Tick bites
Medically reviewed by Drugs.com. Last updated on Mar 5, 2025.
What are Tick bites?

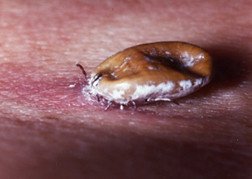
Ticks are tiny, biting arachnids that feed on the blood of warm-blooded animals, including humans. They burrow painlessly into the skin with their feeding parts, bite, draw blood and eventually drop off when they become engorged with blood. Only the feeding parts are inserted into the skin. The body, which is dark in color and ranges from the size of a poppy seed to a pencil eraser, remains visible on the skin surface or scalp. Ticks swell and turn bluish-gray when filled with blood. Most tick bites in the United States involve hard ticks (Ixodidae), which have been increasing in number since the middle 1900s.
|
|
|
Secretions from the tick's feeding parts can cause skin reactions, such as raised areas, lumps, and growths called granulomas. Fever and paralysis also may develop after tick bites, although paralysis is rare. Paralysis is due to a toxin transmitted from the tick's secretions, not due to an infection. However, ticks can be infected with bacteria, viruses, or protozoa, and these organisms can be transmitted from the tick to the host (the animal or person) as the tick feeds, causing disease.
Tick-borne infectious diseases include:
- Lyme disease
- anaplasmosis (formerly known as human granulocytic ehrlichiosis)
- Babesiosis
- human monocytic ehrlichiosis
- tularemia
- Rocky Mountain spotted fever
- Colorado tick fever
- relapsing fever
Ticks live in tall grass and in wooded areas, particularly cool, moist, mature woods with thick undergrowth. They also can be found at the edges of woods near lawns or fields, but rarely in lawns, which are too dry and hot. Ticks wait in the underbrush for an animal or human to brush by, and then grasp the fur or skin and crawl up the leg. They don't fly, jump or drop from trees. They wander the body for 30 minutes to an hour before inserting their feeding parts into the skin.
Symptoms
Most tick bites do not cause any symptoms. However, the following symptoms can develop as a reaction to tick secretions:
- fever
- headache
- muscle pain
- joint pain
- fatigue
- muscle weakness.
Skin reactions include:
- pus-filled bumps
- hardened skin elevations
- nodules (granulomas) that, in rare cases, can grow large enough to require surgical removal.
Tick paralysis is relatively rare. Paralysis begins in the feet and legs and gradually works its way to the upper body, arms and head over a period of hours or days. Once the tick is removed, a person with tick paralysis will recover completely. If the tick is not removed, the person can die if the muscles that control breathing are paralyzed.
Symptoms associated with tick-borne infections differ depending on the type of infection. Common symptoms are as follows:
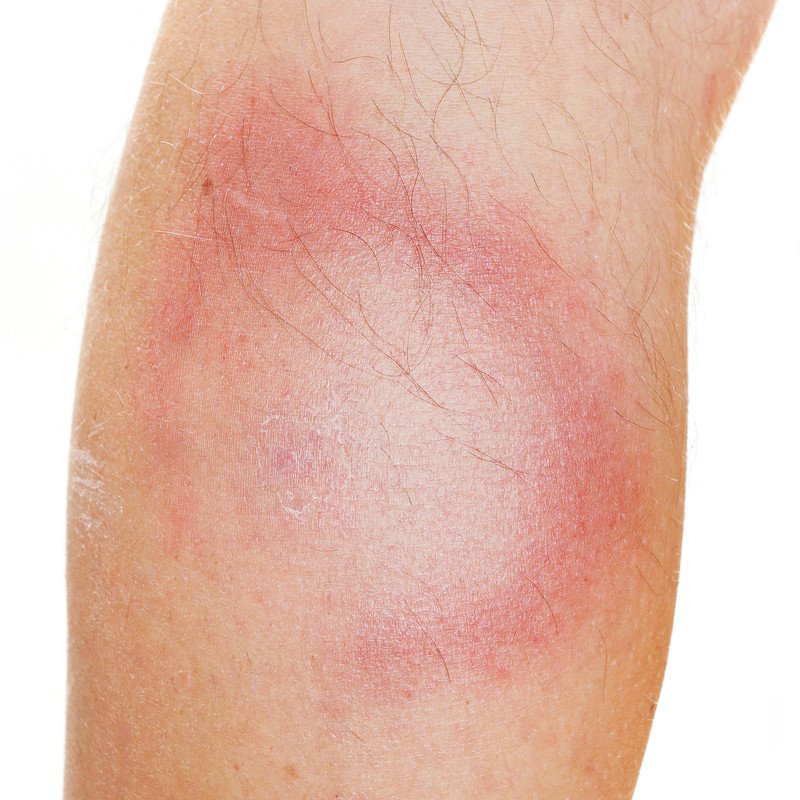
- Lyme disease – A variety of symptoms can occur, including a flulike illness, an expanding red rash that may include a central clear area (a bull's-eye rash), arthritis, heart rhythm problems, difficulties in thinking or perception, and neuropathies (pain or changes in sensation as a result of nerve damage).
|
|
-
Human monocytic ehrlichiosis – Symptoms ranging from mild to severe can involve many organ systems. Common symptoms include high fever, headache, fatigue, nausea, weight loss and a spotted rash. Patients with weak immune systems can develop a fatal, overwhelming infection. Breathing difficulties and mental changes may also occur.
