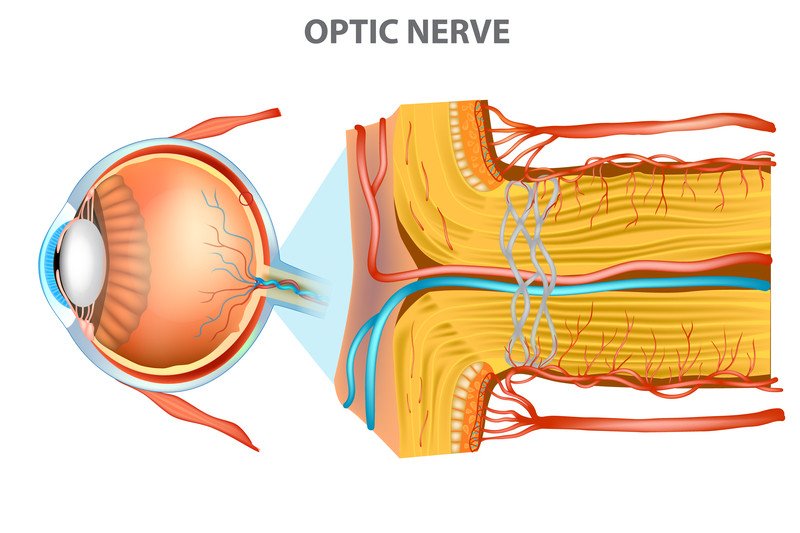
Optic nerve swelling (papilledema)
Medically reviewed by Drugs.com. Last updated on Jun 12, 2025.
What is Optic nerve swelling (papilledema)?

Papilledema is the swelling of the optic nerve as it enters the back of the eye due to raised intracranial pressure. Fluid surrounding the brain is constantly produced and reabsorbed, maintaining just enough intracranial pressure to help protect the brain if there is blunt head trauma.
When you have a headache or unexplained nausea and vomiting, your doctor will look into your eye with an ophthalmoscope. This handheld instrument shines a bright light into your eye. Changes in the appearance of the optic nerve and the blood vessels that pass through it can be seen through the ophthalmoscope and might be related to the source of your symptoms.
The anatomy of the optic nerve makes it a sensitive marker for problems inside the brain. This nerve connects the back of each eyeball and its retina to the brain. In its short span between the brain and the eye, the optic nerve's whole surface is bathed in cerebral spinal fluid. This fluid protects the nerve from sudden movement.
However, even slight increases in the pressure of this fluid, from swelling of the brain, can compress the optic nerve around its whole circumference in a "choking" manner. When this nerve is exposed to high pressure, or when it develops inflammation on its own, it can bulge into the back wall of the eyeball, causing papilledema.
|
|
Doctors have commonly used the term to describe the appearance independent of the underlying cause. The term papilledema ideally should be reserved for swelling of the nerve head when the swelling is caused by elevated intracranial pressure. Other conditions can have a similar appearance to papilledema caused by high intracranial pressure.
Some important causes of increased pressure from cerebral spinal fluid and papilledema are brain tumors and brain infections, such as a brain abscess, meningitis, or encephalitis. A significant proportion of people who are diagnosed with brain tumors have some evidence of papilledema. A pressure increase resulting from bleeding or from very high blood pressure also can cause papilledema.
One condition can cause increased pressure in the cerebral spinal fluid without associated swelling of the brain or ventricles. This condition, called idiopathic intracranial hypertension or pseudotumor cerebri, is caused when the body makes too much spinal fluid. It is more common in women who are obese and of childbearing age. The condition seems to be triggered at times that the body is adjusting to hormone changes, such as pregnancy, the start of birth control pills, the first menstrual period, or menopause.
Symptoms
Symptoms related to papilledema caused by increased pressure include headache and nausea with vomiting and a machinery-like sound. Twenty-five percent of people with advanced severe papilledema also will develop some visual symptoms. Typically, the visual changes are recurring brief episodes lasting less than 30 seconds in which the vision turns gray or black, sometimes described as if a veil has fallen over the eyes. The symptoms usually affect both eyes at once.
