Vision Problems in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about vision problems in children:
Your child may be born with vision problems or develop them over time. Most vision problems are diagnosed during routine eye exams. Early diagnosis and treatment are important to prevent permanent damage.
Signs and symptoms of vision problems:
- Difficulty following an object with his or her eyes
- Blinking or rubbing his or her eyes a lot
- Crossed eyes or one eye pointing the wrong way
- Watery, red eyes, or pain when he or she looks at light
- A white pupil
- Holding things close to his or her eyes when he or she looks at them
- Shutting or covering up one eye when he or she tries to see something
- Squinting or frowning while he or she looks at objects
Seek immediate care if:
- Your child gets chemicals in his eye.
- Your child has a foreign object in his eye.
- Your child's eye is bleeding or looks different than usual.
- Your child has a sudden change in his vision.
- Your child's contact gets stuck in his eye.
Call your child's ophthalmologist or doctor if:
- Your child gets hit in the eye with an object.
- Your child has eye pain or sensitivity to light.
- Your child has red eyes and yellow or green eye drainage.
- Your child's eye is swollen or you see a bump on his or her eyelid.
- Your child feels like there is something in his or her eye.
- Your child says he or she has blurry vision or changes in his or her vision.
- You have questions or concerns about your child's condition or care.
What causes vision problems in children:
- Eye injuries or infections
- Medical conditions such as diabetes, cerebral palsy, or juvenile rheumatoid arthritis (JRA)
- Certain genes passed from a parent to his or her child
- Certain medicines, such as seizure medicine
Eye problems your child may be born with:
- Retinopathy of prematurity (ROP) is when abnormal blood vessels develop in your baby's retinas. The retina is the part of the eye that captures light and sends information to the brain. ROP happens in premature babies or low birth weight babies. ROP most often affects both eyes.
- A cataract is a clouding of the eye's lens. The lens is on the front of the eye. The lens helps focus light to create an image of what your child sees. Cataracts may affect one or both eyes.
- Glaucoma is eye damage that is caused by high pressure in your child's eye. Glaucoma may happen from poor development of his or her eye drainage system. It may be passed from a parent.
Vision problems your child may develop:
- Refractive errors means the eye does not bend light correctly, causing blurry vision. Your child may have trouble seeing things that are close to him or her, or things that are far away. Astigmatism is a problem with the curve of your child's eye surface. Your child may not have symptoms. He or she may have blurry vision or eye discomfort.
- Strabismus happens when the eyes do not move together at the same time. The eyes may face in different directions. One or both of your child's eyes may turn in, out, up, or down.
- Amblyopia is also called lazy eye. Your child may have poorer vision in the lazy eye. This may cause him or her to only use his or her good eye to see. The lazy eye may look normal, or it may turn in. Early treatment is important to prevent permanent vision loss in the eye.
- Ptosis is a condition that causes 1 or both of your child's eyelids to droop or sag. The eyelid may cover the eye and make it difficult for your child to see. Ptosis may cause amblyopia or astigmatism.
- Nystagmus is a condition that causes the eyes to make repetitive, uncontrolled movements. Your child's eyes may move side to side, up and down, or in a circle. He or she may have blurry vision or trouble with his or her balance and coordination. Nystagmus may be caused by problems in your child's brain. Nystagmus may improve with treatment of the brain problems.
Other eye problems that may affect your child's vision:
- Color blindness means your child's eyes are not able to see some or all colors. Color blindness may run in families or develop after an injury to the eyes, nerves, or brain. In children, color blindness happens more commonly in boys than in girls.
- Eye infections may be caused by different kinds of germs, such as bacteria, viruses, or fungi. A stye, or a bump on the edge of his or her eyelid, is a common eye infection. It is caused by an infected eyelash follicle. Conjunctivitis is another common eye infection. It is an infection of the white part of your child's eye.
- A chalazion is a small lump on your child's eyelid. It happens when an eye gland that makes oil becomes clogged.
- A blocked tear duct is a common problem in newborns. Your baby's pediatrician may show you how to massage and unblock the tear duct.
- Retinoblastoma is eye cancer that usually affects 1 eye.
