Hespan: Package Insert / Prescribing Info
Package insert / product label
Generic name: hetastarch in sodium chloride
Dosage form: injection, solution
Drug class: Plasma expanders
Medically reviewed by Drugs.com. Last updated on Oct 10, 2024.
On This Page
- Indications and Usage
- Dosage and Administration
- Dosage Forms and Strengths
- Contraindications
- Warnings and Precautions
- Adverse Reactions/Side Effects
- Drug Interactions
- Use In Specific Populations
- Description
- Clinical Pharmacology
- Nonclinical Toxicology
- Clinical Studies
- References
- How Supplied/Storage and Handling
Highlights of Prescribing Information
HESPAN® (6% HETASTARCH IN 0.9% SODIUM CHLORIDE INJECTION) IN EXCEL® CONTAINER, for intravenous use
Initial U.S. Approval: 1991
WARNING: MORTALITY; KIDNEY INJURY; COAGULOPATHY
See full prescribing information for complete boxed warning.
-
Use of hydroxyethyl starch (HES) products, including HESPAN®, increases risk of
- Mortality
- Kidney injury
- Coagulopathy
- DO NOT use HES products, including HESPAN®, unless adequate alternative treatment is unavailable.
Indications and Usage for Hespan
-
HESPAN® is a hetastarch indicated for treatment of hypovolemia when plasma volume expansion is desired in settings where adequate alternative treatment is unavailable. (1)
-
HESPAN® in leukapheresis has shown to be safe and efficacious in improving the harvesting and increasing the yield of granulocytes by centrifugal means. (1)
Hespan Dosage and Administration
For intravenous use only.
Dosage Forms and Strengths
- 30 g hetastarch in 500 mL 0.9% sodium chloride injection. (3)
Contraindications
- Do not use HES products, including HESPAN®, unless adequate alternative treatment is unavailable.
Warnings and Precautions
- Avoid use in patients with pre-existing renal dysfunction (5.1)
- Increased risk of mortality and acute kidney injury (AKI) in critically ill patients, including patients with sepsis; surgical patients; and blunt trauma patients (5.1)
- Discontinue use of HESPAN® at the first sign of renal injury (5.1)
- Continue to monitor renal function for at least 90 days as use of RRT has been reported up to 90 days after administration of HES products, including HESPAN® (5.1)
- HESPAN® is not recommended for use as a cardiac bypass pump prime, while the patient is on cardiopulmonary bypass, or in the immediate period after the pump has been discontinued because of the risk of increasing coagulation abnormalities and bleeding in patients whose coagulation status is already impaired. Discontinue use of HESPAN® at first sign of coagulopathy (5.2)
-
Monitor liver function in patients receiving HES products, including HESPAN® (5.2)
Adverse Reactions/Side Effects
- Most common adverse reactions are hypersensitivity, coagulopathy, hemodilution, circulatory overload and metabolic acidosis. (6.2)
To report SUSPECTED ADVERSE REACTIONS, contact B. Braun Medical Inc. at 1-800-854-6851 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Revised: 8/2021
Full Prescribing Information
WARNING: MORTALITY; KIDNEY INJURY; COAGULOPATHY
-
Use of hydroxyethyl starch (HES) products, including HESPAN®, increases risk of
- Mortality
- Kidney injury (5.1)
- Coagulopathy (5.2)
- DO NOT use HES products, including HESPAN®, unless adequate alternative treatment is unavailable. (1)
1. Indications and Usage for Hespan
HESPAN® is indicated in the treatment of hypovolemia when plasma volume expansion is desired in settings where adequate alternative treatment is unavailable. It is not a substitute for blood or plasma.
The adjunctive use of HESPAN® in leukapheresis has also been shown to be safe and efficacious in improving the harvesting and increasing the yield of granulocytes by centrifugal means.
2. Hespan Dosage and Administration
Dosage for Acute Use in Plasma Volume Expansion
HESPAN® is administered by intravenous infusion only. Total dosage and rate of infusion depend upon the amount of blood or plasma lost and the resultant hemoconcentration.
