Chronic Abdominal Pain
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is chronic abdominal pain?
Chronic abdominal pain lasts longer than 3 months.
 |
What causes chronic abdominal pain?
The cause of your pain may not be found. The following are possible causes:
- Anxiety or stress
- Lactose intolerance or celiac disease
- Liver disease, cancer, or chronic pancreatitis
- Irritable bowel syndrome, ulcerative colitis, or Crohn disease
- An ulcer in your esophagus or stomach, or an infection
- A hernia or tissue growth that causes organs and tissues to stick together
What are the signs and symptoms of chronic abdominal pain?
Signs and symptoms may come and go. You may feel pain in all areas of your abdomen, or just in one place. You may not want to eat. You may not want to do your daily activities. You may also have any of the following:
- Cramping
- Acid reflux
- Bloating and gas
- Constipation or diarrhea
- Nausea and vomiting
How is the cause of chronic abdominal pain diagnosed?
Your healthcare provider will examine you. He or she may ask about your family history of abdominal pain. Tell your provider about your symptoms and the medicines you currently take. Tell him or her if anything makes your symptoms better or worse. Based on what your provider finds, and your symptoms, you may need any of the following:
- Blood tests may be done to check for inflammation or to get information about your overall health.
- A sample of your bowel movement may be tested to see if you are absorbing nutrients. The sample can also be tested for anything may be causing your pain.
- X-ray, ultrasound, CT, or MRI pictures may be used to check the organs inside your abdomen. You may be given contrast liquid to help the organs show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
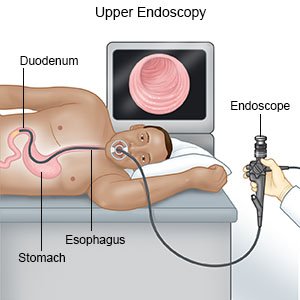
- An endoscopy is a test to look inside your esophagus, stomach, and small intestine. During an endoscopy, healthcare providers may find problems in your esophagus, stomach, or small intestine. Some problems may be fixed during the endoscopy. Samples may be taken from your esophagus, stomach, or small intestine, and sent to a lab for tests.
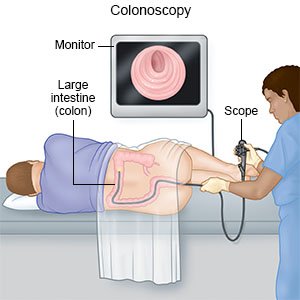
- A colonoscopy is a test used to look inside your colon for problems. Some problems may be fixed during the colonoscopy. Samples may be taken from your colon and sent to a lab for tests.
How is chronic abdominal pain treated?
Healthcare providers may not find a medical problem that is causing your pain. You may need any of the following if a cause is found:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Medicines may be given to manage symptoms such as vomiting or constipation. Medicines may also be used to help manage a cause of your pain, such as anxiety.
- Therapy can help you learn to cope with stress and anxiety. This may help decrease your abdominal pain.
- Surgery is rarely needed but may be done to treat a problem with an organ in your abdomen. Examples include an organ that is stuck to tissue or a hernia.
How can I manage chronic abdominal pain?
- Apply heat on your abdomen for 20 to 30 minutes every 2 hours for as many days as directed. Heat helps decrease pain and muscle spasms.
- Make changes to the foods you eat, if needed. Do not eat foods that cause abdominal pain or other symptoms. Eat small meals more often. The following changes may also help:
- Eat more high-fiber foods if you are constipated. High-fiber foods include fruits, vegetables, whole-grain foods, and legumes such as pinto beans.

- Do not eat foods that cause gas if you have bloating. Examples include broccoli, cabbage, beans, and carbonated drinks.
- Do not eat foods or drinks that contain sorbitol or fructose if you have diarrhea and bloating. Some examples are fruit juices, candy, jelly, and sugar-free gum.
- Do not eat high-fat foods. Examples include fried foods, cheeseburgers, hot dogs, and desserts.
- Eat more high-fiber foods if you are constipated. High-fiber foods include fruits, vegetables, whole-grain foods, and legumes such as pinto beans.
- Make changes to the liquids you drink, if needed. Do not drink liquids that cause pain or make it worse, such as orange juice. Drink liquids throughout the day to stay hydrated. The following changes may also help:
- Drink more liquids to prevent dehydration from diarrhea or vomiting. Ask your healthcare provider how much liquid to drink each day and which liquids are best for you.
- Limit or do not have caffeine. Caffeine may make symptoms such as heartburn or nausea worse.
- Limit or do not drink alcohol. Alcohol can make your abdominal pain worse. Ask your healthcare provider if it is okay for you to drink alcohol. Also ask how much is okay for you to drink. A drink of alcohol is 12 ounces of beer, 1½ ounce of liquor, or 5 ounces of wine.
- Keep track of your abdominal pain. This may help your healthcare provider learn what is causing your pain. Include when the pain happens, how long it lasts, and what the pain feels like. Include any other symptoms you have. Also track what you eat, and any symptoms you have after you eat.
- Manage stress. Stress may cause abdominal pain. Your healthcare provider may recommend relaxation techniques and deep breathing exercises to help decrease your stress. Your healthcare provider may recommend you talk to someone about your stress or anxiety, such as a counselor or a friend. Get plenty of sleep. Exercise regularly.

- Do not smoke. Nicotine and other chemicals in cigarettes can damage your esophagus and stomach. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
When should I seek immediate care?
- Your abdominal pain gets worse, and spreads to your back.
- You vomit blood or what looks like coffee grounds.
- You have blood or mucus in your bowel movement.
- You cannot stop vomiting.
- You have diarrhea for more than 1 week.
- You feel weak, dizzy, or faint.
- Your abdomen is larger than usual, more painful, and hard.
When should I call my doctor?
- You have a fever or chills.
- You have new or worsening symptoms.
- You lose weight without trying.
- Your pain prevents you from doing your daily activities.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Chronic Abdominal Pain
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
