Orbital Cellulitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
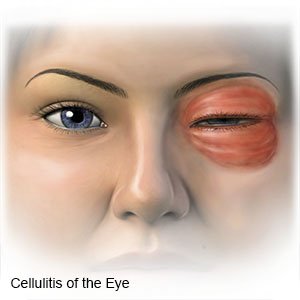
What is orbital cellulitis?
Orbital cellulitis is a bacterial infection of your eye and the tissue around your eye. The nerves that go to the eye are also infected. Orbital cellulitis is a serious condition that can lead to blindness.
 |
What causes orbital cellulitis?
- A sinus infection
- Infection of the teeth, ear, or face
- Trauma to the eye
- An animal or insect bite
- A foreign object
What are the signs and symptoms of orbital cellulitis?
- Red, swollen, painful eye and eyelid
- Bulging eyeball
- Painful eye movements
- Trouble moving your eye
- Blurred, double, or loss of vision
- A fever
How is orbital cellulitis diagnosed?
Your healthcare provider will check your vision, eye movement, and eye pressure. You may also need any of the following:
- Blood tests may show what bacteria is causing your infection.
- A sample of fluid or tissue from your eye or sinuses may show the cause of your infection. A sample may also show what areas are infected and what antibiotic would work best for treatment.
- A CT or MRI may show an abscess, rupture (tear), a blood clot, or other problems. You may be given contrast liquid to help your eye show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
How is orbital cellulitis treated?
You will need to stay in the hospital to treat orbital cellulitis. You may need any of the following:
- Medicines:
- Antibiotics treat the bacterial infection. Antibiotics are given through an IV.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor's order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask if NSAIDs are safe for you. Always read the medicine label and follow directions. Do not give these medicines to children younger than 6 months without direction from a healthcare provider.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Steroids help decrease redness and swelling of your eye.
- Surgery may be needed if your infection is severe and your vision is damaged. Surgery is also needed if an abscess or nasal sinus needs to be drained, or to remove a foreign object.
How can I manage my symptoms?
- Do not rub or scratch your eyes. This can increase your risk for spreading the infection.
- Place a cool, damp cloth on the area. Use clean cloths and clean water. You can do this as often as you need to. Cool, damp cloths may help decrease pain.
- Wash your hands often. Use soap and water. Wash your hands after you use the bathroom, change a child's diapers, or sneeze. Wash your hands before you prepare or eat food. Use lotion to prevent dry, cracked skin.

How can an eye infection be prevented?
- Wear proper safety equipment. Protect your face from injury during sports and other activities.
- Keep wounds clean and dry. Clean wounds on the face with soap and water. Cover wounds with a dry bandage if needed.
Call your local emergency number (911 in the US) if:
- You feel confused or more sleepy than usual.
- You develop a headache and are vomiting.
- You have a stiff neck.
When should I seek immediate care?
- You see red streaks coming from the infected area.
- You lose vision in your infected eye.
- You cannot close your eye due to swelling.
When should I call my doctor?
- The red, warm, swollen area gets larger.
- Your fever or pain does not go away or gets worse.
- You have questions about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Orbital Cellulitis
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
