Leg Fracture
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about a leg fracture?
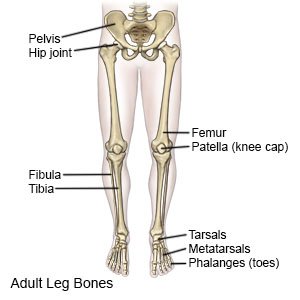
A leg fracture is a break in a bone in your leg.
 |
What are the signs and symptoms of a leg fracture?
- Pain that worsens when you stand on or move your leg
- Trouble moving your leg
- Leg position or shape that is not normal
- Swelling or bruising
- Weakness or loss of feeling in your leg
How is a leg fracture diagnosed?
Your healthcare provider will ask how you injured your leg. He or she will examine your leg. He or she may touch areas of your leg to see if you have decreased feeling. The provider will also check for any open breaks in the skin. You may need an x-ray, ultrasound, CT, or MRI. Contrast liquid may be used to help the fracture show up better in pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
How is a leg fracture treated?
Treatment depends on what kind of fracture you have and how bad it is. You may need any of the following:
- A brace, cast, or splint will decrease leg movement and hold the broken bones in place. These devices may help decrease pain and prevent more bone damage.
- Medicines may be used to prevent or treat pain.
- Surgery may be used to put your bones back into the correct position. Wires, pins, plates, or screws may be used to keep the broken pieces lined up correctly and hold them together.
What can I do to help my leg fracture heal?
- Rest your leg as directed and avoid activities that cause leg pain.
- Apply ice on your leg for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel before you apply it. Ice helps prevent tissue damage and decreases swelling and pain.
- Elevate your leg above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your leg on pillows or blankets to keep it elevated comfortably.

- Use crutches or a walker as directed. Crutches will help you walk and take some weight off your leg while it heals.
- Physical therapy may be recommended. A physical therapist teaches you exercises to help improve movement and strength, and to decrease pain.
Call your local emergency number (911 in the US) if:
- You suddenly feel lightheaded and short of breath.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
When should I seek immediate care?
- Your leg feels warm, tender, and painful. It may look swollen and red.
- The pain in your leg gets worse even after you rest and take medicine.
- Your cast gets wet or damaged.
- Your leg or toes are numb.
- Your leg becomes swollen, cold, or blue.
When should I call my doctor?
- You have a fever.
- Your cast or brace is too tight.
- You notice new blood stains or a bad smell coming from under the cast.
- You have new or worsening trouble moving your leg.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Leg Fracture
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
