This tumor, which also is called an eosinophilic growth hormone-secreting adenoma, secretes abnormally large amounts of growth hormone. In children and teenagers, this overproduction of growth hormone causes a condition called giantism (excessive growth, especially in height). In adults, it causes a condition called acromegaly (abnormal enlargement of the skull, jaw, hands and feet, and other symptoms of abnormal growth). Growth hormone-producing tumors can grow beyond the sella turcica.
- Non-functioning pituitary tumor — This type of pituitary tumor, which also is called a hormonally inactive adenoma, does not cause pituitary hormones and is slow to produce symptoms. For this reason, this type of tumor tends to grow large before it is discovered. In many cases, a nonfunctioning pituitary adenoma is diagnosed only when it already has grown beyond the sella turcica and has begun to cause problems related to pressure on the optic nerves or brain.
In the United States, pituitary tumors are diagnosed in 1 to 15 of every 200,000 people each year, most commonly in women between the ages of 15 and 44. However, autopsy studies suggest that a much larger percentage of the population — perhaps as high as 11% — may have very tiny pituitary tumors that never cause symptoms.
Symptoms of pituitary tumors
A pituitary tumor causes symptoms based on:
- the type of hormone the tumor is overproducing
- the size of the tumor
- the effect the tumor has on the normal production of all the other pituitary hormones.
ACTH-producing tumor
This tumor causes symptoms of Cushing's disease, a condition caused by prolonged overproduction of adrenal glucocorticoids and androgens. Symptoms of Cushing's disease include obesity that is most noticeable on the trunk of the body, thin skin, easy bruising, red or purple lines (striae) on the skin of the abdomen, a moon-shaped face, muscle wasting, excess body hair in women, acne, absence of menstrual periods (amenorrhea) and psychiatric symptoms, such as depression and psychosis. Cushing's disease also can trigger osteoporosis, high blood pressure (hypertension), and diabetes.
Prolactin-producing tumor
This tumor occasionally causes a woman who is not pregnant or nursing to produce breast milk, a condition called galactorrhea. Much more often, it causes absent periods (amenorrhea). In men, it causes impotence and decreased sex drive.
Growth hormone-producing tumor
If this tumor develops before puberty, then the child typically has the following symptoms of giantism (also called gigantism): abnormally rapid growth, unusually tall stature, a very large head, coarse facial features, very large hands and feet, and sometimes, behavioral and visual problems. If the tumor develops after puberty, then the person has the following symptoms of acromegaly: thick, oily skin; coarse features with thick lips and a broad nose; prominent cheekbones; a protruding forehead and lower jaw; a deep voice; enlargement of the hands and feet; a barrel-shaped chest; excessive sweating; and pain and stiffness in the joints.
Nonfunctioning pituitary tumor
These tumors do not produce excessive amounts of hormone. They may be found:
- accidentally when magnetic resonance imaging (MRI) of the brain is done for other reasons
- if they get large enough to affect the production of other pituitary hormones
- if they grow beyond the sella turcica and are causing pressure on the brain or optic nerves that are next to the sella turcica.
Prolactin-producing tumors and nonfunctioning tumors can depress the pituitary's ability to make and release other hormones. Sex hormones usually are depressed first followed by thyroid hormone and then adrenal hormones. Symptoms related to low sex hormone levels include loss of sexual drive, erectile dysfunction, and absence of menstrual periods. If a tumor keeps growing, the person may develop fatigue and lightheadedness because the thyroid and adrenal glands aren't functioning properly.
A very large pituitary tumor that grows beyond the sella turcica can cause headaches, loss of peripheral vision and partial paralysis of the eye muscles.
Diagnosing pituitary tumors
Your doctor will review your symptoms, medical history and current medications. This information is very important because certain medical conditions and/or prescription drugs can have significant effects on your levels of body hormones. For example, psychiatric drugs called neuroleptics can increase blood levels of prolactin, and prescription glucocorticoids (even therapeutic injections of dexamethasone — Decadron and other brand names — into injured joints) can cause high blood levels of glucocorticoids.
During a physical examination, your doctor will look for the signs that show your body is overproducing a particular pituitary hormone. For example, your doctor may look for breast milk production caused by a prolactin-producing tumor or a moon-shaped face and abdominal marks caused by an ACTH-producing tumor.
If your doctor suspects that you have a pituitary tumor, the first step usually is a blood test for hormone levels. Your doctor probably will order an MRI scan of your head to obtain detailed images of the pituitary gland. Usually this test involves an injection of a dye called gadolinium, which is used to highlight brain structures.
If you are having any visual symptoms or the MRI shows a large pituitary tumor, your doctor will refer you to an eye specialist (ophthalmologist) for a comprehensive eye exam, including special eye tests that detect visual loss in specific visual fields.
