Anal disorders
Medically reviewed by Drugs.com. Last updated on Jul 18, 2025.
What are anal disorders?

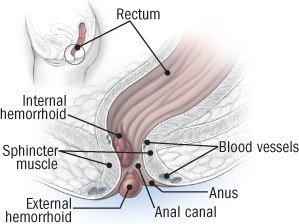
The anus is that part of the intestinal tract that passes through the muscular canal of the pelvis and anal sphincters. It is the final orifice through which stool passes out of the body. In adults, the anus is 4 to 5 centimeters long. The lower half of the anal canal has sensitive nerve endings. There are blood vessels under the lining, and in its mid portion there are numerous tiny, anal glands.
|
|
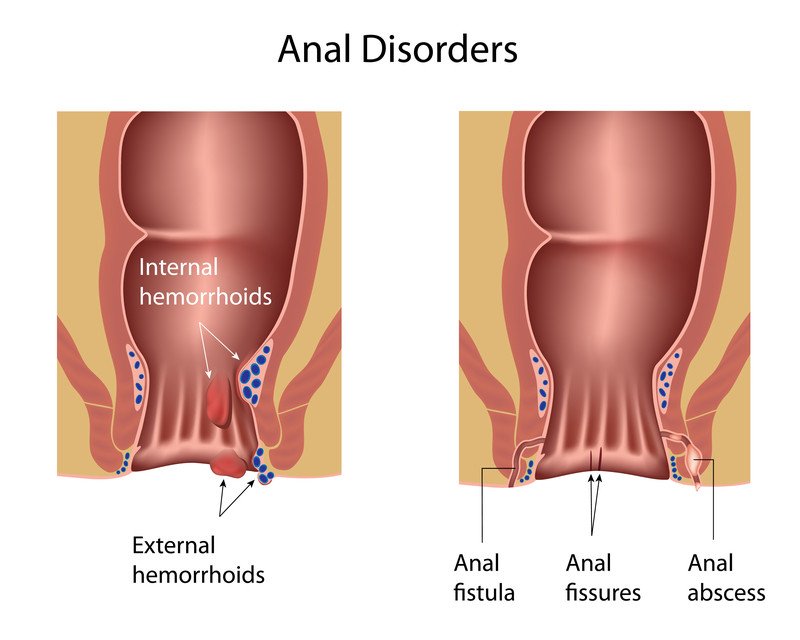
This article describes four disorders that cause anal pain and irritation:
- Anal fissure - An anal fissure, also called an anorectal fissure, is a linear split or tear in the lining ("anoderm") of the lower anal canal. Most anal fissures happen when a large, hard stool overstretches the anal opening and tears the delicate anoderm. Less often, anal fissures develop because of prolonged diarrhea, inflammatory bowel disease or sexually transmitted diseases involving the anorectal area. Acute (short-term) anal fissures are usually superficial and shallow, but chronic (long-term) anal fissures may extend deeper through the anoderm to expose the surface of underlying muscle.
- Anal abscess - An anal abscess is a swollen, painful collection of pus near the anus. Most anal abscesses are not related to other health problems and arise spontaneously, for reasons that are unclear. They originate in a tiny anal gland, which enlarges to create a site of infection under the skin. In the United States, more than half of all anal abscesses occur in young adults between the ages of 20 and 40, and men are affected more often than women. Most anal abscesses are located near the opening of the anus but rarely can occur deeper or higher in the anal canal, closer to the lower colon or pelvic organs.
- Anal fistula - An anal fistula is an abnormal narrow tunnel-like passageway, which is the remnant of an old anal abscess after it has drained. It connects the mid portion of the anal canal (at the anal gland) to the surface of the skin. After an anal abscess has drained (either spontaneously or when lanced by a physician), an anal fistula will develop at least half of the time. Sometimes the opening of the fistula at the skin surface constantly discharges pus or bloody fluid. In other cases, the opening of the fistula closes temporarily, causing the old anal abscess to flare up again as a painful pocket of pus.
- Hemorrhoids - Hemorrhoids do not ordinarily cause pain. Nevertheless, sometime the blood vessels in a small hemorrhoid at the edge of the anal orifice can clot off ("thrombosis"). This may be triggered by a period of constipation of diarrhea. When thrombosis occurs, the external hemorrhoid becomes swollen, hard, and painful, sometimes with bloody discharge.
|
|
Symptoms of anal disorders
Although all four anal disorders cause some type of anal discomfort or pain, other symptoms vary, depending on the specific anal problem.
For anal fissure, symptoms may include:
- pain in the anal area, often described as sharp, searing or burning, and usually triggered by a bowel movement
- mild rectal bleeding, typically a small amount of bright red blood with a bowel movement or on the toilet paper.
For anal abscess, symptoms include:
- a firm, tender mass or swelling in or around the anal area, which may become large
- occasionally fever, chills and a generally sick feeling.
For an anal fistula, signs and symptoms may include:
- mild pain around the anus, centered in an area where an old anal abscess has either drained spontaneously, or has been opened surgically by a doctor.
- persistent drainage of blood, pus or foul-smelling mucus from the anal area.
- symptoms of a recurrent anal abscess (see above), which may develop if the external opening of the fistula becomes clogged and the old abscess reactivates.
