Abdominal Pain in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What do I need to know about abdominal pain in children?
Abdominal pain may be felt anywhere between the bottom of your child's rib cage and his or her groin. Acute pain usually lasts less than 3 months. Chronic pain lasts longer than 3 months. Your child's pain may be sharp or dull. The pain may stay in the same place or move around. Your child may have the pain all the time, or it may come and go. Depending on the cause, he or she may also have nausea, vomiting, fever, or diarrhea.
 |
What causes abdominal pain in children?
The cause may not be found. The following are common causes of abdominal pain in children:
- Overeating, gas pains, or food poisoning
- Constipation or diarrhea
- An injury
- A serious health problem, such as appendicitis
How will I know if my baby has abdominal pain?
Your baby may do any of the following when he or she has pain:
- Bite or squeeze his or her lips tightly
- Cry with a higher pitch, whimper, or groan
- Move around a lot to lie in a way that will not hurt, or move his or her arms around
- Frown or squeeze his or her eyes shut tightly
- Pull his or her knees up to his or her chest
- Get upset when touched
- Shudder (mild shake)
- Sleep more or less than usual
- Touch, rub, or massage his or her abdomen
How will I know if my young child has abdominal pain?
Your toddler, preschooler, or young child may do any of the following when he or she has pain:
- Hold his or her arms, legs, or body stiffly
- Cry, whimper, or groan
- Act restless
- Guard or protect the painful area from touching anything
- Kick when someone comes near
- Lose control of bowel and bladder after he or she has been potty-trained
- Seem withdrawn and not do normal activities, such as play
- Touch, tug, rub, or massage his or her abdomen
How is the cause of abdominal pain in children diagnosed?
Your child's healthcare provider will ask about your child and check his or her abdomen. He or she will want you or your child to describe where the pain is and when it started. The provider may ask if the pain wakes your child or stops him or her from doing daily activities. Describe anything that seems to make the pain better or worse. Your child may need any of the following:
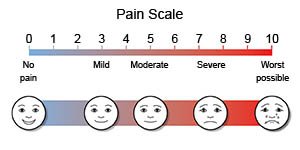
- A smiley face scale may be shown to your child. A smiling face is no pain, and a sad face with tears is very bad pain. Your child will be asked to point to the face that matches what he or she feels.
- Blood, urine, or bowel movement samples may be tested for signs of an infection, disease, or injury.
- X-ray pictures of your child's abdomen may show an injury or other cause of the pain.
How is abdominal pain in children treated?
- Medicines may be given to calm your child's stomach or prevent vomiting.
- Prescription pain medicine may be needed. Ask your child's healthcare provider how to give this medicine safely. Some prescription pain medicines contain acetaminophen. Do not give your child other medicines that contain acetaminophen without talking to a healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your child's provider how to prevent or treat constipation.
- Do not give aspirin to children younger than 18 years. Your child could develop Reye syndrome if he or she has the flu or a fever and takes aspirin. Reye syndrome can cause life-threatening brain and liver damage. Check your child's medicine labels for aspirin or salicylates.
- Relaxation therapy may be used along with pain medicine.
- Surgery may be needed, depending on the cause.
What can I do to help manage my child's abdominal pain?
- Take your child's temperature every 4 hours, or as directed. A fever may be a sign of a condition that needs to be treated.
- Have your child rest until he or she feels better. He or she may need to take more naps than usual during the day. Do not let your child play with other children if he or she has a contagious illness, such as the flu.
- Ask when your older child can eat solid foods. You may be told not to feed your child solid foods for 24 hours.
- Give your child an oral rehydration solution (ORS), as directed. ORS is liquid that contains water, salts, and sugar to help prevent dehydration. Ask what kind of ORS to use and how much to give your child.
- Apply heat on your child's abdomen to help with pain or muscle spasms. You can apply heat with an electric heating pad set on low, a hot water bottle, or a warm compress. Heat should be applied for about 20 to 30 minutes or as long and as often as directed. Always put a cloth between your child's skin and the heat pack to prevent burns.
- Keep track of your child's abdominal pain. This may help your child's healthcare provider learn what is causing the pain. Track when the pain happens, how long it lasts, and how your child describes the pain. Include any other symptoms he or she has with abdominal pain. Also include what your child eats and drinks, and any symptoms that develop after he or she eats.
How can I help my child prevent abdominal pain?
Your child's healthcare provider may give you specific instructions based on your child's age. The following are general guidelines:
- Make changes to the foods you give your child, if needed. Do not give your child foods that cause abdominal pain or other symptoms. Have him or her eat small meals more often. The following changes may also help:
- Give more high-fiber foods if your child is constipated. High-fiber foods include fruits, vegetables, whole-grain foods, and legumes such as pinto beans.

- Do not give foods that cause gas if your child has bloating. Examples include broccoli, cabbage, beans, and carbonated drinks.
- Do not give foods or drinks that contain sorbitol or fructose if your child has diarrhea. Some examples are fruit juices, candy, jelly, and sugar-free gum.
- Do not give high-fat foods. Examples include fried foods, cheeseburgers, hot dogs, and desserts.
- Give more high-fiber foods if your child is constipated. High-fiber foods include fruits, vegetables, whole-grain foods, and legumes such as pinto beans.
- Make changes to the liquids your child drinks, if needed. Do not give liquids that cause pain or make it worse, such as orange juice. The following changes may also help:
- Give your child more liquid, as directed. Give your child liquids throughout the day to help him or her stay hydrated. Ask how much liquid your child should drink each day and which liquids are best for him or her. Give your baby extra breast milk or formula to prevent dehydration. If you feed your baby formula, give him or her lactose-free formula.
- Do not give your child liquid that contains caffeine. Caffeine may make symptoms such as heartburn or nausea worse.
- Help your child manage stress. Stress may cause abdominal pain. Your child's healthcare provider may recommend relaxation techniques and deep breathing exercises to help decrease stress. The provider may recommend your child talk to someone about stress or anxiety, such as a counselor or a trusted friend. Help your child get plenty of sleep and physical activity.

When should I seek immediate care?
- Your child's abdominal pain gets worse.
- Your child vomits blood, or you see blood in his or her bowel movement.
- Your child's pain gets worse when he or she moves or walks.
- Your child has vomiting that does not stop.
- Your male child's pain moves into his genital area.
- Your child's abdomen becomes swollen or tender to the touch.
- Your child has trouble urinating.
When should I call my child's doctor?
- Your child's abdominal pain does not get better after a few hours.
- Your child has a fever.
- You have questions or concerns about your child's condition or care.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Abdominal Pain
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
