Double vision (diplopia)
Medically reviewed by Drugs.com. Last updated on Sep 28, 2023.
What is Double vision (diplopia)?

Double vision, also called diplopia, causes a person to see two images of a single object. There are two types of double vision: monocular and binocular.
Monocular diplopia is double vision in only one eye. The double vision continues even when the other eye is covered. The doubling does not go away when you look in different directions. Monocular diplopia can be caused by:
- Astigmatism — This is an abnormal curvature of the front surface of the cornea.
- A dislocated lens — The ligaments that hold the lens in place are broken, and the lens moves out of place or wiggles. This can be caused by trauma to the eye or a condition known as Marfan's syndrome.
- Pterygium — This is a thickening of the conjunctiva, the thin mucous membrane that lines the inner surface of the eyelids and the whites of the eyes. The thickening extends on the cornea, the clear part of the surface of the eye.
- Keratoconus — The cornea gradually becomes thin and cone-shaped.
- Cataracts — The lens gradually becomes less transparent. Risk factors include being older than 65, having eye trauma or long-term diabetes, smoking, using steroid medications or having radiation treatments.
- A mass or swelling in the eyelid — This condition can press on the front of the eye.
- Dry eye — Your eyes do not produce enough tears.
- Some retinal problems — Double vision can happen when the surface of the retina is not perfectly smooth, which can have a variety of causes.
Binocular diplopia is double vision related to a misalignment of the eyes. The double vision stops if either eye is covered. Any problem that affects one or more of the muscles around the eyeball that control the direction of the gaze can cause binocular diplopia. These are called extraocular muscles. Such problems include:
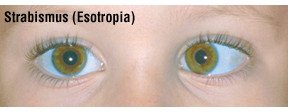
- Strabismus — This is a childhood misalignment of the eyes that affects about 4% of children younger than age 6.
|
|
- Damage to nerves controlling the extraocular muscles — Nerves can be injured by brain damage caused by infection, multiple sclerosis, stroke, head trauma or a brain tumor, especially a tumor located at the lower back portion of the brain. A tumor growing inside the eye socket or trauma to the eye socket can damage a nerve anywhere along its route to the eye muscles.
- Diabetes — This disease can lead to problems with the nerves that control eye muscle movements. Sometimes this can happen before the person is aware that he or she has diabetes.
- Myasthenia gravis — This is a neuromuscular illness that causes the body's muscles to tire easily and become weak. It occurs because the body's immune system mistakenly attacks the places where nerves transmit impulses to muscles, telling the muscles to contract.
- Graves' disease — This is the most common cause of an overactive thyroid (hyperthyroidism). Some people with Graves' disease develop double vision due to swelling and thickening of the muscles that move the eyes within the eye socket.
- Trauma to the eye muscles — The muscles of the eye socket can be injured by facial trauma, especially by a fracture of the thin bones of the eye socket.
Symptoms
The only symptom is seeing two images of a single object.
Diagnosis
The first step is to determine whether your double vision is monocular or binocular. To do this, your doctor will ask you to cover one eye and then the other. If you have monocular diplopia, your doctor will evaluate you for conditions, such as cataracts, that could be causing the problem. You will then need to see an eye specialist (an ophthalmologist). If the problem is binocular and there has been no facial trauma, then your doctor will want to know if you have diabetes, Graves' disease or neurological disorders.
In diagnosing binocular diplopia, your doctor has to determine which eye muscles are affected. To do this, you will be asked to look at the doctor's finger as he moves it up, down, left and right. This lets the doctor see how far your eye can move in each direction. Your doctor also will cover one eye and then the other, while you focus on a target. If the doctor sees your eyes shift as the eye cover is moved, it means your eyes are not aligned properly. Prisms may be placed over your eye to shift the image, and the test is repeated. The prisms allow the doctor to measure the amount or degree of your double vision when you look in different directions. This helps to diagnose the problem and monitor the problem over time. Your doctor will use the results of this exam, together with your medical history and additional symptoms, to determine if you need more tests.
For example, if your doctor suspects that you have hyperthyroidism, then you will need blood tests to measure thyroid hormone levels. If your doctor suspects that something is affecting the nerves to your eye muscles, you may need a magnetic resonance imaging (MRI) or computed tomography (CT) scan of your head to check for signs of trauma, bleeding, tumor or blood vessel malformations in the brain.
In most cases, double vision is easy to pinpoint in adults, because they can describe what they are seeing. Symptoms are tougher to pinpoint in children, who may not be able to explain what is wrong. Parents may notice that the child is squinting, covering one eye with a hand, tilting or turning the head abnormally, or looking sideways.
Expected duration
How long your double vision lasts depends on what is causing it. For example, cataracts and pterygium may become worse over time, but both can be corrected immediately with surgery. In people whose double vision is caused by diabetes, the nerve often regrows after several months. When this happens, double vision gradually disappears. Children with double vision caused by strabismus can improve with treatment.
Prevention
Some causes of double vision can be prevented. To help prevent double vision related to head trauma, wear a seat belt with a shoulder harness while driving, and wear protective goggles and headgear during sporting activities and at work, if your work carries a high risk of eye injury. People with diabetes can decrease their chance of nerve damage, which can lead to double vision, by controlling blood sugar. There is no way to prevent age-related cataracts or some other forms of double vision.
Treatment
Treating double vision depends on its cause. For example, people with astigmatism that causes double vision can wear special contact lenses. Sometimes, simply updating your prescription eyeglasses takes care of the problem. Surgery is used to treat cataracts and pterygium, and surgery on the eye muscles can treat certain types of double vision. Often, adjustable stitches are used so that the position of the eyes can be fine-tuned a few hours after the surgery. That way, the patient is alert for the adjustment and can report whether the double vision is gone. Prisms also may be used in the glasses to fine-tune the surgery by moving the image seen with one eye to coincide with the other eye.
For children with strabismus, treatment includes wearing prescription eyeglasses, prism vision therapy to train the eyes to align properly, or surgery. Double vision caused by a medical or neurological disease may improve by treating the disease. Eye specialists may consider other strategies to help improve the eye movements. Injections of botulinum toxin (Botox) can weaken strong eye muscles opposite the weakened one to help balance vision.
When to call a professional
Call your doctor right away if you have a dramatic change in vision or sudden difficulty seeing clearly.
Children should have their first eye exam before they are 6 months old, with a follow-up exam at age 3. Adults older than 40 years of age should schedule periodic eye examinations, even if they have no noticeable vision problems.
Prognosis
The outlook for double vision depends on its cause. For example, surgery improves the vision of more than 90% of patients with cataracts. Although surgery also can remove a pterygium, the abnormal growth can come back and eventually become larger than the original.
For most children with strabismus, the prognosis is excellent if the condition is detected and treated early.
Additional info
National Eye Institute
https://www.nei.nih.gov/
American Optometric Association
https//www.aoa.org/
American Academy of Ophthalmology
https://www.aao.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.