-
Anaplasmosis – Symptoms ranging from mild to severe include high fever, headache, a general sick feeling (malaise), achy muscles (myalgia), nausea, vomiting, cough, stiff neck and confusion. Less than 10% of people with this disease will develop a rash.
-
Colorado tick fever – Flulike symptoms include fever and chills, severe headache, achy muscles (myalgia), stiff neck, light intolerance and, in some cases, a spotted rash.
-
Babesiosis – Many people will not have any symptoms. Others develop fatigue, fever, drenching sweats, nausea, vomiting, headache, muscle aches, joint aches and jaundice. Patients with suppressed immune systems may develop severe disease.
-
Tularemia – The symptoms of this disease vary widely. Some people do not have any symptoms, but this disease also can be severe, causing septic shock and death. Common symptoms include fever, chills, headache and a general sick feeling (malaise). Many people also develop a single, red ulcerated lump with a central scab and tender, swollen lymph nodes in the area. A small number of patients develop pneumonia.
-
Rocky Mountain spotted fever – Symptoms include fever, headache, a spotted rash on wrists and ankles, and a patchy rash on arms and legs. Muscle aches (myalgia), nausea, vomiting and abdominal pain are also common.
Diagnosis
If you see your doctor for a tick bite, you will be asked about the size of the tick, whether it was attached to your skin and how long you think it had been attached. Your doctor will examine your skin for rashes and ask you about any symptoms that could suggest that you have developed a tick-borne infection. No further diagnostic tests are necessary unless you develop symptoms. If you develop symptoms that suggest a tick-borne illness, your physician will order a variety of blood tests to determine the cause.
Expected duration
A tick bite can cause many different tick-borne infections. How long each illness lasts depends on the infecting organism. In general, the tick bite itself does not cause any symptoms, although some people may develop fever, headache, nausea and a general sick feeling caused by tick secretions. These symptoms usually go away within 24 to 36 hours after the tick is removed.
Tick-induced paralysis begins in the legs five to six days after the tick has attached to the skin, and it progresses to complete paralysis over several days. Paralysis begins to improve within a few hours of removing the tick, and complete recovery takes several days.
The organisms that cause Lyme disease and babesiosis rarely are transmitted to the person or animal if ticks are removed within the first 24 hours after they attach and before they become engorged.
Prevention
To prevent tick bites in tick-infested areas, take the following precautions:
- When in the woods, walk on cleared trails. Avoid walking through tall grass and low brush in wooded areas.
- Wear light-colored clothing covering both the arms and legs.
- Tuck pant legs into socks.
- Treat clothing and skin with tick repellents containing diethyltoluamide (DEET), or use the pesticide permethrin on clothing (but not skin).
- Thoroughly check yourself, children, and pets for ticks after spending time in tick-infested areas. Remember to check the scalp. If one tick is found, check for more.
Treatment
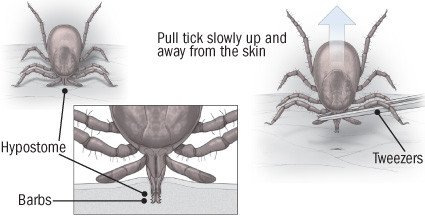
When a tick is discovered on the skin or scalp, it should be removed immediately to avoid a skin reaction and to reduce the likelihood of developing a tick-borne infectious disease. Grasp the head of the tick with a pair of flat or curved forceps or tweezers held as close to the skin as possible. Avoid squeezing the tick. Gently pull the head of the tick away from the skin without twisting. The bite should be cleaned with soap and water. Save the tick in a container with a tight-fitting lid.
|
|
For people in areas where Lyme disease rates are high, one dose of doxycycline can prevent disease if taken within three days of a tick bite. So for those at highest risk, early treatment may be appropriate. This is especially important if the tick was engorged, as this suggests it was attached for long enough to transmit the bacterium that causes Lyme disease.
When to call a professional
Seek medical attention if a tick has buried itself deep in the skin and you cannot remove it or if you find an engorged tick on your skin and are living in or visiting an area where Lyme disease is a risk. Fever and flulike symptoms require medical attention if you know you've recently been bitten by a tick or if the symptoms are accompanied by a skin rash, particularly the bull's-eye rash characteristic of Lyme disease. Muscle weakness or paralysis requires immediate medical attention.
Prognosis
If no infectious organisms have been transmitted by the tick, you should recover from symptoms within a day or two. The outlook for specific tick-borne illnesses varies.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.