Acute Pericarditis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is acute pericarditis?
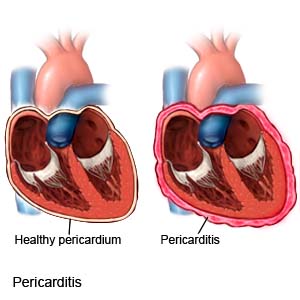
Acute pericarditis is inflammation of the pericardium. The pericardium is the thin sac that surrounds your heart. A small amount of clear fluid between the heart and the sac allows the heart to beat easily. With acute pericarditis, the amount of fluid increases and may contain pus. This can lead to problems with the way that your heart beats.
 |
What causes acute pericarditis?
The cause may not be known. Pericarditis may be caused by any of the following:
- Injuries or accidents that cause a hard blow to the chest and damage the sac
- Germs, such as viruses and bacteria, or an infection in another area of your body that spreads to the sac
- Medicines such as those used to treat high blood pressure, cancer, and infection
- Heart surgery or radiation therapy
- A heart attack that damages the heart muscle
- Fluid and chemical buildup in your body and around your heart from kidney failure
- Autoimmune diseases, cancer, or tuberculosis (TB) that damages the sac or increases the amount of fluid
- A growing baby during pregnancy that pushes on your heart and causes problems
What are the signs and symptoms of acute pericarditis?
The signs and symptoms may appear suddenly and worsen quickly. You may have any of the following:
- Pain in your chest that becomes worse when you lie down
- Fast heartbeat
- Shortness of breath
- Fever
- Feeling more tired than usual and getting tired easily
How is acute pericarditis diagnosed?
Your healthcare provider will examine you and ask you about medical problems that you have had in the past. He or she will listen to your heart. You may also have any of the following tests:
- Blood tests are used to give healthcare providers information about how your body is working.
- Telemetry is continuous monitoring of your heart rhythm. Sticky pads placed on your skin connect to an EKG machine that records your heart rhythm.
- X-ray pictures of your lungs and heart may be used to check the fluid around your heart. Chest x-rays may show signs of infection around your heart.
- An echocardiogram is a type of ultrasound. Sound waves are used to show the structure and function of your heart.
- Transesophageal echocardiogram (TEE) is a type of ultrasound that shows pictures of the size and shape of your heart. It also looks at how your heart moves when it is beating. You may also need a TEE to check for certain problems such as blood clots or infection inside the heart.
- CT scan or MRI pictures may be used to check the amount of fluid around your heart. You may be given contrast liquid before the pictures are taken. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with any metal objects. Metal can cause serious injury. Tell the provider if you have any metal in or on your body.
- Pericardiocentesis is a procedure used to drain extra fluid from the sac. The fluid is sent to a lab to be checked for infection.
- Pericardial biopsy is a procedure used to remove a small piece of the heart sac. The piece is sent to a lab for tests.
How is acute pericarditis treated?
- NSAIDs help decrease swelling and pain or fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Antibiotics help prevent or treat a bacterial infection.
- Steroid medicine helps lower inflammation.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to prevent infections?
The following can help prevent the spread of viruses and bacteria that can cause acute pericarditis or make it worse:
- Wash your hands often. Wash your hands several times each day. Wash after you use the bathroom, change a child's diaper, and before you prepare or eat food. Use soap and water every time. Rub your soapy hands together, lacing your fingers. Wash the front and back of your hands, and in between your fingers. Use the fingers of one hand to scrub under the fingernails of the other hand. Wash for at least 20 seconds. Rinse with warm, running water for several seconds. Then dry your hands with a clean towel or paper towel. Use hand sanitizer that contains alcohol if soap and water are not available. Do not touch your eyes, nose, or mouth without washing your hands first.

- Cover a sneeze or cough. Use a tissue that covers your mouth and nose. Throw the tissue away in a trash can right away. Use the bend of your arm if a tissue is not available. Wash your hands well with soap and water or use a hand sanitizer.
- Clean surfaces often. Clean doorknobs, countertops, cell phones, and other surfaces that are touched often. Use a disinfecting wipe, a single-use sponge, or a cloth you can wash and reuse. Use disinfecting cleaners if you do not have wipes. You can create a disinfecting cleaner by mixing 1 part bleach with 10 parts water.
- Ask about vaccines you may need. Vaccines help protect against viruses and bacteria that cause certain diseases. Your healthcare provider can tell you which vaccines you may need and when to get them.
- Get the influenza (flu) vaccine as soon as recommended each year. The flu vaccine is usually available starting in September or October. Flu viruses change, so it is important to get a flu vaccine every year.
- Ask your healthcare provider about the pneumonia vaccine. The vaccine is recommended for all adults aged 50 or older to prevent pneumococcal disease, such as pneumonia. Adults aged 19 to 49 years who are at high risk for pneumococcal disease should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors.
- COVID-19 vaccines are given to adults as a shot. At least 1 dose of an updated vaccine is recommended for all adults. COVID-19 vaccines are updated throughout the year. Adults 65 or older need a second dose of updated vaccine at least 4 months after the first dose. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
Related medications
When should I seek immediate care?
- You have shortness of breath that is worse when you lie down.
- Your chest pain gets worse or does not get better.
When should I call my doctor?
- You have a fever.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Acute Pericarditis
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
