Skin Grafting
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about skin grafting?
Skin grafting is surgery to cover and repair wounds with a skin graft. A skin graft is healthy skin taken from an area of your body called the donor site. The skin may be taken from an area near the injury to match the area where the graft will be placed. Grafts that are artificial or come from another person or animal may be used temporarily. These are used as covers when large areas of the skin are damaged. They are replaced with your own skin over time.
What are the types of skin grafts?
- Full-thickness grafts are used for deep wounds, so all the layers of skin are taken for the graft. This type of graft is used when it is important to match your skin color, such as on your face. It may also be used when tightening of the skin should be avoided, such as on the fingers. The graft will be trimmed to the correct size and shape to fit the wound.
- Split-thickness grafts are used for shallow, large surface area wounds. The top 2 layers of skin are taken for the graft. This type of graft is also used when more blood and fluid are expected to drain from the wound. The graft is applied as a sheet if the wound is on your face, neck, or hand. It is meshed (cut and stretched) if it is not large enough to cover the wound.
How do I prepare for skin grafting?
- Your surgeon will tell you how to prepare. He or she may tell you not to eat or drink anything after midnight on the day of surgery. Arrange to have someone drive you home after surgery.
- Tell your surgeon about all medicines you currently take. He or she will tell you if you need to stop any medicine for surgery, and when to stop. He or she will tell you which medicines to take or not take on the day of surgery.
- You may need to have blood tests, an ECG, x-ray, or other tests.
- Your surgeon may also need to prepare the wound and donor sites before the surgery. He or she may need to clean the wound site by removing dead tissue. He or she may ask you to keep the wound free from germs until your surgery.
- An anesthesiologist may talk to you before your surgery. You will be given anesthesia to control pain during surgery. Tell him or her if you or anyone in your family had a problem with anesthesia.
Related medications
During your surgery:
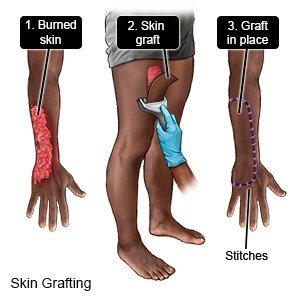
The pattern of the wound will be drawn over the skin of the donor site with a surgical marking pen. If the skin graft will come from your body, the graft will be taken from the donor site. After the graft is fitted and placed over the wound, stitches will be used to attach it in place. The donor site will also be closed with sutures or surgical staples. Bandages will be placed over the graft and donor sites.
 |
What should I expect after skin grafting?
- Medicines may be given to prevent or treat pain, severe itching, or an infection.
- Bandages will cover the surgery area to hold the graft in place. Do not remove the bandage yourself. Your healthcare provider will arrange for the bandage to be removed or changed after a few days. Keep the bandage clean and dry.
- You may need to avoid certain activities , such as exercise or lifting heavy objects. You may also need to avoid activities that can irritate your wounds. Your surgeon will tell you which activities to avoid or limit.
What are the risks of skin grafting?
- The grafted skin may die, and you may need another graft. The grafted skin may not look or feel the way you expected. The skin may contract (shrink) or change color. Scars may form on the graft and donor sites. You may bleed more than expected or get an infection. Bleeding or infection under the graft may slow or prevent wound healing. You could have trouble breathing or develop blood clots.
- You may have continued pain or swelling after surgery. Certain diseases or conditions may slow the healing process. Some examples are diabetes, blood vessel problems, and liver, kidney, lung, or heart conditions. Poor nutrition or a weak immune system may also cause problems with healing.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
