Keratitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is keratitis?
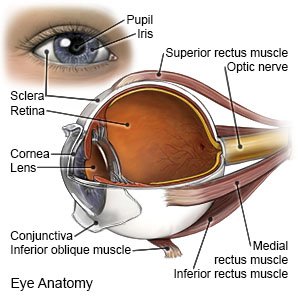
Keratitis is inflammation of the cornea. The cornea is the clear layer that covers the front of your eye. Keratitis may develop in one or both eyes.
 |
What causes keratitis?
- Trauma, such as a fingernail scratch or foreign body
- Exposure to sudden bright light, such as snow or water sports, or welding
- Wearing contact lenses for longer than recommended
- Bacteria, viruses, fungi, or parasites
- Inflammatory diseases, such as rheumatoid arthritis or granulomatosis with polyangiitis
What are the signs and symptoms of keratitis?
- Red eye
- Eye pain
- Feeling that something is in your eye
- Watery eye
- Blurred vision
- Sensitivity to light
- Swelling of the eyelid
How is keratitis diagnosed?
Your healthcare provider will ask about your symptoms and when they started. You may also need any of the following:
- An eye exam to check your vision, or to look for a foreign object or any tears in your cornea. Eye pressure may also be checked. Numbing medicine may be given.
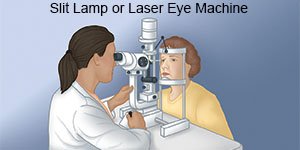
- A slit-lamp exam is a procedure used to check the inside of your eye. Your healthcare provider shines a bright light in your eye. You may need eyedrops to dilate your pupils.
How is keratitis treated?
- Medicines to decrease pain, inflammation, or prevent infection. These may be given as eye drops or pills.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I help manage or prevent keratitis?
- Do not wear contact lenses until your symptoms are gone. When you do wear contacts, use them correctly. Do not wear them for longer than your doctor says you should. Clean and store them properly.
- Wear safety equipment when you work, garden, or play sports. Do not rub your eyes while you work with wood or metal.
- Wash your hands often. Wash your hands several times each day. Wash after you use the bathroom, change a child's diaper, and before you prepare or eat food. Use soap and water every time. Rub your soapy hands together, lacing your fingers. Wash the front and back of your hands, and in between your fingers. Use the fingers of one hand to scrub under the fingernails of the other hand. Wash for at least 20 seconds. Rinse with warm, running water for several seconds. Then dry your hands with a clean towel or paper towel. Use hand sanitizer that contains alcohol if soap and water are not available. Do not touch your eyes, nose, or mouth without washing your hands first.

- Eye patches may be used over the eye for comfort. Patches are generally used for 24 hours.
When should I seek immediate care?
- You have severe eye pain.
- You have a sudden change in your vision.
- You suddenly lose your vision.
- Your symptoms do not go away within 48 hours.
When should I call my ophthalmologist?
- You have a fever.
- Your symptoms get worse, even after treatment.
- You have pus draining from your eye.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Keratitis
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
