Congenital Heart Disease in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
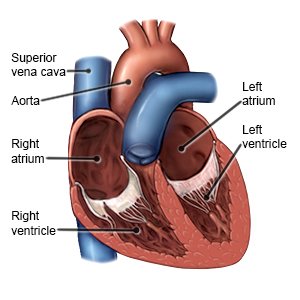
Congenital heart disease (CHD)
is a term used to describe defects in the structure of the heart. It may also be called congenital heart defect. Congenital means your child was born with the heart defect. The defect may affect the heart valves, walls, or blood vessels. Your child may have a hole in part of the heart or narrowing of arteries connected to the heart. Blood may not be able to flow to or flow through your child's heart correctly. The defect may be mild or severe. Your child will need life-long monitoring of CHD.
 |
Call your local emergency number (911 in the US) for any of the following:
- Your child has any of the following signs of a stroke:
- Numbness or drooping on one side of his or her face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
- Your child has a seizure.
- Your child faints or loses consciousness.
- Your child has sudden shortness of breath.
Call your child's doctor if:
- Your child has a fever.
- Your child has chills, a cough, or feels weak and achy.
- Your child is not gaining weight as he or she should, or has a sudden weight gain.
- Your child has new swelling in his or her ankles or legs.
- You have questions or concerns about your child's condition or care.
Signs and symptoms of CHD:
Your child may not have signs or symptoms for a few years. He or she may never have signs or symptoms. Your child may have any of the following:
- High blood pressure
- Trouble breathing, hyperventilation (breathing too quickly)
- Chest pain or sweating
- Blue skin or nails that becomes worse when your child cries
- Fussiness, trouble feeding, or a lack of appetite
- Slower growth, or being small and underweight
- Being out of breath, especially after moving quickly
- Fatigue or fainting
Treatment for CHD
may not be needed. The defect may need to be treated if it is severe or is a type that will not go away without treatment. Your child's age and overall health will also help healthcare providers decide if the defect should be treated. It may not cause health problems as your child gets older.
- Medicines may be used to help your child's heart beat more regularly. He or she may also need medicine to help get rid of extra fluid. He or she may urinate more while taking this medicine.
- A catheter procedure may be used to repair a defect. A catheter is a long, thin tube. Your child's healthcare provider will move the catheter through a vein or artery until it is near the defect. He or she may place a patch or plug on a hole in your child's heart. To widen a narrowed area, a small balloon device attached to the catheter may be inflated. This may also widen a narrowed valve in the heart.
- Surgery may be needed to repair the defect. Your child may need surgery to have a heart valve repaired or replaced. Surgery can also help repair problems from blood vessels that did not form correctly. A heart transplant may be needed if the defect is severe and other treatments do not work. Your child may need more surgery over time.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Manage your child's CHD:
- Do not smoke around your child. Nicotine and other chemicals in cigarettes and cigars can cause heart and lung damage. Your child's risk for health problems is increased if he or she breathes in secondhand smoke. Talk to your older child about not smoking. Ask your healthcare provider for information if you or your older child currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Ask about physical activity. Exercise is important for heart health. Your child's healthcare provider can tell you how much exercise your child needs each day and which exercises are best for him or her. Your child may not be able to do some physical activities or sports. The decision may depend on the type of defect your child has and if it was repaired. Your child's healthcare provider can give you written instructions for activities your child can do. You can give the instructions to your child's school officials.
- Give your child a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, lean meats and fish, and beans. Your child's healthcare provider or a dietitian can help you plan healthy meals and snacks for your child.

- Keep your child's teeth clean and healthy. Have your child get regular checkups at the dentist. Make sure your child brushes his or her teeth as directed. Cavities increase your child's risk for endocarditis (infection in the lining around his or her heart). Antibiotics may be needed before dental procedures. The antibiotic can help prevent an infection caused by bacteria.
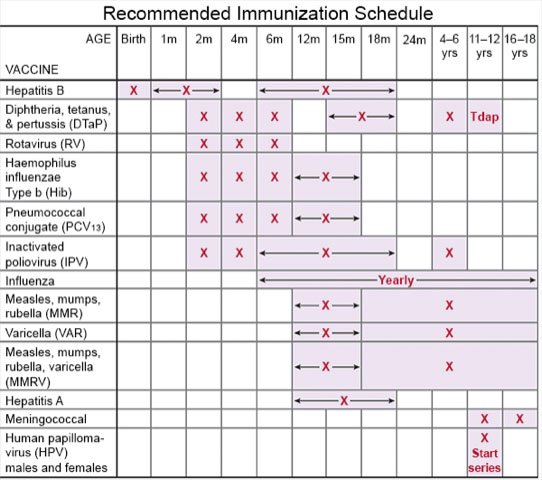
- Ask about vaccines your child needs. Vaccines can help protect your child from diseases that can be dangerous for a child who has CHD. Examples include the flu, measles, and COVID-19. Ask which vaccines your child needs and when he or she should get them.
Follow up with your child's doctor as directed:
Your child will need ongoing tests to monitor his or her heart function. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Congenital Heart Disease
- Atorvastatin (Lipitor): Top 12 Drug Facts You Need to Know
- Do blood pressure drugs interact with alcohol?
- Side Effects of Weight Loss Drugs
Treatment options
- Medications for Congenital Heart Disease
- Medications for Heart Disease
- Medications for Valvular Heart Disease
Care guides
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
