Stroke
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
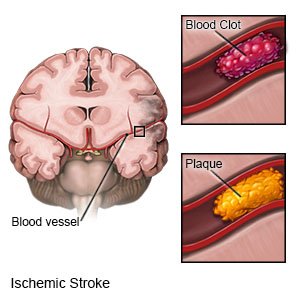
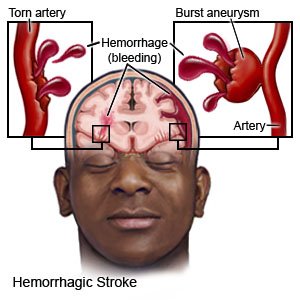
A stroke happens when blood flow to part of the brain is stopped. This can cause serious brain damage from a lack of oxygen. Your healthcare providers will help you create goals for your recovery. They will help you and your family or care providers make a plan for care at home to help you reach your goals. The plan will include lifestyle changes you can make to help you manage your health and prevent another stroke. Your discharge instructions will include information on services and equipment you or your family may need.
 |
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) or have someone call if:
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss

- You have a seizure.
- You have chest pain or shortness of breath.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- You have unusual or heavy bleeding.
Call your doctor or neurologist if:
- Your blood sugar level or blood pressure is higher or lower than usual.
- You have trouble swallowing.
- You have trouble having a bowel movement or urinating.
- You have questions or concerns about your condition or care.
Medicines:
Medicines may be needed to treat high cholesterol, high blood pressure, or diabetes. You may also need any of the following, depending on the kind of stroke you had:
- Antiplatelets , such as aspirin, help prevent blood clots. Take your antiplatelet medicine exactly as directed. These medicines make it more likely for you to bleed or bruise. If you are told to take aspirin, do not take acetaminophen or ibuprofen instead.
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Know the warning signs of a stroke:
The words BE FAST can help you remember and recognize warning signs of a stroke:
- B = Balance: Sudden loss of balance
- E = Eyes: Loss of vision in one or both eyes
- F = Face: Face droops on one side
- A = Arms: Arm drops when both arms are raised
- S = Speech: Speech is slurred or sounds different
- T = Time: Time to get help immediately
 |
Related medications
Recovery testing:
Your healthcare provider will test your recovery 90 days (3 months) after your stroke. This may be done over the phone or in person. Your provider will ask how well you can do the activities you did before the stroke. Your provider will also ask how well you can do your daily activities without help. Your provider may make recommendations for you based on your test. For example, you may need someone to help you walk safely. You may also need help with daily activities, such as getting dressed. Based on your answers, your provider may do this test again over time.
Manage the effects of a stroke:
- Go to stroke rehabilitation (rehab) if directed. Rehab is a program run by specialists who will help you recover abilities you may have lost. Specialists include physical, occupational, and speech therapists. Physical therapists help you gain strength or keep your balance. Occupational therapists teach you new ways to do daily activities. Your therapy may include movements for everyday activities. An example is being able to raise yourself from a chair. A speech therapist helps you improve your ability to talk and swallow.
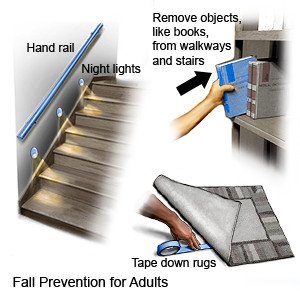
- Make your home safe. Remove anything you might trip over. Tape electrical cords down. Keep paths clear throughout your home. Make sure your home is well lit. Put nonslip materials on surfaces that might be slippery. An example is your bathtub or shower floor. A cane or walker may help you keep your balance as you walk.
Prevent another stroke:
- Manage health conditions. Diabetes and high cholesterol can increase your risk for a stroke. Control your blood sugar and cholesterol levels as directed. Talk to your healthcare provider about your management plan. Your provider will make a plan that helps you manage your conditions. Take your prescribed medicines and check your blood sugar level as directed.
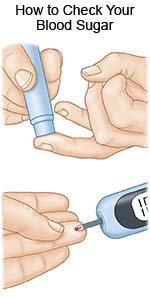
- Check your blood pressure as directed. High blood pressure can increase your risk for a stroke. Follow your provider's directions for controlling your blood pressure.

- Do not use nicotine products or illegal drugs. Nicotine and other chemicals in cigarettes and cigars can cause blood vessel damage. Nicotine and illegal drugs both increase your risk for a stroke. Ask your provider for information if you currently smoke or use drugs and need help to quit. E- cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Talk to your provider about alcohol. Alcohol can raise your blood pressure. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor. Your provider can help you set limits for the number of drinks you have within 24 hours and within a week.
- Eat a variety of healthy foods. Healthy foods include whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Eat at least 5 servings of fruits and vegetables each day. Choose foods that are low in fat, cholesterol, salt, and sugar. Eat foods that are high in potassium, such as potatoes and bananas. A dietitian can help you create healthy meal plans.

- Maintain a healthy weight. Ask your healthcare provider what a healthy weight is for you. Your provider can help you create a weight loss plan, if needed.
- Be physically active as directed. Physical activity, such as exercise, can lower your blood pressure, cholesterol, weight, and blood sugar levels. Healthcare providers will help you create exercise goals. They can also help you make a plan to reach your goals. For example, you can break exercise into 10 minute periods, 3 times in the day. Find an exercise that you enjoy. This will make it easier for you to reach your exercise goals.

- Manage stress. Stress can raise your blood pressure. Find new ways to relax, such as deep breathing or listening to music.
What you need to know about depression after a stroke:
Talk to your healthcare provider if you have depression that continues or is getting worse. Your provider may be able to help treat your depression. Your provider can also recommend support groups for you to join. A support group is a place to talk with others who have had a stroke. It may also help to talk to friends and family members about how you are feeling. Tell your family and friends to let your provider know if they see any signs of depression:
- Extreme sadness
- Avoiding social interaction with family or friends
- A lack of interest in things you used to enjoy
- Irritability
- Trouble sleeping
- Low energy levels
- A change in eating habits or sudden weight gain or loss
Follow up with your doctor or neurologist as directed:
You may need to come in for regular tests of your brain function. Your provider may refer you to a specialist, or to other kinds of care. An example is palliative (comfort) care. Your provider can also give information about respite care to anyone who helps care for you. Respite care is a service to help caregivers take a break or get more rest. Write down your questions so you remember to ask them during your visits.
For support and more information:
- American Stroke Association
Phone: 1- 888 - 478-7653
Web Address: http://www.stroke.org
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Stroke
- Atorvastatin (Lipitor): Top 12 Drug Facts You Need to Know
- Should you mix muscle relaxants with alcohol?
Treatment options
- Medications for Cerebral Thrombosis/Embolism
- Medications for Cerebrovascular Insufficiency
- Medications for Hemorrhagic Stroke
- Medications for Ischemic Stroke
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
