Sprain
Medically reviewed by Drugs.com. Last updated on Dec 12, 2024.
What is a sprain?

A sprain is an injury to ligaments, the tough bands of fibrous tissue that connect bones to one another at a joint. Normally, ligaments stabilize a joint, keep the joint's bones aligned and limit the motion of a joint to the normal range. When a joint is sprained, its torn or stretched ligaments can lose part or all of their ability to reinforce the joint and to keep it moving normally. In severe cases, the sprained joint can become unstable and loose, bones can move out of alignment, and the joint may extend beyond its normal range of motion.
Although ligaments can be sprained in a variety of ways, the actual ligament damage is usually caused by at least one of the following:
- Flexing (bending), extending (stretching out), or twisting a joint beyond its normal range of motion — This injury is a common cause of wrist sprains in skiers. If a skier falls with a ski pole still strapped to the wrist, the attached pole can twist the wrist beyond its normal limits and cause a sprain.
- Suddenly increasing the tension (strain or pull) on a ligament to the point that it snaps in two — This type of injury can happen in the knee joint if you suddenly stop short while running. The extreme tension of the braking force actually tears one of the knee ligaments in two, often causing a pop that can be felt or even heard when the ligament snaps.
- Hitting the joint directly or hitting one of the bones near the joint — This type of sprain often happens in contact sports, especially when a shoulder or knee joint takes the full impact of a collision between two athletes.
Any unusual force across a joint can cause a sprain. Among athletes, more than any other group, sprains are common. Knee sprains and shoulder sprains are common among those who participate in football, basketball, soccer, rugby, wrestling, gymnastics, and skiing. Foot sprains are a danger for ballet dancers, snowboarders, windsurfers, equestrians, and competitive divers. Wrist sprains are common in skiing, football, basketball, baseball, roller hockey, boxing, basketball, volleyball, and weightlifting. The specific joint that tends to be sprained during a particular sport is usually related to the kinds of joint movements that the sport requires, or to the types of impact or collision that can happen. For example, many knee sprains in football players are caused by the extreme knee stress of cutting moves and sharp turns. Others are caused by the direct impact of tackles.
Off the playing field, sprains often occur because of high-impact accidents — for example, striking the knee on the dashboard during a car crash or slipping on a patch of ice and landing on a wrist or shoulder. Sprains are also common in the workplace.
Symptoms of a sprain
In general, sprains cause pain and swelling in the injured joint, along with some local joint tenderness. In moderate or severe sprains, there can also be deformity (a change in the joint's normal contour) and a noticeable change in the joint's function. This change in function can include a feeling that the joint is unstable or unreliable (for example, the knee feels as if it will buckle or give out); a feeling that the joint is too loose or that the bones are not aligned in their normal positions; or a change in the joint's normal range of motion.
Other symptoms depend on the joint involved and the ligament that has been injured. For example, a sprain of the knee's anterior cruciate ligament can sideline an athlete immediately because of severe pain, swelling, and a feeling that the knee will give out. A sprain of the knee's posterior cruciate ligament, however, may cause only mild swelling that does not stop the athlete from continuing play.
Diagnosing a sprain
Information about exactly how you injured your joint is an important part of your evaluation. This information includes:
- the type of movement that caused your injury
- how long it took for pain and swelling to appear
- the ability to use the joint since the injury (for example, ability to bear weight)
- changes in joint function, especially joint instability or a decrease in the joint's normal range of motion.
Also, as part of your basic evaluation, your health care professional will ask about your occupation, your routine recreational and sports activities, and any history of previous injuries to the injured joint. This will help to determine your risk of injuring the area again.
If you were injured during an athletic activity, your doctor may ask if there was an eyewitness who can provide details about your injury.
Because most joints come in pairs, your health care professional will compare your injured joint with your uninjured one. During the examination, your doctor will check your injured joint for swelling, deformity, tenderness, bruising, and skin injuries. If pain and swelling permit it, he or she also will evaluate your joint's range of motion and perform special maneuvers to check for joint instability and abnormal looseness. If your injury is severe, your doctor may recommend diagnostic tests, including:
- x-rays to check for a fracture or other bone damage
- a magnetic resonance imaging (MRI) or computed tomography (CT) scan to look for torn cartilage, a torn ligament, or another cause of pain
- arthroscopy, a minor operation, to look inside the joint and examine it directly.
Once your physical examination and any recommended testing are complete, your doctor may gauge the severity of your sprain according to a traditional grading system.
