Liver Resection
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Liver resection is surgery to remove part of your liver.
 |
DISCHARGE INSTRUCTIONS:
Call your local emergency number (911 in the US) if:
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
Seek care immediately if:
- You are not able to eat, and you lose weight.
- You have foul-smelling drainage coming from your surgery area.
- You have severe abdominal pain.
- You have yellowing of your skin or the whites of your eyes.
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Blood soaks through your bandage.
Call your doctor or surgeon if:
- You have a fever.
- You have pain in the surgery area that does not get better with rest or medicine.
- Your skin near the surgery area is red, warm, and swollen.
- Your stitches come loose.
- You have questions or concerns about your condition or care.
Medicines:
You may need any of the following:
- Antibiotics help treat or prevent an infection caused by bacteria.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Take your medicine as directed. Contact your healthcare provider if you think your medicine is not helping or if you have side effects. Tell your provider if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow-up visits. Carry your medicine list with you in case of an emergency.
Related medications
Care for the surgery area:
Follow your healthcare provider's instructions about how to care for the area. Check for signs of infection, such as red streaks, swelling, or pus.
Take deep breaths and cough 10 times each hour.
This will decrease your risk for a lung infection. Take a deep breath and hold it for as long as you can. Let the air out and then cough strongly. Deep breaths help open your airway. You may be given an incentive spirometer to help you take deep breaths. Put the plastic piece in your mouth and take a slow, deep breath, then let the air out and cough. Repeat these steps 10 times every hour.
Prevent blood clots:
Surgery can increase the risk that blood clots will form in a major vein in your leg or arm. The following can help prevent blood clots:
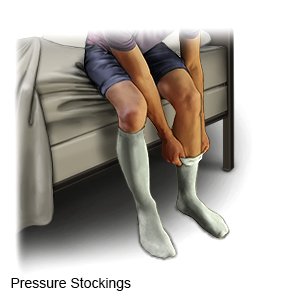
- Compression stockings are tight elastic stockings that put pressure on your legs. The pressure is highest in the toe area and decreases as it goes toward your thighs. Pressure stockings help push blood back up to your heart and keep clots from forming.
- Walking may help prevent a blood clot and decrease your risk for a lung infection.

Activity:
Ask when you can return to your normal activities, such as work and school.
For more information:
- American Liver Foundation
39 Broadway Suite 2700
New York , New York 10006
Phone: 1- 212 - 668-1000
Phone: 1- 800 - 465-4837
Web Address: http://www.liverfoundation.org
Follow up with your doctor or surgeon as directed:
You may need to return for more tests. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