2.1 Adults
The amount usually administered is 500 to 1000 mL. Doses of more than 1500 mL per day for the typical 70 kg patient (approximately 20 mL per kg of body weight) are usually not required. Higher doses have been reported in postoperative and trauma patients where severe blood loss has occurred [see Warnings and Precautions (5)].
2.2 Leukapheresis
250 to 700 mL of HESPAN® (6% hetastarch in 0.9% sodium chloride injection) with citrate anticoagulant is administered by aseptic addition to the input line of the centrifugation apparatus at a ratio of 1:8 to 1:13 to venous whole blood. The HESPAN® and citrate should be thoroughly mixed to assure effective anticoagulation of blood as it flows through the leukapheresis machine.
2.3 Direction for use for HESPAN®
- Do not use plastic container in series connection. If administration is controlled by a pumping device, care must be taken to discontinue pumping action before the container runs dry or air embolism may result. If administration is not controlled by a pumping device, refrain from applying excessive pressure (>300mmHg) causing distortion to the container such as wringing or twisting. Such handling could result in breakage of the container.
- Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration whenever solution and container permit. Use only if solution is clear and container and seals are intact.
- Intended for intravenous administration using sterile equipment. It is recommended that intravenous administration apparatus be replaced at least once every 24 hours.
- Withdraw or expel all air from the bag through the medication port prior to infusion if administration is by pressure infusion.
-
For single use only. Discard unused portion.
CAUTION: Before administering to the patient, review these directions:
Visual Inspection
- Do not remove the plastic infusion container from its overwrap until immediately before use.
- Inspect each container. Read the label. Ensure solution is the one ordered and is within the expiration date.
- Invert container and carefully inspect the solution in good light for cloudiness, haze, or particulate matter.
- Any container which is suspect should not be used.
To Open
- Tear overwrap down at notch and remove solution container.
- Check for minute leaks by squeezing solution container firmly.
- If any leaks are found, discard solution as sterility may be impaired.
Preparation for Administration
- Remove plastic protector from sterile set port at bottom of container.
- Attach administration set. Refer to complete directions accompanying set.
When stored at room temperature, HESPAN® admixtures of 500-560 mL with citrate concentrations up to 2.5% were compatible for 24 hours. The safety and compatibility of additives other than citrate have not been established.
3. Dosage Forms and Strengths
Single-use container:
- 30 g hetastarch in 500 mL of 0.9% sodium chloride injection.
4. Contraindications
- Do not use HES products, including HESPAN®, unless adequate alternative treatment is unavailable.
5. Warnings and Precautions
5.1 Mortality and Renal Dysfunction
- Critically ill patients, including patients with sepsis, are at increased risk of mortality and acute kidney injury (AKI), including need for renal replacement therapy (RRT).
- Surgery patients are at increased risk of mortality and AKI
- Blunt trauma patients are at increased risk of mortality and AKI.
- Avoid use in patients with pre-existing renal dysfunction
- Discontinue use of HESPAN® at the first sign of renal injury
- Continue to monitor renal function for at least 90 days as use of RRT has been reported up to 90 days after administration of HES products, including HESPAN®
5.2 Coagulopathy
- HESPAN® is not recommended for use as a cardiac bypass pump prime, while the patient is on cardiopulmonary bypass, or in the immediate period after the pump has been discontinued because of the risk of increasing coagulation abnormalities and bleeding in patients whose coagulation status is already impaired. Monitor the coagulation status of surgery patients, as excess bleeding has been reported with HES solutions in this population. Discontinue use of HESPAN® at first sign of coagulopathy1-2
HESPAN® has not been adequately evaluated to establish its safety in uses over extended periods other than leukapheresis. HESPAN® has been associated with coagulation abnormalities in conjunction with an acquired, reversible von Willebrand’s-like syndrome and/or Factor Vlll deficiency when used over a period of days. Replacement therapy should be considered if a severe Factor Vlll deficiency is identified. If a coagulopathy develops, it may take several days to resolve. Certain conditions may affect the safe use of HESPAN® on a chronic basis. For example, in patients with subarachnoid hemorrhage where HESPAN® is used repeatedly over a period of days for the prevention of cerebral vasospasm, significant clinical bleeding may occur. Intracranial bleeding resulting in death has been reported.3
Slight declines in platelet counts and hemoglobin levels have been observed in donors undergoing repeated leukapheresis procedures using HESPAN® due to the volume expanding effects of hetastarch and to the collection of platelets and erythrocytes. Hemoglobin levels usually return to normal within 24 hours. Hemodilution by HESPAN® may also result in 24 hour declines of total protein, albumin, calcium, and fibrinogen levels. Regular and frequent clinical evaluation and complete blood counts (CBC) are necessary for proper monitoring of HESPAN® use during leukapheresis. If the frequency of leukapheresis is to exceed the guidelines for whole blood donation, you may wish to consider the following additional tests: total leukocyte and platelet counts, leukocyte differential count, hemoglobin and hematocrit, prothrombin time (PT), and partial thromboplastin time (PTT).
