Viral Pneumonia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is viral pneumonia?
Viral pneumonia is a lung infection caused by a virus, such as those that cause the flu or COVID-19. You can get a viral infection by breathing in the virus or by touching something that has the virus on it. Viral pneumonia can develop if a virus in your body travels to your lungs. Your risk for viral pneumonia is higher if you are older than 65 or have lung or heart disease. Your risk is also higher if you have a weakened immune system.
 |
What are the signs and symptoms of viral pneumonia?
Signs and symptoms may develop slowly over several days. Your signs and symptoms may be different if you are older than 65 years. You may be confused or have aches and pains instead of the following more typical symptoms:
- Cough, which may or may not bring up mucus
- Fever above 100.4°F (38°C) or chills
- Shortness of breath, rapid breathing, or wheezing
- Muscle pain and tiredness
- Chest pain when you cough or breathe deeply
- Nausea and vomiting
- Headache
How is viral pneumonia diagnosed?
Your healthcare provider will ask about your signs and symptoms and examine you. Your provider will listen to your heart and lungs. Tell your provider if you have been around anyone who is sick. You may need any of the following:
- A chest x-ray may show signs of infection in your lungs.
- A mucus sample is collected and tested for the virus that caused your pneumonia. Your healthcare provider may swab your throat or the inside of your nose to get a mucus sample. You may be asked to cough mucus into a cup.
- Blood tests may show signs of an infection.
How is viral pneumonia treated?
Most people with viral pneumonia are treated at home. Older adults and people with health problems may need to stay in the hospital. You may need any of the following:
- Antiviral medicine is given to treat an infection caused by a virus. Antivirals work best if taken within 72 hours of infection. After 72 hours, the medicine can still help shorten the amount of time you have the virus, or reduce your symptoms.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Airway clearance techniques are exercises to help remove mucus so you can breathe more easily. Your healthcare provider will show you how to do the exercises. These exercises may be used along with machines or devices to help decrease your symptoms.
- Respiratory support is given to help you breathe. You may receive oxygen to increase the level of oxygen in your blood. You may also need a machine to help you breathe.
How can I manage my symptoms?
- Rest as needed. Rest often while you recover. Slowly start to do more each day.
- Drink liquids as directed. Ask how much liquid to drink each day and which liquids are best for you. Liquids help thin your mucus, which may make it easier for you to cough it up.
- Do not smoke. Avoid secondhand smoke. Smoking makes it harder for you to get better. Nicotine and other chemicals in cigarettes and cigars can cause lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Use a cool mist humidifier. A humidifier will help increase air moisture in your home. This may make it easier for you to breathe and help decrease your cough.
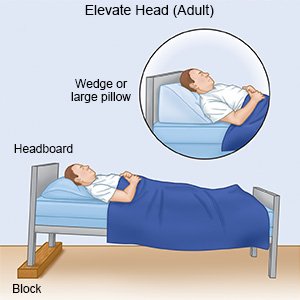
- Keep your head elevated. You may be able to breathe better if you keep your head and upper back elevated.
How can I prevent viral pneumonia?
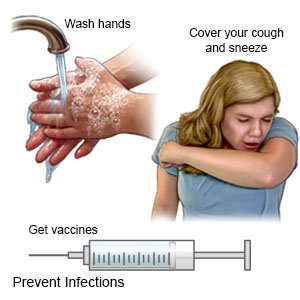
- Prevent the spread of germs. Wash your hands often with soap and water. Use hand sanitizer if soap and water are not available. Do not touch your eyes, nose, or mouth unless you have washed your hands first. Cover your mouth when you cough. Cough into a tissue or the bend of your arm so you do not spread germs from your hands. If you are sick, stay away from others as much as possible.
- Ask about vaccines you may need. Your healthcare provider can tell you if you should also get vaccines not listed below:
- Get an influenza (flu) vaccine as directed. The flu vaccine is recommended for everyone 6 months or older. Get the vaccine as soon as recommended each year, usually in September or October.
- Get a COVID-19 vaccine as directed. At least 1 dose of an updated vaccine is recommended for everyone 6 months or older. COVID-19 vaccines are given as a shot in 1 to 3 doses, depending on the age of the person who receives it. COVID-19 vaccines are updated throughout the year. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
- Get a pneumonia vaccine as directed. The vaccine is recommended for all adults aged 50 or older. Adults aged 19 to 49 years who are at high risk for pneumonia should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors. Children routinely receive 4 doses of the pneumonia vaccine, starting at 2 months.
 |
When should I seek immediate care?
- You have more trouble breathing or your breathing seems faster than normal.
- Your lips or fingernails turn blue.
- You are confused and cannot think clearly.
- You are urinating less or not at all.
When should I call my doctor?
- Your symptoms are not getting better or are getting worse, even after treatment.
- You have questions or concerns or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Viral Pneumonia
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
