Hematuria
Medically reviewed by Drugs.com. Last updated on Jan 29, 2024.
What is hematuria?

Hematuria is the presence of red blood cells in the urine. If there are enough red cells, the urine can become bright red, pink or cola colored. Often, however, the urine appears completely normal because there is not enough blood to cause a color change. In this case, the condition is called "microscopic" hematuria.
There are many possible causes of hematuria, including:
- Urinary tract infection — Hematuria can be caused by an infection in any part of the urinary tract, most commonly the bladder (cystitis) or the kidney (pyelonephritis).
- Kidney stones
- Tumors in the kidney or bladder
- Exercise — Exercise hematuria is a harmless condition that produces blood in the urine after strenuous exercise. It is more common in males than females.
- Trauma — Traumatic injury to any part of the urinary tract — from the kidneys to the urethral opening (the connection between the bladder and the outside world) — can cause hematuria.
- Drugs — Hematuria can be caused by medications, such as blood thinners, including heparin, warfarin (Coumadin) or aspirin-type medications, penicillins, sulfa-containing drugs and cyclophosphamide (Cytoxan).
- Glomerulonephritis — Glomerulonephritis is a family of illnesses that are characterized by inflammation of the glomeruli, the filtering units of the kidneys. Glomerulonephritis is a rare complication of certain viral and bacterial infections (including strep throat). It can also occur in people with certain auto-immune diseases, systemic lupus erythematosus (lupus or SLE) and vasculitis. Sometimes there is no identifiable cause.
- Bleeding disorders — This includes conditions such as hemophilia and von Willebrand's disease.
Symptoms of hematuria
By itself, hematuria rarely causes symptoms. One exception is when the bladder has so much blood in it that clots form, and the flow of urine is blocked. This can cause pain at the site of the blockage in the lower pelvis. Symptoms usually come from the cause of the hematuria, and vary depending on the condition:
- Glomerulonephritis — If glomerulonephritis is not severe, it may not cause any symptoms. If symptoms appear, they can include swelling, especially in the lower extremities, reduced urination, and high blood pressure.
- Kidney or bladder infection — Symptoms depend on the site of infection, but can include intense pain on one side of the mid-back, fever, shaking chills, nausea and vomiting, pain above the pubic or bladder region, foul-smelling urine, the need to urinate more often than normal, and pain or discomfort during urination.
- Prostate infection — There can be pain in the lower back or in the area between the scrotum and anus, pain during ejaculation, blood in the semen, and, sometimes, fever and chills.
- Tumor in the kidney or bladder —Most kidney and bladder cancers grow without causing any pain or discomfort. When symptoms develop, the most common are abdominal pain, more frequent urination and pain at the end of urination.
- Kidney stones — When a kidney stone becomes trapped in one of the ureters (the narrow tubes connecting each kidney to the bladder), it can cause severe pain in the back, side or groin, nausea and vomiting, or painful and frequent urination.
- Bleeding disorders — Bleeding disorders tend to cause abnormal bleeding throughout the body, not just into the urine. Depending on the specific bleeding problem, symptoms can include abnormal bruising, prolonged bleeding from cuts, bleeding in the skin, bleeding into the joints or gastrointestinal tract (causing black, tarry stools or bright red blood in the stool), or gum bleeding even with gentle flossing or brushing.
- Trauma — There often will be signs of traumatic injury to the body surface, such as bruises, swelling, punctures and open wounds.
Diagnosis
Your health care professional will want a sample of your urine to confirm that you have hematuria. In women, blood can get into the urine during menstruation. Your doctor may want to repeat the urine test between periods.
Once your doctor has confirmed that you have hematuria, he or she will ask about your medical history and your family's medical history, especially any history of kidney disease, bladder problems or bleeding disorders. Your doctor also will ask about any recent trauma or strenuous exercise, recent viral or bacterial infections, the medications you take, and your symptoms, including more frequent urination, pain with urination and pain in your side.
Your doctor also will examine you. He or she will take your temperature and blood pressure, and will see if you have pain or discomfort in your side or over your bladder. The doctor may recommend that women undergo a pelvic examination, and men undergo a prostate examination.
Your doctor will ask you for a fresh urine sample for a urinalysis. Urine is analyzed in the laboratory to look for protein, white cells and red cells to identify a kidney or bladder infection, or kidney inflammation (glomerulonephritis).
Then, depending on the suspected cause of your hematuria, additional testing may include:
- Urine culture — In this test, a sample of urine is monitored to see if bacteria grow. This test is used to confirm a kidney or bladder infection.
- CT scan of the kidneys, ureters and bladder— Most often the computerized tomographic (CT) scan is done without intravenous contrast first. If additional information is still needed, the radiologist may want to inject a dye (also called a contrast medium) into an arm vein. The dye collects in the kidneys and is excreted in the urine, providing an outline of the entire urinary system. Tell the radiologist about your allergies, especially any previous reaction to contrast medium.
- Ultrasound — This test uses sound waves to help establish whether a kidney mass is a noncancerous (benign), fluid-filled cyst or a solid mass, such as a cancerous tumor. Ultrasound also can identify kidney stones.