5.3 Hypersensitivity Reactions
Life threatening anaphylactic/anaphylactoid reactions including death have been rarely reported with HESPAN®. Patients may develop hypersensitivity reaction to corn starch from which this product is made. If a hypersensitivity reaction occurs, administration of the drug should be discontinued immediately and the appropriate treatment and supportive measures should be undertaken until symptoms have resolved.
5.4 Circulatory Overload
HESPAN® has not been adequately evaluated to establish its safety in situations other than treatment of hypovolemia in elective surgery.
Large volumes of HESPAN® may transiently alter the coagulation mechanism due to hemodilution and a direct inhibitory action on Factor Vlll. Administration of volumes of HESPAN® that are greater than 25% of the blood volume in less than 24 hours may cause significant hemodilution reflected by lower hematocrit and plasma protein values. Administration of packed red cells, platelets, or fresh frozen plasma should be considered if clinically indicated.
When using HESPAN® for plasma volume expansion, caution should be taken to avoid excessive hemodilution and circulatory overload especially in those patients at risk for developing congestive heart failure and pulmonary edema. HESPAN® is primarily excreted via the kidneys so caution should be exercised in patients who have impaired renal function. Although the risk of circulatory overload is largely dependent on the clinical circumstances, use of doses higher than 20 mL/kg/24h will increase the risk significantly. Increased risk of coagulation abnormalities and bleeding is also associated with higher doses. Monitor patients' vital signs and hemoglobin, hematocrit, platelet count, prothrombin time and partial thromboplastin time.
5.5 Liver Function Test
- Monitor liver function in patients receiving HES products, including HESPAN®
5.6 Drug/Laboratory Test Interactions
Bilirubin Levels
Indirect bilirubin levels of 8.3 mg/L (normal 0.0-7.0 mg/L) have been reported in 2 out of 20 normal subjects who received multiple infusions of HESPAN® (6% hetastarch in 0.9% sodium chloride injection). Total bilirubin was within normal limits at all times; indirect bilirubin returned to normal by 96 hours following the final infusion. The significance, if any, of these elevations is not known; however, caution should be observed before administering HESPAN® to patients with a history of liver disease.
Serum Amylase Levels
Elevated serum amylase levels may be observed temporarily following administration of HESPAN® although no association with pancreatitis has been demonstrated. Serum amylase levels cannot be used to assess or to evaluate for pancreatitis for 3-5 days after administration of HESPAN®. Elevated serum amylase levels persist for longer periods of time in patients with renal impairment. Hetastarch has not been shown to increase serum lipase.
6. Adverse Reactions/Side Effects
Serious adverse reactions reported in postmarket clinical trials include increased mortality and AKI (including need for RRT) in critically ill subjects, including subjects with sepsis, and surgical subjects. Clinical trials have also shown increased mortality and AKI in blunt trauma subjects. Increased coagulopathy was reported in surgical subjects.
Most common adverse reactions are hypersensitivity, coagulopathy, hemodilution, circulatory overload and metabolic acidosis.
6.1 Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
(Note: All of the studies listed below used licensed HES products except for reference 4.)
