Ventricular Septal Defect in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
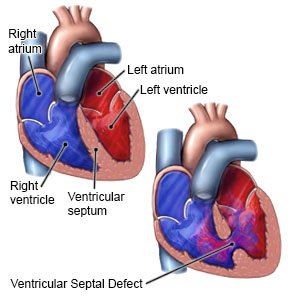
A ventricular septal defect (VSD) is a common kind of heart defect. An opening between the 2 lower chambers (ventricles) of your child's heart stays open. Normally, this closes before a baby is born. A VSD can cause blood to flow back into the right side of the heart instead of to the rest of your child's body. A VSD can lead to heart or lung problems or to low oxygen levels in your child's blood.
 |
WHILE YOU ARE HERE:
Informed consent
is a legal document that explains the tests, treatments, or procedures that your child may need. Informed consent means you understand what will be done and can make decisions about what you want. You give your permission when you sign the consent form. You can have someone sign this form for you if you are not able to sign it. You have the right to understand your child's medical care in words you know. Before you sign the consent form, understand the risks and benefits of what will be done to your child. Make sure all of your questions are answered.
Stay with your child for comfort and support
as often as possible while he or she is in the hospital. Ask another family member or someone close to the family to stay with your child when you cannot be there. Bring items from home that will comfort your child, such as a favorite blanket or toy.
Medicines:
- Antibiotics treat or prevent a bacterial infection.
- Diuretics help your child's body get rid of extra fluid. This can help your child breathe easier.
- Heart medicine helps your child's heart beat more strongly or more regularly.
Monitoring:
- A pulse oximeter is a small sensor that fits on your child's hand or foot. It measures the amount of oxygen in your child's blood.
- An EKG test records your child's heart rhythm and how fast his or her heart beats.
Tests:
- Blood tests may show infection, kidney function, or get information about your child's overall health. Blood tests may also be needed to check oxygen and carbon dioxide levels in your child's blood.
- A chest x-ray is taken to look at your child's heart and lungs.
- An echocardiogram is a type of ultrasound. Sound waves are used to show the structure and function of your child's heart.
- Cardiac catheterization is a procedure to look at your child's heart or measure pressure in his or her heart. Your child's healthcare provider will insert a catheter into a blood vessel in his or her arm, leg, or neck. Contrast liquid may be given to help healthcare providers see your child's heart and blood vessels better. Tell your child's healthcare provider if he or she has ever had an allergic reaction to contrast liquid.
Treatment:
- A nasogastric (NG) tube may be needed if your baby has trouble feeding. An NG tube is used to give liquid nutrition and medicine. The tube is put into your baby's nose and guided down into his or her stomach.
- Respiratory support includes oxygen, an endotracheal (ET) tube, or a ventilator. These can help your child breathe.
- Surgery may be needed to close the VSD in your child's heart. Surgery may be done as open heart surgery. It may also be done by inserting a catheter into a blood vessel in your child's groin. A small device will be inserted through the catheter to close the VSD.
RISKS:
A VSD may affect your child's health and quality of life depending on the severity of his or her symptoms. With or without treatment, your child may be at an increased risk for heart and lung problems.
CARE AGREEMENT:
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Ventricular Septal Defect
- Atorvastatin (Lipitor): Top 12 Drug Facts You Need to Know
- Do blood pressure drugs interact with alcohol?
- Side Effects of Weight Loss Drugs
Treatment options
Care guides
- Adult Congenital Heart Disease
- Congenital Heart Disease in Children
- Ventricular Septal Defect in Children
Medicine.com guides (external)
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
