Bronchiectasis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
Bronchiectasis is a condition that causes mucus to collect in your airway. Chronic respiratory infections or inflammation cause the bronchi to become thick. Bronchi are larger airways that help carry air in and out of your lungs. Your lungs make mucus to trap and remove germs and irritants that you breathe. Bronchiectasis prevents your lungs from clearing the mucus. This leads to more infections and inflammation, and scarring in your lungs.
 |
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that you may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done. Make sure all your questions are answered.
Medicines:
- Antibiotics help fight or prevent an infection caused by bacteria. Some antibiotics also help bring down swelling in your airway. You may get antibiotics as pills, through an IV, or breathed in through a nebulizer.
- Bronchodilators help open the air passages in your lungs.
- Mucolytics help thin the mucus from your lungs. Thin mucus may be easier to cough up.
- Steroids help decrease inflammation in your lungs and open your airway so you can breathe easier.
Tests:
- A sputum (mucus) sample is collected in a cup when you cough. The sample is sent to a lab to find out if you have an infection.
- X-ray or CT scan pictures are used to check your lungs and airway. You may be given contrast liquid to help these show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- Bronchoscopy is done to look inside your airway and lungs. Healthcare providers insert a bronchoscope (a tube with a light on the end) into your mouth and down into your lungs. Healthcare providers may also collect samples of sputum, fluid, or cells from your lungs for testing. This may help find the cause or see if you have an infection.
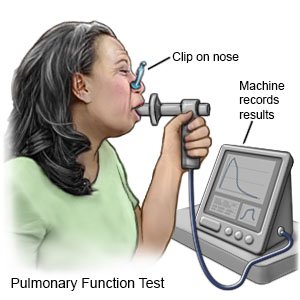
- Pulmonary function tests help healthcare providers learn how well your body uses oxygen. You breathe into a mouthpiece connected to a machine. The machine measures how much air you breathe in and out over a certain amount of time.
Treatment:
- Oxygen may be given through a mask or nasal cannula to help you breathe easier. Oxygen can also decrease the strain on your heart and can help prevent more breathing problems.
- Surgery may be used to remove a part of your lung causing your symptoms. You may also need a lung transplant if your symptoms become severe. Surgery may also be needed to stop heavy bleeding in your airway if you cough up a lot of blood.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
RISKS:
As more airway damage happens, you may develop lung conditions such as emphysema or respiratory failure. Pressure can grow in your pulmonary artery (blood vessel) and lead to heart failure. Respiratory or heart failure may be life-threatening.
CARE AGREEMENT:
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Bronchiectasis
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
