Refractive Errors of the Eye
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What are refractive errors of the eye?
Refractive errors of the eye are common vision disorders. These disorders happen when there is a problem with how your eye bends and focuses light. Refractive errors are caused by abnormal shape and texture of your eye.
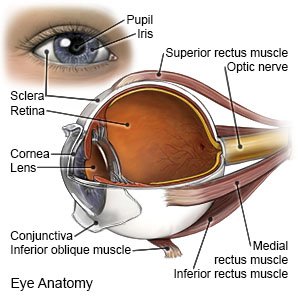 |
What increases my risk for a refractive error?
- A family history of refractive errors, especially if both parents have a refractive error
- Eye strain, such as reading in dim light or overworking your eyes
- Eye trauma or eye surgery that changes or damages the cornea and lens
- An abnormally thin cornea, dislocated or small lenses
- A condition such as diabetes that can change the shape of your eye
What signs and symptoms may I have with different types of refractive errors?
The most common symptom is blurry vision. You may rub, shut, or cover one eye, squint, or tilt or turn your head often. You may also have eye strain, headache, or fatigue. You may have other symptoms based on your type of refractive error:
- Astigmatism means the cornea does not have the normal round shape. The irregular curves makes the eye shaped more like a spoon or football. Astigmatism may be present at birth and may happen along with hyperopia or myopia. Astigmatism causes both near and far objects to appear as deformed images. Straight lines may appear wavy.
- Hyperopia is also called hypermetropia, or farsightedness. Hyperopia occurs when the eyeball is too short or the cornea is a little flat or less curved. This causes light rays entering the eye to focus behind the retina. Hyperopia causes distant objects to be seen clearly, but close or near objects are blurred.
- Myopia is also known as nearsightedness. Myopia usually occurs between 5 to 15 years of age. The eyeball is too long or the cornea is too curved or rounded. This causes the light rays to focus in front of the retina. Myopia causes close objects to look clear, but far objects are blurred.
- Presbyopia is common in adults 40 years or older. Presbyopia happens when the lens becomes stiff and less flexible. This causes the lens to lose its ability to bend or change shape. The lens cannot move and is not able to bring nearby objects into focus. Presbyopia prevents objects from being clear up close. You may need to hold reading material at arm's length in order to read it.
- Esotropia is a form of strabismus, also called squint or cross-eyed, where the eyes may not be aligned. One eye may turn inward while the other focuses normally. Your eyes do not look in the same direction at the same time.
- Anisometropia happens when you have different bending power between the 2 eyes. One eye may have myopia, and the other eye may have hyperopia.
How are refractive errors diagnosed?
Your healthcare provider may ask about your symptoms, medical history, and medicines. He or she may do a series of tests that aim bright lights directly at your eyes. You may also need any of the following tests:
- A cover-uncover test checks if your eyes are aligned. An object is placed at a certain distance far away from you while one eye is covered. Your healthcare provider carefully looks at the uncovered eye for any movement.
- A test for fixation checks how well your uncovered eye follows the light. One eye is covered while your healthcare provider moves a small flashlight in front of you. He or she repeats the test on the other eye and compares the results.
- A refraction test checks the lens of your eyes. You will be asked to look at a chart through a device that has lenses of different strengths. You will be asked if the word or picture is clear as he or she changes the lenses.
- A visual acuity test checks your ability to see clearly. You will be shown charts with letters, pictures, and shapes. Your healthcare provider may ask you to read eye charts placed farther down the room from you. These charts help your healthcare provider check how well you see colors and lines at different distances.
How are refractive errors treated?
- Contact lenses and glasses help correct the shape of your eyes. This helps light to focus correctly and improves your vision.
- You may need eyedrops or ointments. These decrease inflammation, help your eyes focus, and can make your eye muscles stronger.
- You may need surgery to reshape the curve of your cornea. There are different types of refractive surgery to treat refractive errors. Your vision may be corrected by a laser. Your healthcare provider may place tiny plastic rings into the cornea. Ask your healthcare provider for more information on refractive surgery.
What can I do to care for my eyes?
- Get regular eye exams. Get your eyes checked at least every year.
- Eat healthy foods. Fresh fruits and vegetables that are rich in vitamins A and C may help with your vision. Foods such as sweet potatoes, apricots, and carrots are rich in good nutrients for the eyes.
- Take care of your contacts or glasses. Store, clean, and use your contacts or glasses as directed. Replace your glasses or contact lenses as often as your healthcare provider suggests.
- Decrease eye strain. Rest your eyes, especially after you read or sew for long periods of time. Get plenty of sleep at night. Use lights that reduce glare in your home, school, or workplace.
- Wear dark sunglasses. This will help prevent pain and light sensitivity. Make sure the sunglasses have UVA and UVB protection. This will protect your eyes when you go outside.
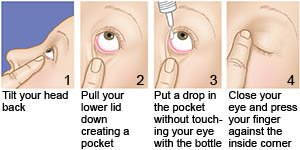
- Use eyedrops safely. If your treatment plan includes eyedrops, it is important to use them as directed. Your provider may give you detailed instructions to follow. The eyedrops may also come with safety instructions. Follow all instructions to help prevent an infection. Do not touch the tip of the bottle to your eye. Germs from your eye can spread to the medicine bottle.
When should I call my healthcare provider or ophthalmologist?
- You have a headache that does not go away, even after treatment.
- You have a sudden loss of vision.
- You have changes in your eyesight.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