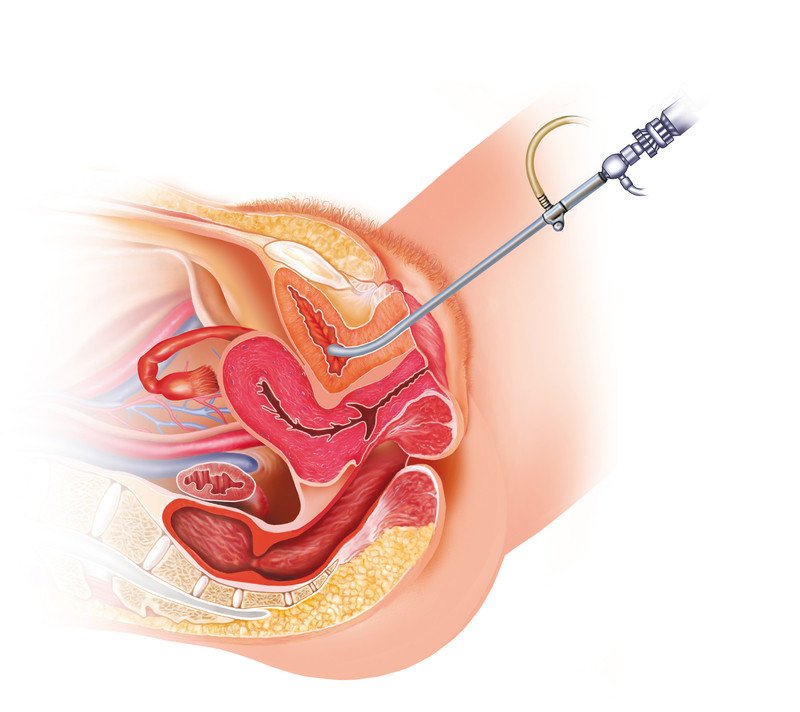
- Cystoscopy — In this test, the doctor inserts a flexible telescope into the urethra and passes it into the bladder to inspect the bladder lining for tumors or other problems. This test usually is done with local anesthesia and sedation.
|
|
- Blood tests — These can check for signs of urinary tract infection, kidney failure, anemia (which often accompanies kidney problems), bleeding disorders, or abnormally high levels of blood chemicals that can encourage the formation of kidney stones.
Additional testing for conditions causing kidney inflammation (such as lupus) may be recommended, depending on the findings of the routine blood and urine tests.
Expected duration of hematuria
How long hematuria lasts depends on its underlying cause. For example, hematuria related to strenuous exercise typically goes away on its own within 24 to 48 hours. Hematuria resulting from a urinary tract infection will end when the infection is cured. Hematuria related to a kidney stone will clear after the stone is passed or removed.
Preventing hematuria
To prevent hematuria related to strenuous exercise, switch to a less-intense exercise program. In general, you can help to prevent other forms of hematuria by following a lifestyle that fosters a healthy urinary tract:
- Stay well hydrated. Drink about eight glasses of fluid daily (more during hot weather).
- Avoid smoking cigarettes, which are linked to urinary tract cancers.
Treating hematuria
The treatment of hematuria depends on its cause. In general, people with exercise-related hematuria do not need any treatment other than to modify their exercise programs. People with drug-related hematuria will improve if they stop taking the medication that caused the problem. Antibiotics typically will cure infection-related hematuria. For other causes of hematuria, treatment may be more complex:
- Urinary tract infection — Bladder infections can be treated with a very short course of antibiotics. For kidney infections, doctors typically prescribe a seven to 10 day course.
- Kidney stones — Smaller stones sometimes can be flushed from the urinary tract by drinking lots of fluids. Larger stones may require surgery or lithotripsy, a procedure that breaks up the stone.
- Trauma — Treatment depends on the type and severity of injuries. In severe cases, surgery may be necessary.
- Tumor in bladder or kidney — Treatment is determined by the type of cancer and how much the cancer has spread (its stage), as well as by the patient's age, general health and personal preferences. The primary types of treatment are surgery, chemotherapy, radiation therapy and immunotherapy, a type of treatment that stimulates the immune system to fight cancer.
- Glomerulonephritis — Treatment may include antibiotics to treat any infection, medications called diuretics that help to increase the amount of urine excreted from the body, and medications to control high blood pressure if needed. However, children who develop glomerulonephritis related to a streptococcal infection often recover after antibiotics without needing additional treatment. If it is caused by an autoimmune disorder, such as lupus, medications to suppress the immune system, are usually prescribed.
- Bleeding disorders — Treatment depends on the specific type of bleeding disorder. Patients with hemophilia can be treated with infusions of clotting factors or with fresh frozen plasma, a type of transfusion that provides missing factors.
When to call a professional
Call your doctor immediately if you notice blood in your urine or if your urine turns the color of cola. You should also call your health care professional if you have fever or pain in the lower abdomen or side.
Prognosis
Most people whose hematuria is related to exercise, medication, kidney stones, urinary tract infection or prostatitis have an excellent outlook for complete recovery.
Children with hematuria resulting from glomerulonephritis usually recover completely if their illness is mild or if it develops after a strep infection. Adults with glomerulonephritis are less likely to recover on their own, although the outlook depends on the specific type of glomerulonephritis. More severe forms of the disease eventually can lead to chronic kidney failure.
For people with kidney or bladder cancer, the outlook depends on the stage and type of tumor. In general, if a kidney or bladder tumor is diagnosed early, the cancer often can be cured.
Although people with hemophilia may have repeated bleeding episodes (including bleeding into joints, internal organs and other parts of the body), recent advances in treatment have achieved a near-normal lifespan for many patients.
Additional info
National Institute of Diabetes and Digestive and Kidney Disorders
https://www.niddk.nih.gov/
National Kidney Foundation
https://www.kidney.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.