A randomized controlled trial (N=804) in severe sepsis patients using HES product (not approved in the U.S.) reported increased mortality (relative risk, 1.17; 95% CI, 1.01 to 1.36; p=0.03) and RRT (relative risk, 1.35; 95% CI, 1.01 to 1.80; p=0.04) in the HES treatment arm.4
Another randomized controlled trial (N=196) using different HES in severe sepsis patients reported no difference in mortality (relative risk,1.20; 95% CI, 0.83 to 1.74; p=0.33) and a trend for RRT (relative risk, 1.83; 95% CI, 0.93 to 3.59; p=0.06) in HES patients.5
A randomized controlled trial (N=7000) using different HES in a heterogeneous patient population consisting of critically ill adult patients admitted to the ICU reported no difference in mortality (relative risk, 1.06; 95% CI, 0.96 to 1.18; p=0.26) but increased use of RRT (relative risk, 1.21; 95% CI, 1.00 to 1.45; p=0.04) in HES patients.6
In a retrospective study of adult patients (N=1442) undergoing pulmonary or esophageal surgery who were prophylactically fluid restricted during the procedure, 74 developed AKI (5.1%) within the first 72 hours postoperatively. Fluid restriction neither increased nor was a risk factor for AKI. AKI occurred more often when HES products were administered to patients with decreased renal function or having >2 risk factors with normal renal function, whereas restriction of crystalloid was unrelated to AKI, regardless of preoperative renal function.12
In a retrospective case series of high-risk adult vascular surgery patients (N=796) receiving fluid therapy during a vascular surgery procedure, logistic regression analysis using prespecified confounding variables or suspected risk factors for AKI showed that intraoperative administration of an HES product was associated with increased likelihood of 30-day mortality and need for RRT, compared with use of crystalloids alone.13
In a retrospective study of adult subjects undergoing elective noncardiac surgery, patients (N=14,680) receiving an HES product and crystalloid were propensity-matched with patients (N=14,680) receiving only crystalloid. After controlling for potential confounding variables, odds of experiencing AKI of severe intensity with HES was 21% greater than with crystalloid alone. In addition, AKI risk increased as a function of HES volume.14
In a prospective observational study assessing the impact of HES products on recipient renal graft outcomes in brain-dead organ donors, data were obtained on 986 kidneys transplanted from 529 donors. Kidneys from donors who received HES had a higher rate of delayed graft function in recipient subjects (41% versus 31%). After accounting for the propensity of donors to receive HES products, HES product administration was independently associated with an increased risk of delayed graft function in recipients.A dose response relationship also was evident.15
In a randomized, controlled trial of adult subjects (N=33) undergoing elective cystectomy comparing an HES product versus lactated Ringer’s, administration of HES reduced clot strength (Maximum Amplitude; p<0.001) and increased blinded evaluation of perioperative blood loss by more than 50% (2181 mL versus 1370 mL, respectively; p=0.04). There was no significant between-group difference with respect to frequency of reoperation or length of hospital stay.16
In a prospective, sequential, observational study in adult subjects undergoing open heart surgery in association with cardiopulmonary bypass, fluid therapy using only an HES product (2004-2006, N=2137), 4% gelatin (2006-2008, N=2324) and crystalloids (N=2017, 2008-2010) led to increased need for renal replacement therapy after HES and gelatin, compared with crystalloid. Propensity score stratification confirmed greater use of RRT in the HES and gelatin periods compared to the crystalloid period. Fluid intake was higher in the crystalloid group only during the first 20 hours.17
In a retrospective observational study, 606 adult patients underwent open heart surgery in association with cardiopulmonary bypass. Until July 2013 they received an HES product (N=247) both as pump prime (1500 mL) and intraoperative fluid replacement (1000 mL), but only crystalloid (N=359) from August 2013 onward. The frequency (percent) of postoperative AKI was higher in patients receiving HES (N=53; 21.5%) than those receiving crystalloid (N=34; 9.5%). Surgical revision for rebleeding also was higher for HES (N=11; 4.6%) than for crystalloid (N=5; 1.4%).18
In a meta-analysis of RCTs (n=15) in adult subjects (N=4409) undergoing surgery who received an HES product, significantly more HES subjects (83/2157; 3.8%) than controls (56/2252; 2.5%) underwent RRT (relative risk, 1.44; 95% CI, 1.04, 2.01).19
In a retrospective observational study of adult blunt and penetrating trauma patients, use of an HES product was a significant independent predictor of AKI after blunt trauma, but not penetrating trauma, in multiple logistic regression analysis. In separate logistic regression models, HES also was a significant predictor of mortality after blunt trauma but not penetrating trauma.20
In a retrospective observational study of severely injured adult blunt (89%) and penetrating (11%) trauma patients (N=413) admitted to the ICU, 103 patients developed AKI within the first week of ICU admission. AKI was associated with increased 30-day (17.5% versus 5.8%, AKI versus non-AKI cohorts, respectively) and 1-year mortality (26.2% versus 7.1%). Univariate and multivariable regression analyses of prespecified risk factors for AKI found that volume loading using an HES product was independently associated with postinjury AKI within the first 24 hours.21
6.2 Postmarketing Experience
Because adverse reactions are reported voluntarily post-approval from a population of uncertain size, it is not always possible to reliably estimate the frequency of these reactions or establish a causal relationship to product exposure.