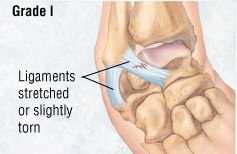
- Grade I (mild) — A mild injury causing only stretching or microscopic tears in a ligament. Although tiny tears can stretch the ligament, they do not significantly affect the stability of the injured joint.
|
|
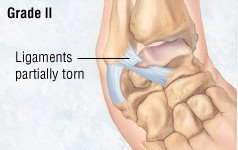
- Grade II (moderate) — The injured ligament is partially torn, and there is some mild to moderate joint instability.
|
|
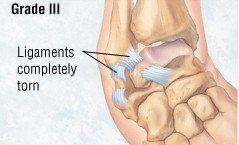
- Grade III (severe) — The ligament is either torn completely or avulsed (pulled away from the place where it attaches to bone), and there is significant joint instability.
|
|
Expected duration of a sprain
How long a sprain lasts depends on many factors, including the location and severity of your sprain, how closely you follow your rehabilitation program, and your lifestyle (athletic or nonathletic). For example, symptoms of a Grade I wrist sprain may improve within just two or three days, while a Grade I shoulder sprain may take about two weeks. In the knee, a Grade I or II sprain of one of the collateral ligaments probably will heal within two to four weeks, but a severe (Grade III) sprain of the anterior cruciate ligament may take four to 12 months.
In general, rehabilitation programs are usually longest for athletes, especially athletes who play sports in which there is a high risk of injuring the sprained joint again.
Preventing a sprain
The best way to prevent sprains is to avoid accidents and injuries. To prevent sports-related sprains, you should:
- Warm up and stretch before you participate in athletic activities.
- Exercise to strengthen the muscles around your joints.
- Avoid sudden increases in the intensity of your training program. Never push yourself too hard, too fast. Increase intensity gradually.
- Wear comfortable, supportive shoes that fit your feet and your sport.
- Wear protective equipment. For example, snowboarders and inline skaters can protect themselves from wrist sprains by using wrist guards or snug-fitting plastic wrist splints.
- If possible, choose sports equipment that helps to limit your risk of sprains. For example, skiers may be able to decrease the risk of wrist sprains by using ski poles that have a low-profile grip with finger grooves. Skiers also should grip their ski poles without using straps and discard their poles during a fall.
Treating a sprain
If you have a Grade I or Grade II sprain, your health care professional probably will recommend that you follow the RICE rule:
- Rest the joint.
- Ice the injured area soon after the injury to reduce swelling.
- Compress the swelling with an elastic bandage.
- Elevate the injured joint.
|
|
Depending on the location of your sprain, your health care professional also may suggest that you wear a sling or a brace to temporarily reduce stress on the injured area. In addition, you can take a nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen (Advil, Motrin, and others) to ease pain and relieve swelling. As your joint pain gradually subsides, your doctor may prescribe a rehabilitation program to strengthen the muscles around your injured joint. As nearby muscles get stronger, the joint becomes more stable, reducing the risk of injuring it again.
If you have a Grade III sprain, several different treatments can be used, depending on which ligament has been torn. Some torn ligaments can be repaired surgically with stitches, whereas others must be replaced surgically using either an autograft (a piece of your own tissue) or an allograft (a piece of donor tissue). Still others are treated with rehabilitation and temporary casting or bracing.
When to call a professional
If you injure a joint, call your doctor immediately if the joint:
- becomes very painful or swollen
- has lost its normal contours, looks deformed or has misaligned bones
- feels unstable or loose
- is unable to carry its normal load — for example, if your leg cannot bear weight
- has a change in its normal range of motion — for example, you can't stretch out your knee or you can't bend your wrist.
Prognosis
The outlook is generally good for most Grade I or Grade II sprains. Overall, 80% to 90% of patients recover fully, depending on the specific ligament that was injured. Although most Grade III sprains also heal well, there may be a greater risk of troublesome long-term symptoms, especially chronic joint pain, persistent swelling, or some limitation of joint function. Without surgery, Grade III sprains may continue to cause symptoms of instability.
Also, as a long-term complication, some patients with sprains eventually develop symptoms of osteoarthritis in the injured joint. These symptoms may not start until 10 to 15 years after the initial injury.
Additional info
National Institute of Arthritis and Musculoskeletal and Skin Diseases
https://www.niams.nih.gov/
American Academy of Orthopaedic Surgeons (AAOS)
https://orthoinfo.aaos.org/
National Athletic Trainers' Association
https://www.nata.org/
American Physical Therapy Association
https://www.apta.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.