Stomach Cancer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about stomach cancer?
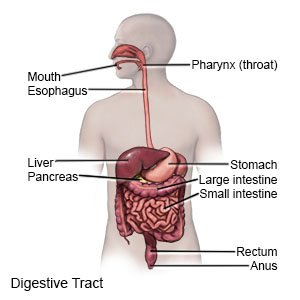
Most stomach cancer starts in the cells that line the stomach but may form anywhere in the stomach. It is also called gastric cancer.
 |
What increases my risk for stomach cancer?
- Age older than 60 years
- Intestinal metaplasia (cells like intestine cells grow in your stomach)
- Regularly eating smoked, salt-cured, or pickled foods, such as bacon, ham, or corned beef
- Not eating many fruits or vegetables
- Extra body weight
- A family history of colon cancer
- A stomach condition, such as stomach ulcers caused by bacteria
- Stomach surgery
- Cigarette smoking
What are the signs and symptoms of stomach cancer?
- Heartburn, nausea, vomiting, or stomach pain
- Loss of appetite
- Diarrhea or constipation
- Unexplained weight loss
- Feeling bloated or full even after a small meal
- Trouble swallowing food
- Blood in your vomit or bowel movement
How is stomach cancer diagnosed?
- Blood tests may be used to check for anemia (lack of red blood cells). Stomach cancer can cause anemia to develop.
- A bowel movement sample may be checked for blood.
- An x-ray, ultrasound, or CT may show the size and location of the tumor or if the cancer has spread. You may be given contrast liquid to help the tumor show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- Barium is a substance that helps your stomach and intestines show up better in x-rays. You may need to eat a meal that has barium in it. An x-ray machine is then used to take pictures of your stomach. Healthcare providers watch the pictures to see how your stomach digests the meal.
- An endoscopy is a procedure used to find problems with how your digestive tract is working. A scope is used to see the inside of your digestive tract. A scope is a long, bendable tube with a light and camera on the end of it. Samples may be taken from your digestive tract and sent to a lab for tests. Small tumors may be removed, and bleeding may be treated during an endoscopy.
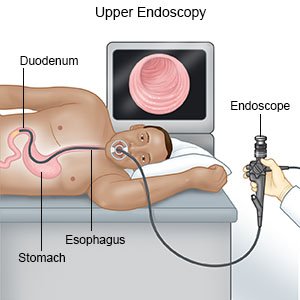
How is stomach cancer treated?
- Surgery called gastrectomy may be used to remove part or all of your stomach.
- Chemotherapy is medicine to kill cancer cells. Chemotherapy may also be used to shrink lymph nodes that contain cancer.
- Radiation therapy uses x-rays or gamma rays to kill cancer cells and may stop the cancer from spreading.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Related medications
What can I do to manage stomach cancer?
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can make it more difficult to manage stomach cancer. Smoking also increases your risk for new or returning cancer and delays healing after treatment. Do not use e-cigarettes or smokeless tobacco in place of cigarettes or to help you quit. They still contain nicotine. Ask your healthcare provider for information if you currently smoke and need help quitting.
- Eat healthy foods. Increase the amount of fruits and vegetables you eat. Other healthy foods include whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Limit foods such as salami, corned beef, ham, and bacon. A dietitian may work with you to help reduce symptoms.

- Drink liquids as directed. Ask how much liquid to drink each day and which liquids are best for you. Drink extra liquids to prevent dehydration. You will also need to replace fluid if you are vomiting or have diarrhea from cancer treatments.
- Do not drink alcohol. Alcohol can cause more stomach damage.
- Exercise as directed. Exercise can help increase your energy level and appetite. Ask your provider how much exercise you need and which exercises are best for you.

Where can I find support and more information?
- American Cancer Society
250 Williams Street
Atlanta , GA 30303
Phone: 1- 800 - 227-2345
Web Address: http://www.cancer.org
Call your local emergency number (911 in the US) for any of the following:
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
When should I seek immediate care?
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- You are vomiting and cannot keep food or liquids down.
- You are dizzy or feel confused.
When should I call my doctor?
- You have a fever.
- Your pain is worse or does not go away after you take pain medicine.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Stomach Cancer
Treatment options
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
