Osteomyelitis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is osteomyelitis?
Osteomyelitis is a severe bone infection. It can develop in any bone, but often involves the long bones, such as your arm and leg bones, or the bones of the spine. Osteomyelitis is caused by different types of germs, such as bacteria or a fungus.
What increases my risk for osteomyelitis?
- Recent trauma or surgery
- Poor blood flow to your arms or legs
- Weak immune system
- Medical conditions, such as diabetes, sickle cell anemia, or a prosthetic implant
- A central vein or dialysis catheter
- Age older than 50
- Poor nutrition
- IV drug abuse
What are the signs and symptoms of osteomyelitis?
- Fever
- Pain, redness, and swelling
- Trouble moving or putting weight on your limb
- Bruising or discoloration
- Pus coming from a wound or sore
- Night sweats
- A bone that looks out of place
How is osteomyelitis diagnosed?
- Blood tests are used to show the type of germ causing the infection.
- X-ray, CT, or MRI takes pictures of your bone and tissue to look for infection and damage. You may be given contrast liquid to help the bone and tissue show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. Do not enter the MRI room with anything metal. Metal can cause serious injury. Tell the healthcare provider if you have any metal in or on your body.
- A bone scan shows diseased or damaged bones. A radioactive liquid, called a tracer, is given through an IV. The tracer collects in your bones so problems show up better in pictures.
- A bone biopsy takes a sample of your bone to learn what is causing your infection. It can also help healthcare providers learn how to best treat the infection.
How is osteomyelitis treated?
You may need any of the following:
- Medicine will be given to fight the infection and to decrease pain or fever.
- Hyperbaric oxygen therapy may be needed to help the wound heal. During therapy your infected bone is exposed to a high amount of oxygen.
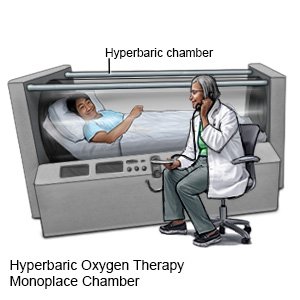
- Surgery may be needed to drain or remove the infected, damaged, or dead bone tissue. Screws, pins, or a graft may be placed. A limb may be amputated if the bone infection spreads or becomes severe.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my symptoms?
- Eat a variety of healthy foods. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Ask if you need to be on a special diet.

- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage and make it difficult to heal. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Manage other medical conditions , such as diabetes, to prevent more bone damage.
When should I seek immediate care?
- You have severe pain.
- Your bone breaks.
When should I call my doctor?
- Your symptoms return.
- You have increased swelling, pain, or redness of your infected area.
- You have new drainage or an odor from your wound.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Osteomyelitis
Treatment options
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
