Bacterial Pneumonia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is bacterial pneumonia?
Bacterial pneumonia is a lung infection caused by bacteria. Your lungs become inflamed and cannot work well. Bacterial pneumonia germs are easily spread when an infected person coughs, sneezes, or has close contact with others.
 |
What increases my risk for bacterial pneumonia?
- A cold or the flu
- Recent hospitalization
- Use of a ventilator to help you breathe
- Older age
- Smoking
- A large amounts of alcohol
- Health conditions, such as heart or lung disease
- A weakened immune system caused by HIV, cancer, or steroid use
What are the signs and symptoms of bacterial pneumonia?
- Dry cough or coughing up mucus, which may be streaked with blood
- Fever or chills
- Shortness of breath, wheezing, or chest pain
- Feeling tired easily
- Fast heartbeat
- Headache, muscle pain, or abdominal pain or discomfort
How is bacterial pneumonia diagnosed?
Your healthcare provider will ask about your signs and symptoms and examine you. You may need any of the following tests:
- Pulse oximetry measures the amount of oxygen in your blood.

- Blood tests are used to check for infection.
- A chest x-ray may show signs of infection in your lungs.
- A mucus sample is collected and tested for the germ that is causing your illness. It can help your healthcare provider choose the best medicine to treat the infection.
How is bacterial pneumonia treated?
Treatment depends on what caused your bacterial pneumonia and how bad your symptoms are. You may need any of the following:
- Antibiotics help treat a bacterial infection.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Airway clearance techniques are exercises to help remove mucus so you can breathe more easily. Your healthcare provider will show you how to do the exercises. These exercises may be used along with machines or devices to help decrease your symptoms.
- Respiratory support is given to help you breathe. You may receive oxygen to increase the level of oxygen in your blood. You may also need a machine to help you breathe.
How can I manage bacterial pneumonia?
- Rest as needed. Rest often while you recover. Slowly start to do more each day.
- Keep your head elevated. You may be able to breathe better if you keep your head and upper body elevated.
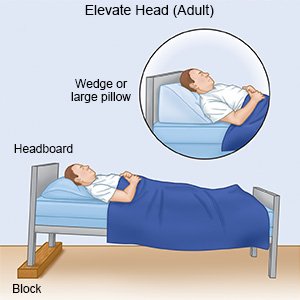
- Do not smoke. Smoking increases your risk for pneumonia. Smoking also makes it harder for you to get better after you have had pneumonia. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products. Avoid secondhand smoke.
- Drink liquids as directed. Ask how much liquid to drink each day and which liquids are best for you. Liquids help thin your mucus, which may make it easier for you to cough it up.
- Use a cool mist humidifier to increase air moisture in your home. This may make it easier for you to breathe and help decrease your cough.
What can I do to prevent bacterial pneumonia?
- Prevent the spread of germs. Wash your hands often with soap and water. Use gel hand cleanser when there is no soap and water available. Do not touch your eyes, nose, or mouth unless you have washed your hands first. Cover your mouth when you cough. Cough into a tissue or your shirtsleeve so you do not spread germs from your hands. If you are sick, stay away from others as much as possible.
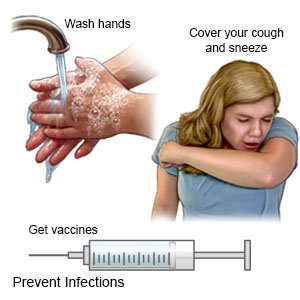
- Ask about vaccines you may need. Your healthcare provider can tell you if you should also get vaccines other than those listed below, and when to get them:
- Get an influenza (flu) vaccine as directed. The flu vaccine is recommended for everyone 6 months or older. Get the vaccine as soon as recommended each year, usually in September or October.
- Get a COVID-19 vaccine as directed. At least 1 dose of an updated vaccine is recommended for everyone 6 months or older. COVID-19 vaccines are given as a shot in 1 to 3 doses, depending on the age of the person who receives it. COVID-19 vaccines are updated throughout the year. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
- Get a pneumonia vaccine as directed. The vaccine is recommended for all adults aged 50 or older. Adults aged 19 to 49 years who are at high risk for pneumonia should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors. Children routinely receive 4 doses of the pneumonia vaccine, starting at 2 months.
- Limit or do not drink alcohol. Large amounts can lead to pneumonia. Alcohol can also cause or worsen dehydration. Women should limit alcohol to 1 drink a day. Men should limit alcohol to 2 drinks a day. A drink of alcohol is 12 ounces of beer, 5 ounces of wine, or 1½ ounces of liquor.
Call your local emergency number (911 in the US) or have someone call if:
- You are confused or cannot think clearly.
When should I seek immediate care?
- You are urinating less or not at all.
- You cough up blood.
- You have more trouble breathing, or your breathing seems faster than normal.
- Your heart or pulse beats more than 100 times in 1 minute.
- Your lips or fingernails turn blue.
When should I call my doctor?
- Your symptoms are the same or get worse 48 hours after you start antibiotics.
- You cannot eat, you have loss of appetite or nausea, or you are vomiting.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Bacterial Pneumonia
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
