Anaphylaxis in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is anaphylaxis?
Anaphylaxis is a life-threatening allergic reaction that must be treated immediately. Your child's risk for anaphylaxis increases if he or she has asthma or allergies. Medical conditions such as heart disease can also increase your child's risk. It is important to be prepared if your child is at risk for anaphylaxis. Symptoms can be worse each time he or she is exposed to a trigger.
What may trigger anaphylaxis?
The following are some of the most common triggers for children:
- Milk, peanuts, tree nuts, eggs, shellfish and certain other types of fish, wheat, and soy
- Stings from bees, wasps, or fire ants
- Antibiotics, NSAIDs, or aspirin
- Latex
- Exercise following exposure to another trigger, such as after your child eats a trigger food
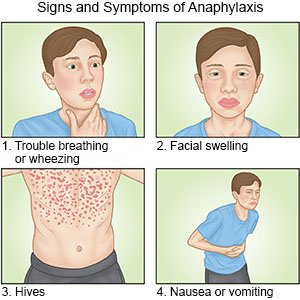
What are the signs and symptoms of anaphylaxis?
Your child may have any of the following within seconds to hours after exposure to a trigger:
- Trouble breathing, shortness of breath, wheezing, or coughing
- Throat tightening, swelling of the lips or tongue, or trouble swallowing
- Rash, hives, swelling, or itching
- Nausea, vomiting, diarrhea, or abdominal cramps
- Dizziness, lightheadedness, fainting, or confusion
- Sudden behavior changes or irritability
-
How is anaphylaxis diagnosed?
Your child's healthcare provider will examine your child for signs of anaphylaxis. The provider will ask if your child has a history of allergies. The provider will also ask about exposure to possible triggers and when they occurred. Tell the provider if your child takes medicines or has any health conditions. Your child may need more testing if he or she developed anaphylaxis after being exposed to a trigger and then exercising. This is called exercise-induced anaphylaxis.
How is anaphylaxis treated?
Your child's healthcare provider will remove the allergen from your child, if possible. Your child may also need any of the following:
- Epinephrine is medicine used to treat severe allergic reactions such as anaphylaxis. It is given as a shot into the outer thigh muscle.
- Medicines such as antihistamines, steroids, and bronchodilators decrease inflammation, open airways, and make breathing easier.
- Intravenous (IV) fluids may be given to treat low blood pressure caused by anaphylaxis or epinephrine.
- Oxygen may be needed if your child's blood oxygen level is lower than it should be. Your child may get oxygen through a mask placed over his or her nose and mouth or through small tubes placed in the nostrils.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What steps do I and my child need to take for signs or symptoms of anaphylaxis?
- Immediately give 1 shot of epinephrine only into the outer thigh muscle. Even if your child's allergic reaction seems mild, it can quickly become anaphylaxis. This may happen even if your child had a mild reaction to the allergen in the past. Each exposure can cause a different reaction. Watch for signs and symptoms of anaphylaxis every time your child is exposed to a trigger. Be ready to give a shot of epinephrine. It is okay to inject epinephrine through clothing. Just be careful to avoid seams, zippers, or other parts that can prevent the needle from entering the skin.
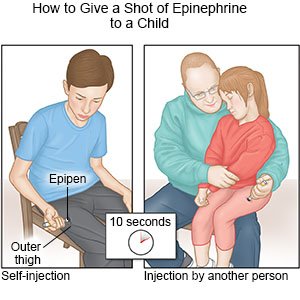
- Leave the shot in place as directed. Your child's healthcare provider may recommend you leave it in place for up to 10 seconds before you remove it. This helps make sure all of the epinephrine is delivered.
- Call your local emergency number and go to the emergency department, even if the shot improved your child's symptoms. Tell your adolescent never to drive himself or herself. Bring the used epinephrine shot to the emergency department.
What safety precautions do I and my child need to take?
- Keep 2 shots of epinephrine with your child at all times. Your child may need a second shot, because epinephrine only works for about 20 minutes and symptoms may return. Your child's healthcare provider can show you, your child, and other family members how to give the shot. Check the expiration date every month and replace it before it expires.
- Create an action plan. Your child's provider can help you create a written plan that explains the allergy and an emergency plan to treat a reaction. The plan explains when to give a second epinephrine shot if symptoms return or do not improve after the first. Give copies of the action plan and emergency instructions to family members, work and school staff, and daycare providers. Show them how to give a shot of epinephrine.
- Help your child be careful when he or she exercises. If your child has had exercise-induced anaphylaxis, do not let him or her exercise right after he or she eats. Tell your child to stop exercising right away if he or she starts to develop any signs or symptoms of anaphylaxis. Your child may first feel tired, warm, or have itchy skin. Hives, swelling, and severe breathing problems may develop if he or she continues to exercise.
- Have your child carry medical alert identification. Have your child wear medical alert jewelry or carry a card that explains the allergy. Ask your child's provider where to get these items.
- Identify and avoid known triggers. Read food labels for ingredients. Look for triggers in your child's environment.
- Ask about treatments to prevent anaphylaxis. Your child may need allergy shots or other medicines to treat allergies.
Call your local emergency number (911 in the US) if:
- Your child has a skin rash, hives, swelling, or itching.
- Your child has trouble breathing, shortness of breath, wheezing, or coughing.
- Your child's throat tightens or his or her lips or tongue swell.
- Your child has trouble swallowing or speaking.
- Your child is dizzy, lightheaded, confused, or feels like he or she is going to faint.
- Your child has nausea, diarrhea, or abdominal cramps, or he or she is vomiting.
When should I seek immediate care?
- Signs or symptoms of anaphylaxis return.
When should I call my child's doctor?
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Anaphylaxis
Treatment options
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
