Corneal Ulcer
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a corneal ulcer?
A corneal ulcer is an open sore on your cornea. The cornea is the smooth, clear outer layer of your eye. A corneal ulcer is caused by bacteria that get into your eye, such as through a scratch.
What increases my risk for a corneal ulcer?
- Dry eyes
- Eye injury from an accident, contact lenses, or a chemical splash
- Medical conditions, such as diabetes or rheumatoid arthritis
- Incorrect use of eye medicines
- Swollen eyelids
- Recent eye surgery
What are the signs and symptoms of a corneal ulcer?
The most common symptom is eye pain. You may also have the following:
- A feeling that you have something in your eye
- Round, white spots or gray haze on your eye
- Red, swollen, and watery eyes
- Red skin around your eye
- Blurred or decreased vision
- Sensitivity to bright light
How is a corneal ulcer diagnosed?
Your healthcare provider will examine your eye and ask about your symptoms. You may need any of the following:
- Slit-lamp test: A microscope is used to look into your eye and check for injury. Your healthcare provider may use dye to see your injury better.
- Contact lens culture: Your healthcare provider may take a sample of your contact lens to check for bacteria.
How is a corneal ulcer treated?
- NSAIDs: These medicines decrease swelling, pain, and fever. NSAIDs are available without a doctor's order. Ask your healthcare provider which medicine is right for you. Ask how much to take and when to take it. Take as directed. NSAIDs can cause stomach bleeding and kidney problems if not taken correctly.
- Antibiotic eye medicine: This is given to treat an infection caused by bacteria. It may be in eyedrops or an ointment.
- Cycloplegic eye medicine: This will dilate your pupil and relax your eye muscles, which will decrease your pain.
- Pain medicines: You may be given prescription medicine to take away or decrease pain. Do not wait until the pain is severe before you take your medicine.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What are the risks of a corneal ulcer?
Your condition may return or worsen after treatment. The bacteria may spread deeper into your eye and cause tissue damage or scarring. Without treatment, you could lose your vision.
How can I manage my symptoms?
- Apply a warm compress: Wet a washcloth with warm water and place it on your eye. This will help decrease swelling and pain. Use as often as directed.
- Clean around your eye: Gently remove any crusty buildup around your eye.
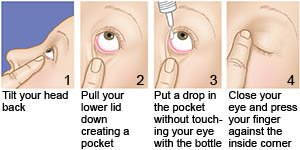
- Use eyedrops: This will keep your eyes moist and help decrease pain.
- Use safety equipment: Wear sunglasses or safety goggles to avoid another injury.
- Ask about your contacts: Do not wear contact lenses until your healthcare provider says it is okay. Always clean your contact lenses with proper contact cleaner.
When should I contact my healthcare provider?
- Your vision gets worse.
- Your symptoms do not improve with treatment.
- You have questions or concerns about your condition or care.
When should I seek immediate care or call 911?
- You have severe eye pain.
- You lose your vision.
- You think your corneal ulcer is getting bigger.
- You injure your eye again.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Corneal Ulcer
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
