Polycythemia Vera
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Polycythemia vera (PV) is a condition that causes your bone marrow to produce too many red blood cells (RBCs). RBCs carry oxygen throughout the body. Too many white blood cells (WBCs) and platelets may also be produced. The extra blood cells make your blood thicker than normal. Blood that is too thick cannot flow easily, so less oxygen is delivered to your body's tissues. Left untreated, PV is life-threatening. PV is usually caused by a gene mutation (change). Your risk for PV increases if you are male or older than 50 years.
DISCHARGE INSTRUCTIONS:
Call 911 for any of the following:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
- You have a severe headache or a seizure.
- You cough up blood.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- You have new or worsening symptoms.
- You have heavy bleeding that does not stop after 20 minutes of applied pressure.
Contact your healthcare provider if:
- Your nose or gums bleed.
- You see blood in your urine.
- You have a sore or skin changes on your hands or feet, or under your compression stocking.
- You have more bruises than usual.
- You have questions or concerns about your condition or care.
Medicines:
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Aspirin can help thin your blood, and relive bone pain and burning in your hands or feet. Aspirin can cause stomach bleeding in some people. Only take aspirin if directed by your healthcare provider. Do not take more than the recommended amount.
- Medicines may be given to reduce itching or uric acid, or to control stomach acid production. Do not take iron supplements.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Related medications
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Follow up with your healthcare provider as directed:
You may need ongoing tests or treatment. Write down your questions so you remember to ask them during your visits.
Do not smoke:
Nicotine and other chemicals in cigarettes and cigars can increase your risk for blood clots and cause lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
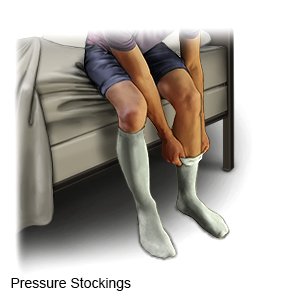
Help keep your blood flowing:
Wear support stockings as directed. Support stockings are tight and help push blood up and out of your lower leg veins. Elevate your feet when you sit. This will help prevent blood from pooling in your leg veins.
 |
Exercise as directed:
Exercise helps improve blood flow and prevents blood clots. Ask your healthcare provider which exercises are best for you. Stop if you feel any chest pain or shortness of breath.
Drink liquids as directed:
Liquids help keep your blood thin. Your healthcare provider may recommend that you drink at least 3 liters (12 cups) of liquid each day. Ask which liquids are best for you.
Manage your symptoms:
- Prevent bleeding and bruising. PV or blood thinners used to manage it can increase your risk for heavy bleeding and easy bruising. Use an electric razor and soft toothbrush. Floss your teeth gently. Do not play contact sports, such as football. These sports increase the risk for bruising. Get care immediately if you are injured. Ask about other ways to prevent bleeding and bruising. Tell all healthcare providers that you have PV or are taking blood thinners.
- Protect your hands and feet. Wear gloves outside if the temperature is low. Check your hands and feet for sores caused by blood circulation problems. You may not feel the sores because of the low blood flow.
- Avoid high temperatures. Do not take hot baths or sit in hot tubs. The heat can increase symptoms such as facial flushing and skin itching. Protect your skin when you are outside in hot weather. Do not use a tanning bed or sun lamp. These can damage your skin.
- Take cool baths to relive itching. Itching can increase after a hot bath. Cool water may help relive itching. You may want to use oatmeal, corn starch, or a mild moisturizing soap to relieve dryness or itching. Lotion may also help relieve dry skin.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Polycythemia Vera
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
