Muscle Strain
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a muscle strain?
A muscle strain is a twist, pull, or tear of a muscle or tendon. A tendon is a strong elastic tissue that connects a muscle to a bone.
What are the types of muscle strains?
- A mild strain is also called a first-degree strain. It is a tear of a few muscle fibers with little swelling. You may have very little or no loss of muscle strength.
- A moderate strain is also called a second-degree strain. There is more damage to your muscle or tendon, and it is weaker than it was before the injury.
- A severe strain is also called a third-degree strain. This tear goes along the whole length of the muscle, and you are unable to use the muscle at all.
What increases my risk for a muscle strain?
- Overuse of a muscle without rest in between uses
- Activities that use certain muscles more than others, such as dance, volleyball, tennis, or golf
- Lifting heavy objects
- Older age
- Not warming up before exercise
- Past muscle injury, or going back to your usual activity before your injury has healed
- Stiff, tight, and weak muscles
- Training longer or farther than your usual time or distance
- Problems with your feet, or your legs being different lengths
What are the signs and symptoms of a muscle strain?
The signs and symptoms of a muscle strain depend on how badly your muscle is injured. The signs and symptoms may or may not show up right away when the injury happens. You may have one or more of the following:
- Bruised skin on the area of your injured muscle
- Muscle soreness, cramps, or spasms
- Little or stiff muscle movement, or loss of muscle strength
- Swelling in the area of the injury
- Muscle pain that gets worse with activity, or pain that moves or spreads to another body area
- Crepitus (crackling sound or grating feeling) when you move your muscle
How is a muscle strain diagnosed?
Your healthcare provider will examine you and ask about your medical history. He or she may touch and press parts of your muscle. He or she may bend, stretch, or move your joint certain ways. You may also need any of the following tests:
- X-ray pictures may be used to make sure you did not break a bone when your muscle strain happened.
- MRI or CT scan pictures may be used to check for tears or other muscle injuries. Pictures may also be used to look at your joints, bones, or blood vessels. You may be given contrast liquid before the pictures are taken to help your muscles show up better in the pictures. Tell your healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell your provider if you have any metal in or on your body.
- Ultrasound pictures may be used if other pictures do not show any injury.
What can I do to help a muscle strain heal?
- 3 to 7 days after the injury: Use Rest, Ice, Compression, and Elevation (RICE) to help stop bruising and decrease pain and swelling.
- Rest your muscle to allow the injury to heal. When the pain decreases, begin normal, slow movements. For mild and moderate muscle strains, you should rest your muscles for about 2 days. If you have a severe muscle strain, you should rest for 10 to 14 days. You may need to use crutches to walk if your muscle strain is in your legs or lower body.
- Apply ice on the injured area. Use an ice pack, or put crushed ice in a plastic bag. Cover the bag with a towel before you apply it to your skin. Apply ice for 15 to 20 minutes each hour, or as directed.
- Use compression to decrease swelling. You can wrap an elastic bandage around the area to create compression. The bandage should be tight enough for you to feel support. Do not wrap it too tightly.
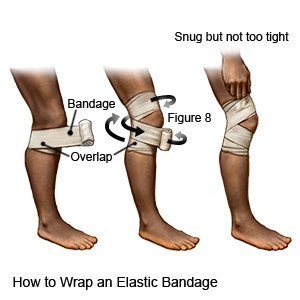
- Elevate the area above the level of your heart, if possible. Keep the injured muscle raised above your heart if possible. For example, if you have a strain of your lower leg muscle, lie down and prop your leg up on pillows. This helps decrease pain and swelling.

- 3 to 21 days after your injury: Start to slowly and regularly exercise your strained muscle. This will help it heal. If you feel pain, decrease how hard you are exercising.
- 1 to 6 weeks after your injury: Stretch the injured muscle. Stretch the muscle for about 30 seconds. Do this 4 times a day. You may stretch the muscle until you feel a slight pull. Stop stretching if you feel pain.
- 2 weeks to 6 months after your injury: The goal of this phase is to return to the activity you were doing before the injury without hurting the muscle again.
- 3 weeks to 6 months after your injury: Keep stretching and strengthening your muscles to prevent injury. Slowly increase the time and distance that you exercise. You may still have signs and symptoms of muscle strain 6 months after the injury, even if you do things to help it heal. In this case, you may need surgery on the muscle.
How is a muscle strain treated?
- Medicines:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Muscle relaxers help decrease pain and muscle spasms.
- Steroid injections help decrease pain and inflammation.
- Local anesthetic can be used to numb the are for a short time. This is often used if you have a muscle strain in your back.
- A physical therapist can teach you exercises to help improve movement and strength, and to decrease pain.
- Surgery may be needed if your muscle strain does not heal after 6 months. Surgery may be done to drain blood that has pooled in your muscle. If your tendon was torn off of the bone, it may be put back with surgery.
How can a muscle strain be prevented?
- Always wear proper shoes when you play sports. Replace your old running shoes with new ones often if you are a runner. Use special shoe inserts or arch supports to correct leg or foot problems. Ask your healthcare provider for more information on shoe supports.
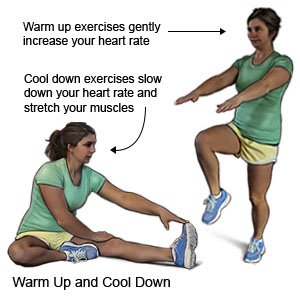
- Do warm up and cool down exercises. Do stretching exercises before you work out or do sports activities. These exercises will help loosen and decrease stress on your muscles. Cool down and stretch after your workout. Do not stop and rest after a workout without cooling down first.
- Keep your muscles strong with strength training exercises. Exercises such as weight lifting and stretching exercises help keep your muscles flexible and strong. A physical therapist or trainer may help you with these exercises.

- Slowly start your exercise or sports training program. Follow your healthcare provider's advice on when to start exercising. Slowly increase time, distance, and how often you train. Sudden increases in how often you train may cause you to injure your muscle again.
When should I seek immediate care?
- You suddenly cannot feel or move your injured muscle.
When should I call my doctor?
- Your pain and swelling worsen or do not go away.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Muscle Strain
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