The following adverse reactions have been identified and reported during the post-approval use of HES products:
Hypersensitivity reactions
including death, life-threatening anaphylactic/anaphylactoid reactions, cardiac arrest, ventricular fibrillation, severe hypotension, non-cardiac pulmonary edema, laryngeal edema, bronchospasm, angioedema, wheezing, restlessness, tachypnea, stridor, fever, chest pain, bradycardia, tachycardia, shortness of breath, chills, urticaria, pruritus, facial and periorbital edema, coughing, sneezing, flushing, erythema multiforme, and rash [see Warnings and Precautions (5.3)].
Cardiovascular reactions
including circulatory overload, congestive heart failure, and pulmonary edema [see Warnings and Precautions (5.4)].
Hematologic reactions
including intracranial bleeding, bleeding and/or anemia due to hemodilution [see Warnings and Precautions (5.4)] and/or Factor Vlll deficiency, acquired von Willebrand’s-like syndrome, and coagulopathy including rare cases of disseminated intravascular coagulopathy and hemolysis.
Other reactions
including vomiting, peripheral edema of the lower extremities, submaxillary and parotid glandular enlargement, mild influenza-like symptoms, headaches, and muscle pains. Hydroxyethyl starch-associated pruritus has been reported in some patients with deposits of hydroxyethyl starch in peripheral nerves.
Related/similar drugs
7. Drug Interactions
HESPAN® should be used with caution in patients who have been anticoagulated with other drugs that negatively influence the coagulation system.
- The safety and compatibility of other additives have not been established.
8. Use In Specific Populations
8.1 Pregnancy
Hetastarch has been shown to have an embryocidal effect on New Zealand rabbits when given intravenously over the entire organogenesis period in a daily dose 1/2 times the maximum recommended therapeutic human dose (1500 mL) and on BD rats when given intraperitoneally, from the 16th to the 21st day of pregnancy, in a daily dose 2.3 times the maximum recommended therapeutic human dose. When hetastarch was administered to New Zealand rabbits, BD rats, and swiss mice with intravenous daily doses of 2 times, 1/3 times, and 1 times the maximum recommended therapeutic human dose respectively over several days during the period of gestation, no evidence of teratogenicity was evident.
There are no adequate and well-controlled studies in pregnant women. HESPAN® should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus.
11. Hespan Description
HESPAN® (6% hetastarch in 0.9% sodium chloride injection) is a sterile, nonpyrogenic solution for intravenous administration.
Each 100 mL contains:
Hetastarch..... 6 g
Sodium Chloride, USP..... 0.9 g
Water for Injection, USP..... qs
pH adjusted with Sodium Hydroxide, NF if necessary
Concentration of Electrolytes (mEq/L): Sodium 154, Chloride 154
pH: approximately 5.9 with negligible buffering capacity
Calc. Osmolarity: approximately 309 mOsM
Hetastarch is a synthetic colloid derived from a waxy starch composed almost entirely of amylopectin. Hydroxyethyl ether groups are introduced into the glucose units of the starch, and the resultant material is hydrolyzed to yield a product with a molecular weight suitable for use as a plasma volume expander and erythrocyte sedimenting agent. The molar substitution is approximately 0.75 which means hetastarch has an average of approximately 75 hydroxyethyl groups for every 100 glucose units. The weight average molecular weight is approximately 600,000 with a range of 450,000 to 800,000 and with at least 80% of the polymers falling within the range of 20,000 to 2,600,000. Hydroxyethyl groups are attached by ether linkage primarily at C-2 of the glucose unit and to a lesser extent at C-3 and C-6. The polymer resembles glycogen, and the polymerized D-glucose units are joined primarily by α-1,4 linkages with occasional α-1,6 branching linkages.