How eye problems are diagnosed and treated:
All children aged 3 to 5 years should have at least 1 vision screening. Your child's healthcare provider will check the shape of your child's eyes and how they react to light. He or she may ask your child to read letters off of a chart or point to pictures. Tell his or her healthcare provider if you have noticed any problems with your child's eyes. If your child is born with vision problems or develops vision problems, he or she may need to see an ophthalmologist. An ophthalmologist is a doctor who diagnoses and treats eye and vision problems. Your child may need any of the following to treat an eye problem:
- Medicines such as antibiotic or antifungal eyedrops may be given to treat a bacterial or fungal infection. Eyedrops may also be used to treat glaucoma, strabismus, or amblyopia.
- Glasses can be worn by children of all ages. Glasses can help correct refractory errors or astigmatism. Choose lenses made of polycarbonate. This type of lens is less likely to scratch or break than other types. Choose plastic frames for children younger than 2 years. Attach a strap to both ends of your child's glasses. This will help keep your child's glasses in place.
- Contacts may be appropriate for your child by around age 10 years. Contacts may help correct some types of refractory errors. Your child may still need glasses while his or her contacts are out. Teach your child to wash his or her hands before he or she touches his or her eye or contacts. Your child should clean and change his or her contacts as directed. He or she should not swim or sleep with contacts in his or her eyes.
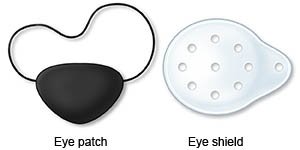
- An eye patch may be used to treat strabismus or amblyopia (lazy eye). Apply the patch to your child's healthy eye as directed. He or she may need a bandage placed over his or her eye or a cloth patch that fits over glasses. This will help improve vision in your child's weaker eye. Your child may need to wear the patch for 2 to 6 hours every day. Encourage your child to wear the patch. Distract him or her with toys and games to help him or her forget about the patch.
- Surgery may be used to correct problems such as a lazy eye or strabismus. Surgery may also be used to remove a cataract or relieve a plugged duct.
Help improve your child's vision health:
- Have your child's eyes checked every year. A child with a high risk for eye problems may need to have his or her eyes checked more often. This includes children who were born prematurely (early), or have a disease or condition that affects the brain. Early diagnosis and treatment of vision problems or eye diseases may prevent permanent damage.
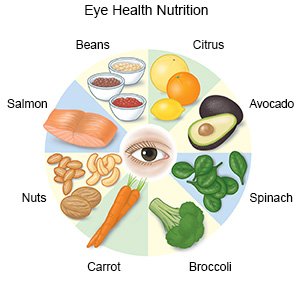
- Offer your child foods that contain eye-healthy nutrients. Eye-healthy nutrients include vitamin A, vitamin C, vitamin E, omega-3 fatty acids, lutein, and zeaxanthin. Examples of foods that contain these nutrients include spinach, peanuts, salmon, collard greens, avocados, squash, eggs, and blueberries. Ask your child's healthcare provider for a full list of foods that contain eye-healthy nutrients. Your child may also need to take a vitamin or supplement to help him or her get enough of these nutrients.
- Encourage your child to wear safety glasses, eye shields, or goggles. He or she should wear these any time he or she does an activity that increases his or her risk for an eye injury. Examples include swimming, racquetball, or lacrosse.
- Help your child prevent eye infections. An eye infection may be caused by bacteria, viruses, or fungi. Teach your child to wash his or her hands often. Wash your hands before and after you touch your child's eye. Encourage your child not to share eyedrops with anyone. Ask your child's healthcare provider how to put in eyedrops correctly.
- Encourage your child to wear sunglasses. Ultraviolet (UV) light from the sun can be harmful. Make sure sunglasses and ski goggles have UV protection.
- Limit your child's screen time. Screen time is the amount of television, computer, smart phone, and video game time your child has each day. It is important to limit screen time. This helps your child get enough sleep, physical activity, and social interaction each day. Your child's pediatrician can help you create a screen time plan. The daily limit is usually 1 hour for children 2 to 5 years. The daily limit is usually 2 hours for children 6 years or older. You can also set limits on the kinds of devices your child can use, and where he or she can use them. Keep the plan where your child and anyone who takes care of him or her can see it. Create a plan for each child in your family. You can also go to https://www.healthychildren.org/English/media/Pages/default.aspx#planview for more help creating a plan.
- Help protect your child's eyes during screen time. Too much time spent watching TV, playing video games, or staring at the computer can cause vision problems. Have your child take breaks from these activities every 20 minutes.
Follow up with your child's doctor or ophthalmologist as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
