Iron Deficiency Anemia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is iron deficiency anemia (IDA)?
IDA happens when your body does not have enough iron to make hemoglobin. This means you will have low hemoglobin and red blood cell levels. Hemoglobin is part of red blood cells and helps carry oxygen throughout your body. Blood loss and not eating enough foods that contain iron are common causes of low iron.
What increases my risk for IDA?
- Blood loss may reduce iron levels in your blood over time. Ways you may lose blood include:
- A female's monthly period
- Trauma or bleeding in your intestines
- Hemorrhoids
- Donating blood more than 5 times a year
- Pregnancy increases the amount of iron your body needs.
- Low-iron diet such as a strict vegan or vegetarian diet.
- Digestive conditions such as Celiac disease, chronic diarrhea or Crohn disease may interfere with how your body absorbs iron from your food.
- Medicines may prevent your body from absorbing iron from your food. NSAIDs such as ibuprofen or aspirin may cause bleeding in your intestines.
What are the signs and symptoms of IDA?
- Feeling weak, tired, or irritable
- Pale skin, cold hands, and feet
- Headache, dizziness
- Shortness of breath with activity or chest pain
- Fast or uneven heartbeat
- Sore or swollen tongue and mouth
- Nails that break easily
- An urge to eat things that are not food such as ice, paint, starch, or dirt
How is IDA diagnosed?
- Blood tests will show how much iron is in your blood and how your body uses the iron.
- A bowel movement sample will show any blood in your bowel movement.
- An endoscopy may show bleeding in your esophagus or stomach. An endoscope is a bendable tube with a light and camera on the end. It is put into your esophagus through your mouth and throat.
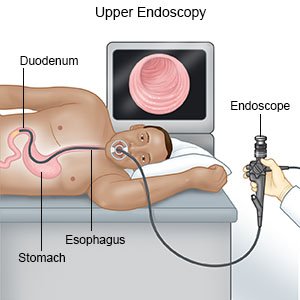
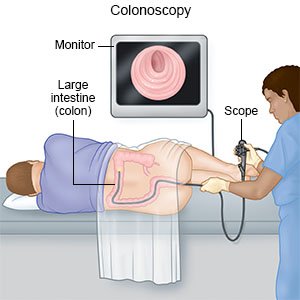
- A colonoscopy may show bleeding in your intestines. A scope is put into your rectum.
Related medications
How is IDA treated?
Treatment depends on the cause of your IDA and may take 3 to 6 months. You may need any of the following:
- Medicines and supplements may increase the amount of iron in your blood. Ask your healthcare provider how much iron you should take each day. Tell your provider about all medicines you currently take.
- Iron infusions replace iron in your body through an IV in one of your veins. Your provider will tell you if an iron infusion is right for you.
- A blood transfusion may be needed if your anemia is severe. This will help replace the blood and iron you have lost.
- Surgery may be needed if your IDA is caused by bleeding in your intestines.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my symptoms?
- Take iron supplements with vitamin C. Taking your iron supplement with food or drinks high in vitamin C helps your body absorb iron.

- Eat foods rich in iron and protein. Nuts, meat, dark leafy green vegetables, and beans are high in iron and protein. Limit milk to 2 cups a day. The calcium in milk can interfere with how your body absorbs iron. You may need to meet with a dietitian to create the right food plan for you.
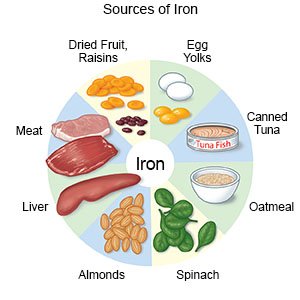

- Drink liquids as directed. Iron supplements may cause constipation. Liquids help prevent constipation. Ask how much liquid to drink each day and which liquids are best for you.
When should I seek immediate care?
- You have dark or bloody bowel movements.
- You vomit blood.
- You are too dizzy to stand up.
- You have trouble swallowing because of the pain in your mouth and throat.
When should I call my doctor?
- You have heartburn, constipation, or diarrhea.
- You have nausea or are vomiting.
- You are dizzy or very tired.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Iron Deficiency Anemia
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
