Pericardial Effusion
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is pericardial effusion?
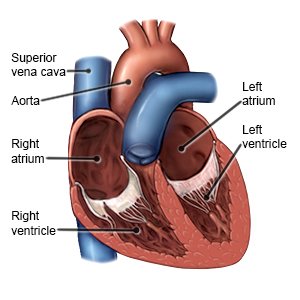
Pericardial effusion is a buildup of fluid in the pericardium. The pericardium is a 2-layer sac that surrounds the heart. The sac normally contains a small amount of clear fluid between its layers. This allows the heart to move smoothly against other organs in the chest as it beats. The fluid buildup puts pressure on your heart. This makes it difficult for your heart to pump. Fluid may collect slowly or quickly.
 |
What causes pericardial effusion?
The cause may be unknown, or it may be caused by any of the following:
- Diseases such as rheumatoid arthritis, cancer, hypothyroidism (low levels of thyroid hormone), or kidney failure
- Infections of the pericardium caused by viruses, bacteria, or parasites
- Inflammation of the pericardium, called pericarditis
- Injury or trauma that damages the pericardium, such as a puncture wound in the chest, or a heart attack
- Procedures such as heart surgery or radiation therapy near the heart
What are the signs and symptoms of pericardial effusion?
You may not have any symptoms, or you may have any of the following:
- Chest pain
- Cough
- Feeling lightheaded or faint
- Swelling of your legs and feet
- Shortness of breath, especially when lying down
- Trouble swallowing food
How is pericardial effusion diagnosed?
Your healthcare provider will ask about your health and the medicines you are taking. You may need any of the following tests:
- An EKG records your heart rhythm and how fast your heart beats. It is used to check for damage or problems in your heart.
- Blood tests may be done to look for signs of infection or other possible causes of pericardial effusion.
- A chest x-ray is a picture of your lungs and heart. Chest x-rays may show fluid around the heart and lungs.
- An echocardiogram is a type of ultrasound. Sound waves are used to show the structure and function of your heart.
- A CT or MRI scan takes pictures of your chest. The pictures may show fluid around your heart or other problems. You may be given contrast liquid to help your heart show up better in pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- A sample of fluid from the pericardial sac may be taken with a needle. The fluid is sent to a lab for tests.
Related medications
How is pericardial effusion treated?
Treatment depends on the cause of your pericardial effusion. You may need any of the following:
- Antibiotics help treat an infection caused by bacteria.
- Steroids help decrease swelling.
- NSAIDs help decrease swelling and pain or fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Pericardial drainage relieves pressure on your heart so it can pump normally. A catheter is inserted into the pericardium to drain fluid.
- A balloon procedure is another way to drain extra fluid. A needle is put into the pericardium and a guidewire is threaded through the needle. The needle is then removed. A catheter with a balloon at its end is passed over the guidewire into the correct position in the pericardium. The balloon is inflated and deflated several times to create an opening for the fluid to drain out.
- Surgery may be done to remove part or most of the pericardium.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Call your local emergency number (911 in the US) if:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have sudden chest pain.
- You have sudden trouble breathing.
When should I seek immediate care?
- You feel lightheaded or faint.
- You have swelling in your legs or feet.
When should I call my doctor?
- You have a fever.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Pericardial Effusion
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