Visual blackouts often are triggered by a change in position, such as by standing up very suddenly, or they may be triggered by coughing or straining in the chest or abdomen. Occasionally, people with papilledema can have an experience of flashing lights, often seen in an arc shape. Other visual changes occur over time, including a smaller field of vision with a larger blind spot and, ultimately, blindness, if successful treatment is not given.
Diagnosis
The front end of the optic nerve is visible at the back of the eye when your doctor or an eye specialist looks through the pupil with an ophthalmoscope. The round, front end is just over 1.5 millimeters in size. Normally, the end of the nerve, called the optic disc, has a crisp outline and is indented slightly. If the optic disc appears elevated and has a blurred outside edge, your doctor can diagnose papilledema. The pressure within the nerve can cause the draining veins in your eye to become congested.
Also, very tiny pulsations that normally are seen in the eye's veins tend to disappear. When papilledema is severe, small red spots from local bleeding or spotty color changes on the retina from accumulated debris or from damaged retina cells may be seen. Papilledema due to raised intracranial pressure is almost always bilateral.
The physical exam also will include a check of your field of vision. Papilledema causes each eye to have a wider blind spot near the nose, and it narrows the peripheral (edge) vision. To check your visual field, your doctor may compare your vision abilities to his or her own by sitting across from you and moving fingers in and out of view. Visual fields can be tested more formally by an ophthalmologist using vision grids.
Findings that show you have papilledema indicate a very abnormal problem that usually needs immediate medical attention. The concern is less about vision loss. Papilledema from increased brain pressure usually does not damage the optic nerve, except when it is high pressure over a long time. The concern is damage to the brain; the brain swelling can sometimes be life-threatening. Brain imaging should be performed urgently either with computed tomography (CT) or magnetic resonance imaging (MRI).
If there is no abnormality on the brain scan, most patients will need to have a lumbar puncture (spinal tap) done so that the pressure of the cerebral spinal fluid can be measured. Idiopathic intracranial hypertension (pseudotumor cerebri) is a common cause of papilledema when the brain scan is normal.
Expected duration
After the cause of papilledema is identified and treated, and any pressure increase in the spinal fluid has returned to normal, optic disk swelling gradually will go away over six to eight weeks. When a pressure increase requires longer treatment, as in idiopathic intracranial hypertension, symptoms can take longer to clear.
Prevention
Many of the causes of papilledema cannot be prevented. Steps to help prevent some causes of papilledema include:
- Follow your doctor's instructions to control high blood pressure, and never skip doses of blood pressure medicine unless your doctor instructs you to do so.
- Stay physically fit and avoid obesity by exercising and maintaining a low-fat diet.
Treatment
The choice of treatment of papilledema depends upon its cause.
If a brain tumor is diagnosed, a biopsy (by surgery) may be required as the first step. Treatment of a brain tumor depends on the location and size. Treatment might include surgery, radiation, chemotherapy, biologic therapy, or a combination of these. High blood pressure should be managed as an emergency in the hospital if it results in papilledema.
Idiopathic intracranial hypertension can be treated with repeated spinal taps to remove excess spinal fluid, or with a medication called acetazolamide (Diamox and other brand names). This medicine causes the body to make less cerebral spinal fluid and returns the central nervous system's pressure to normal. Weight loss is encouraged and is helpful. A few patients will require surgery to help extra spinal fluid drain if they do not do well with initial treatment. Because idiopathic intracranial hypertension is often a long-lasting condition that has the potential to damage vision, monitoring by an ophthalmologist is an important part of the treatment.
When to call a professional
If you have a headache that is accompanied by nausea and vomiting, and you do not know the cause, it is important for you to contact your doctor immediately. It is particularly important to have these symptoms evaluated if you have a fever, high blood pressure, or if you have recently started taking birth control pills or are pregnant.
Prognosis
You may have mild papilledema for months or years and still not lose significant vision. However, once you begin to lose vision, it can become permanent within days or weeks, and requires urgent treatment.
Additional info
National Institute of Neurological Disorders and Stroke
https://www.ninds.nih.gov/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.