Cardiomyopathy
Medically reviewed by Drugs.com. Last updated on Jan 10, 2025.
What is cardiomyopathy?

Cardiomyopathy refers to changes in the heart muscle. These changes prevent part or all of the heart from contracting normally.
There are three types of cardiomyopathy. The types are based on the physical changes that occur in the heart:
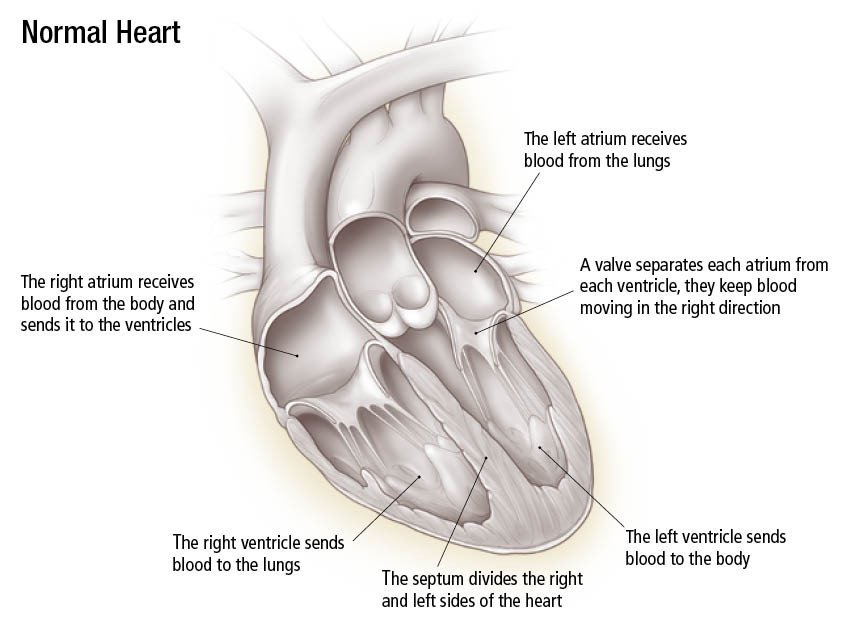
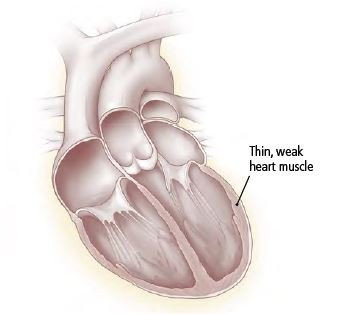
- Dilated cardiomyopathy — The damaged heart muscle stretches out of shape. The heart becomes enlarged. It loses its ability to pump blood effectively. This eventually leads to heart failure. Risk factors for dilated cardiomyopathy include:
- coronary artery disease
- high blood pressure
- prolonged, excessive alcohol use
- myocarditis (heart muscle inflammation)
- untreated thyroid disorders
- inherited genetic diseases
- disorders in which the heart muscle is overloaded with iron or amyloid protein
- radiation and chemotherapy treatments.
- Hypertrophic cardiomyopathy — The muscular heart wall thickens abnormally. As a result, the heart muscle cannot relax fully. As a result, the heart does not fill up with as much blood as in a healthy heart. So the heart has less blood to pump out to the body. There is another problem with hypertrophic cardiomyopathy, as well. The heart muscle wall can become so thickened that it blocks the flow of blood out of the heart. Both of these problems can lead to heart failure.
- Restrictive cardiomyopathy — Various diseases can cause substances to be deposited where they do not belong: in the heart muscle. This causes the heart's muscular walls to become so rigid that the heart cannot expand to fill up with all the blood that is returning from the body. The result is that the heart does not have as much blood to pump as the body needs.
Symptoms of cardiomyopathy
The symptoms of cardiomyopathy vary by type.
- Dilated cardiomyopathy — Symptoms can include
- shortness of breath, especially during exertion
- fatigue
- difficulty breathing while lying down
- leg swelling
- palpitations
- chest pain.
- Hypertrophic cardiomyopathy — Symptoms, when they occur, are usually the same as the symptoms of dilated cardiomyopathy. Sometimes, the first symptom may be fainting or even sudden death. The condition also can cause chest pain, usually during exercise.
- Restrictive cardiomyopathy — Fluid accumulates in the legs and abdomen. This condition also can cause shortness of breath, especially during exertion.
Diagnosing cardiomyopathy
Your doctor will review your medical history.
He or she will ask about
- your family's history of heart disease
- any family members whose death was sudden and unexplained
- specific circumstances that trigger your heart-related symptoms.
Your doctor will examine you, paying special attention to your heart.
This will be followed by
- an electrocardiogram (EKG). This test records the electrical activity of your heart.
- a chest X-ray
- blood tests
- an echocardiogram. This test uses sounds waves to create a picture of the heart at work.
You may also need other tests.
Expected duration of cardiomyopathy
Dilated cardiomyopathy sometimes can be reversed if it is caused by a treatable condition.
Most cases of hypertrophic and restrictive cardiomyopathy are persistent. They can get worse over time.
Preventing cardiomyopathy
The best way to prevent cardiomyopathy is to prevent the diseases that cause it.
Know your risk factors for coronary artery disease. Modify those risks early in life.
You can reduce your risk for coronary artery disease by
- keeping blood pressure normal. Eat a diet rich in vegetables and fruits. Take medication as needed.
- crinking no more than two alcoholic beverages per day. Do not drink alcohol at all if you are at high risk of dilated cardiomyopathy.
If you have any family members with inherited cardiomyopathy, contact your doctor for an evaluation.
Treating cardiomyopathy
The treatment of cardiomyopathy depends on its cause. Here are some of the more common treatments:
- medications that prolong life in people with dilated cardiomyopathy
- angiotensin-converting enzyme (ACE) inhibitors
- angiotensin receptor blockers
- beta blockers
- aldosterone receptor antagonists
- sacubitril/valsartan (Entresto)
- drugs that improve the symptoms of heart failure in dilated cardiomyopathy
- diuretics
- ACE inhibitors
- angiotensin receptor blockers
- digoxin
- sacubitril/valsartan (Entresto)
- drugs that help to relax the heart muscle in hypertrophic cardiomyopathy
- beta blockers
- verapamil, a calcium-channel blocker drug
- antiarrhythmic drugs to correct abnormal heart rhythms.
- a pacemaker or an implantable defibrillator to prevent fatal arrhythmias.
SGLT2 inhibitors are the newest class of drugs that improve outcome in people with cardiomyopathy, especially those with dilated cardiomyopathy.
For patients with hypertrophic cardiomyopathy, blockage to the outflow of blood can sometimes be reduced. This is done by damaging part of the muscle between the two ventricles. This damage can be created at surgery or through a catheter.
A heart transplant may be necessary for patients whose poor heart function has become disabling or life threatening.
When to call a professional
Call your doctor whenever you have any of the following symptoms:
- shortness of breath, with or without exertion
- difficulty breathing when you sleep or lie down
- fainting or light-headed spells
- palpitations
- leg swelling.
Call your doctor immediately if you have chest pain. Call even if you think that you are too young to be having heart problems.
Prognosis
The outlook varies. It depends on the specific cause and severity of the cardiomyopathy.
The survival rate of people with most types has improved dramatically in the past decade. This is due to the increased number of treatments available.
Additional info
American Heart Association (AHA)
https://www.heart.org/
National Heart, Lung, and Blood Institute (NHLBI)
https://www.nhlbi.nih.gov/
American College of Cardiology
https://www.acc.org/
Learn more about Cardiomyopathy
Treatment options
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