For thrombosis of an external hemorrhoid, the signs and symptoms include:
- a firm and usually quite painful swelling at the anal orifice
- occasionally bloody discharge, if the surface of the hemorrhoid breaks down.
Diagnosing anal disorders
Once you have described your symptoms, your doctor will ask questions about your medical history and lifestyle that will help in evaluating your anal problem. Depending on your symptoms, the doctor may ask about:
- your bowel habits, especially any history of constipation
- your medical history, including any history of bleeding disorders, episodes of rectal bleeding, inflammatory bowel disease, sexually transmitted diseases or radiation treatment for cancer
- your use of prescription or nonprescription medications that may increase the risk of bleeding
- whether you practice anal intercourse or have any history of anal trauma.
Next, your doctor will perform a physical examination of your abdomen, followed by an external examination of your anal area and a digital (finger) rectal examination. Usually your doctor will also perform anoscopy (insertion of a tube-like instrument into the anus to look inside the anal canal) and sigmoidoscopy (a short telescope to examine the rectum and lower colon).
Expected duration of anal disorders
How long anal disorders last varies:
- Anal fissure — Painful anal fissures can be a recurrent problem in people who suffer from repeated episodes of constipation. Fortunately, superficial fissures usually heal quickly with medical treatment, and most symptoms disappear within a few days to a couple of weeks.
- Anal abscess — An anal abscess sometimes drains on its own, although it is always safer for a doctor to evaluate the problem. If the abscess does not drain on its own, the doctor may incise and drain the abscess. After an abscess is drained, the pain is usually immediately better. An anal abscess often turns into an anal fistula even with appropriate treatment.
- Anal fistula — Without treatment, an anal fistula may continue to ooze blood or pus for prolonged periods.
- Thrombosed external hemorrhoid — Usually the body will slowly reabsorb the clot in such a hemorrhoid, and the pain and swelling will slowly go away over a period of days to a couple of weeks. However, when it is very painful, your doctor can remove the clot.
Preventing anal disorders
You may be able to prevent anal fissures by preventing constipation. To do this, soften your stool by gradually adding more fiber to your diet, and by drinking 6 to 8 glasses of water daily. Commercially available fiber supplement powders work well.
Although it is not always possible to prevent other types of anal disorders, you may be able to decrease your risk for these illnesses by:
- using gentle techniques to clean the anal area
- keeping the anal area dry by changing underwear frequently and using powder to absorb moisture
- always using a condom if you practice anal intercourse
- never inserting any foreign object into the rectum.
Treating anal disorders
A doctor must diagnose the four anal disorders described here. Once the diagnosis is made, your treatment may or may not involve surgery, depending on the specific disorder. If surgery is necessary, your doctor will use whatever type of anesthesia is appropriate to help prevent you from feeling pain in this very sensitive area.
- Anal fissure - For an acute fissure, your doctor may recommend that you follow the suggestions for relieving constipation that are described in the Prevention section above. He or she also may tell you to apply a medicated ointment to the fissure, and to soak the anal area in warm water for 10 to 15 minutes several times a day ("sitz bath"). For chronic fissures, surgery can correct the problem in more than 90% of cases.
- Anal abscess - An anal abscess must be opened or lanced by a doctor to drain the pus. This procedure is called incision and drainage, or I&D. This usually can be done as an outpatient procedure, especially if you are young and generally healthy, and your abscess is close to the anal opening.
- Anal fistula - Surgery to unroof the fistula track ("fistulotomy"), is the most effective therapy. Your doctor opens the infected canal and scrapes away any remnants of the old anal abscess. The wound is left open to heal from the bottom up. If the fistula is associated with Crohn's disease, treatment is directed toward the Crohn's disease with anti-inflammatory medications combined with an antibiotic.
- Thrombosed external hemorrhoid - Usually this will slowly disappear on its own. The process can be hastened by taking a fiber supplement to soften the stool, as well as by taking frequent warm water soaks ("sitz baths"). If the hemorrhoid is unusually painful, the doctor may carry a minor surgical procedure under local anesthesia to remove the clotted hemorrhoid.
When to call a professional
Call your doctor promptly whenever you have rectal bleeding or any bloody discharge from the anus. Even if you have been treated for a bleeding fissure in the past, it is always safer for your doctor to determine the best course of action. This is especially true if you are over age 40, when there is an increase in the risk of rectal bleeding from colorectal cancer and other serious digestive diseases.
Also, call your doctor if you have:
- severe pain in the anal area
- a tender mass or swelling near the anus, with or without a fever
- pus or a foul-smelling discharge from the anus
- discomfort or tightness in the anal area that interferes with bowel movements.
Prognosis
In most cases, the prognosis is excellent. Almost all acute fissures heal quickly with conservative treatment, and almost all fistulas and chronic fissures can be corrected with surgery. Appropriate treatment of anal strictures will allow stool to pass easily and comfortably.
Most anal abscesses heal after being drained by a doctor. Some develop into anal fistulas. If a fistula does complicate the healing of an abscess, a fistulotomy will totally eliminate both the fistula and any remaining abscess in most patients.
Additional info
National Institute of Diabetes & Digestive & Kidney Disorders
Office of Communications and Public Liaison
https://www.niddk.nih.gov/
American College of Gastroenterology (ACG)
https://gi.org/
American Gastroenterological Association
https://www.gastro.org/
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.