Endoscopic Biliary Stent Placement
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about an endoscopic biliary stent placement?
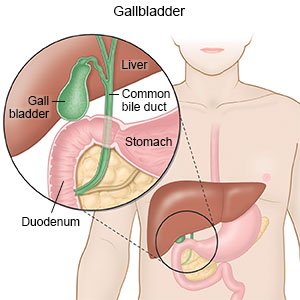
An endoscopic biliary stent placement is a procedure to open a blocked bile duct. Your bile duct carries bile from your gallbladder to your small intestine. Bile helps your body digest foods. A stent is a small tube made of plastic or metal. The stent helps widen your bile duct and keeps it open.
 |
How do I prepare for an endoscopic biliary stent placement?
- Your healthcare provider will talk to you about how to prepare for your procedure. He or she may tell you not to eat or drink anything after midnight on the day of your procedure. He or she will tell you what medicines to take or not take on the day of your procedure. You may need to stop taking blood thinners, aspirin, or NSAIDs several days before your procedure.
- You may be given an antibiotic to help prevent a bacterial infection. You will be given contrast liquid during your procedure. Tell your healthcare provider if you have ever had an allergic reaction to contrast liquid or antibiotics. Arrange for someone to drive you home and stay with you.
Related medications
What will happen during an endoscopic biliary stent placement?
- You will be given general anesthesia to keep you asleep and free from pain during surgery. Your healthcare provider will insert an endoscope through your mouth and into your stomach. An endoscope is a long tube with a camera and a light. The provider will move the endoscope until it reaches your small intestines. He or she will use the camera to find the opening to your bile duct.
- Your healthcare provider will inject contrast liquid into your bile duct. This will help your bile duct show up better in pictures. Your provider may use a balloon to widen your bile duct. He or she will insert 1 or more stents through the endoscope and into your bile duct. The provider will take more pictures to make sure the stent or stents are in the correct position.
What will happen after an endoscopic biliary stent placement?
Healthcare providers will monitor you until you are awake. You may need blood tests to check your liver function. You may have abdominal pain or feel bloated. You may also feel nauseous. These symptoms should go away in a few hours. You may be able to go home or you may need to spend a night in the hospital.
What are the risks of an endoscopic biliary stent placement?
You may bleed more than expected or get an infection. The endoscope or tools may damage your esophagus, stomach, intestines, or bile duct. The biliary stent may move out of place or block your bile duct. The procedure may not work and you may need to have another stent placed.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