The chemical name for hetastarch is hydroxyethyl starch.
The structural formula is as follows:
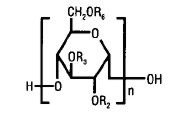
Amylopectin derivative in which R2 and R3 are H or CH2CH2OH and R6 is H, CH2CH2OH, or a branching point in the starch polymer connected through an α-1,6 link to additional D-glucopyranosyl units.
HESPAN® is a clear, pale yellow to amber solution. Exposure to prolonged adverse storage conditions may result in a change to a turbid deep brown or the formation of a crystalline precipitate. Do not use the solution if these conditions are evident.
Not made with natural rubber latex, PVC or DEHP.
The plastic container is made from a multi-layered film specifically developed for parenteral drugs. It contains no plasticizers and exhibits virtually no leachables. The solution contact layer is a rubberized copolymer of ethylene and propylene. The container is nontoxic and biologically inert. The container-solution unit is a closed system and is not dependent upon entry of external air during administration. The container is overwrapped to provide protection from the physical environment and to provide an additional moisture barrier when necessary.
The closure system has two ports; the one for the administration set has a tamper evident plastic protector.
12. Hespan - Clinical Pharmacology
12.1 Mechanism of Action
The plasma volume expansion produced by HESPAN® approximates that of 5% Albumin (Human). Intravenous infusion of HESPAN® results in expansion of plasma volume.
12.2 Pharmacodynamics
HESPAN® results in expansion of plasma volume that decreases over the succeeding 24 to 36 hours. The degree of plasma volume expansion and improvement in hemodynamic state depend upon the patient’s intravascular status.
12.3 Pharmacokinetics
Hetastarch molecules below 50,000 molecular weight are rapidly eliminated by renal excretion. A single dose of approximately 500 mL of HESPAN® (approximately 30 g) results in elimination in the urine of approximately 33% of the dose within 24 hours. This is a variable process but generally results in an intravascular hetastarch concentration of less than 10% of the total dose injected by two weeks. A study of the biliary excretion of HESPAN® in 10 healthy males accounted for less than 1% of the dose over a 14 day period. The hydroxyethyl group is not cleaved by the body but remains intact and attached to glucose units when excreted. Significant quantities of glucose are not produced as hydroxyethylation prevents complete metabolism of the smaller polymers.
The addition of hetastarch to whole blood increases the erythrocyte sedimentation rate. Therefore, HESPAN® is used to improve the efficiency of granulocyte collection by centrifugal means.
14. Clinical Studies
Surgical Patients Comparative Studies
In randomized, controlled, comparative studies of HESPAN® (6% hetastarch in 0.9% sodium chloride injection) (n=92) and Albumin (n=85) in surgical patients, no patient in either treatment group had a bleeding complication and no significant difference was found in the amount of blood loss between the treatment groups.7-10
Pediatric Postoperative Volume Expander Study
In one small double-blind study, 47 infants, children, and adolescents (ages 1 year to 15.5 years) scheduled for repair of congenital heart disease with moderate hypothermia were randomized to receive either HESPAN® or Albumin as a postoperative volume expander during the first 24 hours after surgery. Thirty-eight children required colloid replacement therapy, of which 20 children received HESPAN®. No differences were found in the coagulation parameters or in the amount of replacement fluids required in the children receiving 20 mL/kg or less of either colloid replacement therapy. In children who received greater than 20 mL/kg of HESPAN®, an increase in prothrombin time was demonstrated (p=0.006).11 There were no neonates included in this study [see Use in Specific Populations (8.4)].
