Cluster Headache
Medically reviewed by Drugs.com. Last updated on Jun 30, 2025.
What is a cluster headache?
A cluster headache is a very painful headache that starts quickly, peaks within 15 minutes, and stops suddenly. The headache usually lasts 30 to 60 minutes but can last up to 3 hours. Cluster headaches follow patterns and often occur at the same time of the day or year. You may have cluster headaches once every other day, or up to 8 each day. A cluster period usually lasts for 2 to 12 weeks but can last longer than a year. Weeks or months may pass before a new cluster period begins. A cluster headache can be triggered by alcohol, medicine, stress, bright light, or heat.
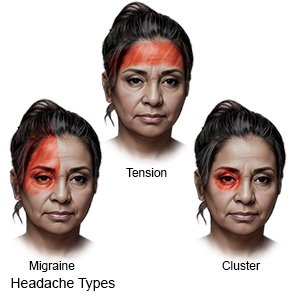 |
What increases my risk for a cluster headache?
The cause is not known. You are more likely to have cluster headaches if you are male. They often begin between the ages of 20 and 40 years. Your risk is also higher if you smoke or have a family history of cluster headaches.
What are the signs and symptoms of a cluster headache?
- Severe pain on one side of your head that stabs or burns
- Swollen or watery eye, or droopy eyelid
- A runny or stuffy nose
- Red or sweaty face
- Restlessness
- Sensitive to noise or light
- Exhaustion after the headache stops
How is a cluster headache diagnosed?
Your healthcare provider will ask you to describe your symptoms. Tell the provider how often your headaches occur and how long they last. The provider will ask about your medical history and medicines. Tell your provider if you smoke cigarettes or drink alcohol. You may also need any of the following tests:
- A neurological exam is a series of tests to check for problems with your brain and nervous system. Your healthcare provider will shine a light in your eyes to find out how they react to light. The provider may ask questions to check your memory, hand grasp, and balance.
- CT scan or MRI pictures may be taken of your brain and the blood vessels and structures in your head. You may be given contrast liquid to help images show up better on the monitor. Tell healthcare providers if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with any metal. The MRI uses a powerful magnet. Metal can cause serious injury from the magnet. Tell the healthcare provider if you have any metal in or on your body.
How is a cluster headache treated?
Cluster headaches cannot be cured, but treatment may help your symptoms. Your healthcare provider may have you try several medicines to find out what works best for you. You may need medicines for pain and for prevention. The following may be used to treat pain during a cluster headache:
- Extra oxygen may give you pain relief during a cluster headache. You will breathe through a plastic mask that is attached to an oxygen tank for about 15 minutes.
- Migraine medicine may be given to relieve your pain quickly.
- Steroids may help reduce pain and swelling. Steroids may also be used to prevent cluster headaches.
- Numbing medicine may be given to numb your pain if other treatments do not work.
- Surgery may be used if other treatments do not work. Surgery may be used to remove certain nerves that can lead to cluster headache pain. You may also need surgery to lower pain and inflammation in the nerves around your eye.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
What can I do to prevent a cluster headache?
One goal is to prevent headaches before they happen. Another goal is to shorten a cluster period. Headaches may happen less often and be less severe with certain medicines. Seizure medicine or mood stabilizers may be given to prevent cluster headaches. You may need to take one medicine at the start of a cluster period. You may take a different medicine for as long as your cluster period lasts or is expected to last.
Related medications
Fioricet
Fioricet (acetaminophen, butalbital, and caffeine) is used to treat tension headaches that are ...
Ubrelvy
Ubrelvy (ubrogepant) tablets are used for the acute treatment of migraine. Includes Ubrelvy side ...
Botox
Botox is used cosmetically to reduce facial lines and wrinkles and for medical purposes for ...
Nurtec ODT
Nurtec ODT (rimegepant) is used to treat acute migraines and prevent episodic migraines, by ...
Imitrex
Imitrex (sumatriptan) is used to treat migraine headaches, with or without aura, in adults ...
Maxalt
Maxalt (rizatriptan) is used to treat migraine headaches in adults, with or without aura. Includes ...
Advil
Advil (ibuprofen) reduces fever, pain and inflammation caused by headaches, toothaches, arthritis ...
Memantine
Memantine is used to treat moderate to severe dementia in people with Alzheimer’s disease. It is an ...
Acetaminophen/butalbital/caffeine
Acetaminophen/butalbital/caffeine is used for headache
Topiramate
Learn about topiramate, an anticonvulsant used for seizures, migraine prevention, and weight loss ...
What can I do to manage cluster headaches?
- Do not smoke. Cluster headaches are more common among smokers. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Do not drink alcohol during a cluster period. Alcohol triggers more headaches during cluster periods.
- Do not travel between altitudes. Altitude changes can trigger headaches. Do not fly on an airplane or travel between places with high and low altitudes.
- Set a regular sleep schedule. Go to sleep and wake up at the same times each day. Changes in sleep patterns may trigger cluster headaches.
- Manage stress. Stress, long hours at work, and emotional challenges can trigger cluster headaches. Find out what works for you to lower stress.
- Keep a headache record. Write down when your headaches start and stop, and exactly what you were doing when they began. Record what you ate or drank and how much you slept in the 24 hours before the headache. Keep track of the things you did to treat your symptoms. Write down if they did or did not help. Do this to learn what triggers your headaches and how to make them go away.
- Work with your healthcare provider to manage your pain. Both pain relievers and medicines used to treat other health conditions can trigger cluster headaches. Go over all your medicines with your healthcare provider. Work with your provider to manage your headache pain and other conditions.
You or someone close to you should call your local emergency number (911 in the US) if:
- Your pain is so bad you think about attempting suicide.
When should I seek immediate care?
- You feel more tired or sleepy than usual.
- You notice changes in your vision.
- Your stomach is upset or you are vomiting.
- You have a seizure.
When should I call my doctor or neurologist?
- You cannot get enough sleep because of your headaches.
- Your headaches happen each time you are active.
- Treatment does not help your symptoms.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Cluster Headache
- Advil Dosage Charts for Infants and Children
- Dosage Charts for Infants and Children
- Motrin Dosage Charts for Infants and Children
- Top 9 Things You Must Know About Naproxen
- Tylenol Dosage Charts for Infants and Children
- What are the risks of mixing pain medications and alcohol?
Treatment options
Care guides
Symptoms and treatments
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