Expected duration of pituitary tumors
In most cases, a pituitary tumor will continue to slowly grow until it is treated. Sometimes, however, a prolactin-secreting tumor will stabilize, or even improve, without treatment.
Preventing pituitary tumors
Because doctors do not know why pituitary tumors develop, there is no way to prevent them.
Treating pituitary tumors
Doctors have two main goals in treating pituitary tumors: to reduce the abnormally high levels of hormones and to shrink the tumor to prevent pressure damage to the optic nerves and brain. Treatment depends on the type of pituitary tumor:
- ACTH-producing tumor — Most people with this type of pituitary tumor undergo a surgical procedure called transsphenoidal hypophysectomy. In this procedure, the surgeon removes the pituitary tumor through an incision in the upper portion of the nasal passages. After surgery, levels of glucocorticoid hormones are abnormally low, so the patient typically needs to take supplemental glucocorticoid medication for about 3 to 12 months. This medication gradually is tapered as the body slowly reestablishes a normal working relationship between the pituitary gland and the adrenal glands. If the tumor cannot be completely removed by surgery, radiation therapy may be needed.
- Prolactin-producing tumor (prolactinoma) — Treatment is determined by the size of the tumor and how much prolactin is being produced. Small tumors sometimes don't need to be treated and can be monitored to see if they change. If treatment is necessary, the doctor will prescribe one of the drugs called long-acting dopamine agonists, such as bromocriptine (Parlodel) or cabergoline (Dostinex). These drugs reduce blood levels of prolactin and often shrink the size of the pituitary tumor. If a prolactinoma is large or produces high levels of prolactin, surgery may be recommended. Surgery also may be needed if medications don't help or the person can't take the medications long term because of side effects. When surgery is needed, the tumor is removed with a procedure called transsphenoidal hypophysectomy. In rare cases, radiation therapy may be needed.
- Growth hormone-producing tumor — Transsphenoidal hypophysectomy is usually the first choice. If the tumor cannot be completely removed or blood levels of insulin-like growth factor 1 (IGF-1) and growth hormone remain elevated, doctors use drug therapy with a somatostatin analog, such as octreotide (Sandostatin) or lanreotide (Somatuline Depot). If the response is still inadequate, then a drug called pegvisomant is recommended. Radiation therapy is used in people who do not respond to surgery or medication.
- Nonfunctioning pituitary tumor — Many doctors do not treat nonfunctioning pituitary tumors if the tumor is less than 10 millimeters in diameter. Instead, they monitor the growth of the tumor with periodic MRI scans. Larger tumors are removed surgically using a transsphenoidal hypophysectomy, sometimes followed by radiation therapy to eliminate any remaining tumor.
Transsphenoidal hypophysectomy is a safe and effective procedure that is popular for cosmetic reasons. However, not all pituitary tumors can be removed by using this surgical approach, either because the tumor is too large or because it is in a position that is difficult to reach through the nose. Instead, the surgeon must do a procedure called a craniotomy, which removes the tumor through an incision in the front portion of the skull.
When to call a professional
Make an appointment to see your doctor if:
- you have frequent headaches
- you notice that your vision is becoming less sharp
- you have trouble seeing objects in a particular visual field
- you think that you may have symptoms of Cushing's disease or acromegaly
- you are a woman who has unexplained absent periods or is producing breast milk when you are not nursing
- you are a man who is impotent or has decreased sexual desire
- you are a parent who is worried that your child is growing faster or taller than expected.
Prognosis
The outlook depends on the type of pituitary tumor, the size of tumor at the time of diagnosis and the extent of injury to the optic nerves and other parts of the body:
- ACTH-producing tumor — After surgery, the cure rate is 80% to 90% for ACTH-producing tumors that have not enlarged beyond the sella turcica. If the tumor cannot be completely removed surgically, radiation therapy is often successful.
- Prolactin-producing tumor — Medical treatment is safe and effective in the great majority of cases, even when the tumor is fairly large. In women of childbearing age whose periods disappear because of a prolactin-producing pituitary tumor, medical treatment often restores fertility. When surgery is needed, success rates are very high.
- Growth hormone-producing tumor — Approximately 60% of tumors can be cured with surgery. In people treated medically, medication lowers hormone levels and relieves symptoms in most cases.
- Non-functioning pituitary tumor — The outlook depends on the size of the tumor. People with small tumors that do not need immediate treatment or can be completely removed with surgery have an excellent prognosis. Even for large tumors that interfere with vision, surgery can stop further deterioration of vision.
Additional info
National Cancer Institute (NCI)
https://www.cancer.gov
American Cancer Society (ACS)
https://www.cancer.org/
American Association of Clinical Endocrinologists
https://www.aace.com/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.