Adult Critically Ill Studies
Three randomized controlled trials (RCTs) followed critically ill adult patients treated with different HES products for 90 days.
One trial (N=804) in severe sepsis patients using HES product (not approved in the U.S.) reported increased mortality (relative risk, 1.17; 95% CI, 1.01 to 1.36; p=0.03) and RRT (relative risk, 1.35; 95% CI, 1.01 to 1.80; p=0.04) in the HES treatment arm.4
Another trial (N=196) using different HES in severe sepsis patients reported no difference in mortality (relative risk,1.20; 95% CI, 0.83 to 1.74; p=0.33) and a trend for RRT (relative risk, 1.83; 95% CI, 0.93 to 3.59; p=0.06) in HES patients.5
A third trial (N=7000) using different HES in a heterogeneous patient population consisting of critically ill adult patients admitted to the ICU reported no difference in mortality (relative risk, 1.06; 95% CI, 0.96 to 1.18; p=0.26) but increased use of RRT (relative risk, 1.21; 95% CI, 1.00 to 1.45; p=0.04) in HES patients.6
15. References
- Knutson JE., et al., Does Intraoperative Hetastarch Administration Increase Blood Loss and Transfusion Requirements After Cardiac Surgery? Anesthesia Analg., 2000;90:801-7.
- Cope JT., et al., Intraoperative Hetastarch Infusion Impairs Hemostasis After Cardiac Operations. The Annals of Thoracic Surgery, 1997;63:78-83.
- Damon L., Intracranial Bleeding During Treatment with Hydroxyethyl Starch. New England Journal of Medicine, 1987;317(15):964-965.
- Perner A, et al., Hydroxyethyl starch 130/0.42 versus Ringer's acetate in severe sepsis patients. The New England Journal of Medicine, 2012 July 12;367(2):124-34.
- Guidet B, et al., Assessment of hemodynamic efficacy and safety of 6% hydroxyethyl starch 130/0.4 vs 0.9% NaCl fluid replacement in patients with severe sepsis: The CRYSTMAS Study. Critical Care, 2012 May 24;16(3):R94.
- Myburgh JA, et al., Hydroxyethyl starch or saline for fluid resuscitation in intensive care. The New England Journal of Medicine, 2012 November 15;367(20):1901-11.
- Diehl J., et al., Clinical Comparison of Hetastarch and Albumin in Postoperative Cardiac Patients. The Annals of Thoracic Surgery, 1982;34(6):674-679.
- Gold M., et al., Comparison of Hetastarch to Albumin for Perioperative Bleeding in Patients Undergoing Abdominal Aortic Aneurysm Surgery. Annals of Surgery, 1990;211(4):482-485.
- Kirklin J., et al., Hydroxyethyl Starch versus Albumin for Colloid Infusion Following Cardiopulmonary Bypass in Patients Undergoing Myocardial Revascularization. The Annals of Thoracic Surgery, 1984;37(1):40-46.
- Moggio RA., et al., Hemodynamic Comparison of Albumin and Hydroxyethyl Starch in Postoperative Cardiac Surgery Patients. Critical Care Medicine, 1983;11(12):943-945.
- Brutocao D., et al., Comparison of Hetastarch with Albumin for Postoperative Volume Expansion in Children After Cardiopulmonary Bypass. Journal of Cardiothoracic and Vascular Anesthesia, 1996;10(3):348-351.
- Ahn HJ, Kim JA, Lee AR, et al. The risk of acute kidney injury from fluid restriction and hydroxyethyl starch in thoracic surgery.
Anesth Analg 2016; 122(1):186-193. - Green RS, Butler MB, Hicks SD, et al. Effect of hydroxyethyl starch on outcomes in high-risk vascular surgery patients: A
retrospective analysis. J Cardiothorac Vasc Anesth 2016; 30(4):967-72. - Kashy BK, Podolyak A, Makarova N, et al. Effect of hydroxyethyl starch on postoperative kidney function in patients having
noncardiac surgery. Anesthesiology 2014; 121 (4):730-9. - Patel MS, Niemann CU, Sally MB, et al. The impact of hydroxyethyl starch use in deceased organ donors on the development of
delayed graft function in kidney transplant recipients: A Propensity-Adjusted Analysis. Am J of Transplant 2015; 15 (8):2152-8. - Rasmussen KC, Johansson PI, Højskov M, et al. Hydroxyethyl starch reduces coagulation competence and increases blood loss
during major surgery: results from a randomized controlled trial. Ann Surg 2014; 259 (2):249-54. - Bayer O, Schwarzkopf D, Doenst T, et al. Perioperative fluid therapy with tetrastarch and gelatin in cardiac surgery — a
prospective sequential analysis. Crit Care Med 2013; 41(11):2532-42. - Lagny MG, Roediger L, Koch JN, et al. Hydroxyethyl starch 130/0.4 and the risk of acute kidney injury after cardiopulmonary
bypass: A single-center retrospective study. J of Cardiothorac and Vasc Anesth 2016: 30(4):869-75. - Wilkes MM, Navickis RJ. Postoperative renal replacement therapy after hydroxyethyl starch infusion: a meta-analysis of
randomized trials. Neth J Crit Care 2014; 18:4-9. - Allen CJ, Valle EJ, Jouria JM, et al. Differences between blunt and penetrating trauma after resuscitation with HES. J Trauma
Acute Care Surg 2014; 77(6):859-64. - Eriksson M, Brattström O, Mårtensson J, et al. Acute kidney injury following severe trauma: Risk factors and long-term outcome. J
Trauma Acute Care Surg 2015; 79(3):407-12.
16. How is Hespan supplied
HESPAN® (6% hetastarch in 0.9% sodium chloride injection) is supplied sterile and nonpyrogenic in 500 mL EXCEL® Containers packaged 12 per case.
NDC REF Volume
0264-1965-10 L6511 500 mL
Exposure of pharmaceutical products to heat should be minimized. Avoid excessive heat. Protect from freezing.
Store at room temperature (25°C); however, brief exposure up to 40°C does not adversely affect the product.
Storage in automated dispensing machines: Brief exposure up to 2 weeks to ultraviolet or fluorescent light does not adversely affect the product labeling legibility; prolonged exposure can cause fading of the red label. Rotate stock frequently.
Rx only
EXCEL and HESPAN are registered trademarks of B. Braun Medical Inc.
B. Braun Medical Inc.
Bethlehem, PA 18018-3524 USA
1-800-227-2862
Y36-003-048 LD-233-5
PRINCIPAL DISPLAY PANEL - 500 mL
6% hetastarch in
0.9% sodium chloride injection
HESPAN®
NDC 0264-1965-10
500 mL
EXCEL® CONTAINER
For intravenous use only.
Each 100 mL contains: Hetastarch 6 g
Sodium Chloride USP 0.9 g in Water for Injection, USP
pH adjusted with Sodium Hydroxide, NF
Electrolytes (mEq/L): Sodium 154 Chloride 154
If administration is by pressure infusion, all air should be withdrawn
or expelled from the bag through the medication port prior to infusion.
Sterile. Single dose container. Discard unused solution.
Recommended Storage: Store at room temperature, 25°C (77°F). Avoid
excessive heat. Protect from freezing. Usual Dosage: See package insert for
complete information.
Do not remove overwrap until ready for use. If leaks are found, discard solution as
sterility may be impaired. DO NOT INTRODUCE ADDITIVES OTHER THAN CITRATE INTO BAG.
REF L6511
Not made with natural rubber latex, PVC or DEHP.
Rx only

B. Braun Medical Inc.
Bethlehem, PA 18018-3524 USA
1-800-227-2862
www.bbraun.com
Y94-003-305 LD-152-7
EXP LOT

| HESPAN
hetastarch in sodium chloride injection, solution |
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
|
||||||||||||||||||||
| Labeler - B. Braun Medical Inc. (002397347) |
| Establishment | |||
| Name | Address | ID/FEI | Business Operations |
|---|---|---|---|
| B. Braun Medical Inc. | 037425308 | label(0264-1965) , manufacture(0264-1965) , pack(0264-1965) | |
More about Hespan (hetastarch)
- Compare alternatives
- Side effects
- Dosage information
- During pregnancy
- Drug class: plasma expanders
- En español
