Ventral Hernia
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a ventral hernia?
A ventral hernia is a bulge through a weak area in the abdominal wall. The abdominal wall is made of fat and muscle and holds the organs in place. The hernia may contain abdominal tissue, part of an organ (such as the intestine), or fluid.
What are the types of ventral hernias?
- An epigastric hernia occurs in the area between the sternum (chest bone) and the umbilicus (belly button).
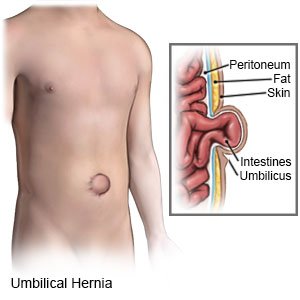
- An umbilical hernia occurs in the umbilicus.
- A spigelian hernia develops in the lower right or left part of the abdomen.
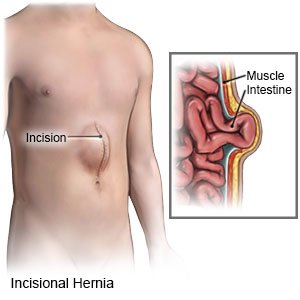
- An incisional hernia forms at a previous surgical incision site.
What causes a ventral hernia?
- Surgery or trauma to the abdomen, such as from a motor vehicle accident
- Age older than 60
- Intense exercise or lifting heavy objects often
- A higher body weight than recommended
- Pregnancy and childbirth
- A birth defect that prevents the abdominal wall from closing
- Chronic constipation, chronic cough, or straining to have bowel movements
- A chronic condition such as ascites
What are the signs and symptoms of a ventral hernia?
A ventral hernia may not cause any pain. Your hernia may disappear when you lie flat. You may have any of the following:
- A soft bulge or swelling in your abdomen or over your belly button
- A bulge that gets bigger when you cough, strain to have a bowel movement, or sit up
- Abdominal pain or constipation
- Fever, nausea, or vomiting
How is a ventral hernia diagnosed?
Your healthcare provider will ask about your symptoms and when they started. Tell your provider about other medical conditions you have and your activities. Your provider may examine your abdomen and feel for bumps. You may be asked to cough or bear down like you are having a bowel movement. This may help your provider see and feel your hernia better. You may need any of the following:
- Ultrasound, CT, or MRI pictures may show a blockage in the intestines or reduced blood flow to your organs. The imaging tests will also help your provider plan your treatment. You may be given contrast liquid to help the organs show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid. The MRI machine uses a powerful magnet. Do not enter the MRI room with anything metal. Metal can cause serious injury from the magnet. Tell a healthcare provider if you have any metal in or on your body.
- Blood and urine tests may be used to check your overall health, kidney function, or find signs of an infection.
How is a ventral hernia treated?
Surgery is often used to treat a ventral hernia. Your healthcare provider may also recommend any of the following:
- Medicines may be given to help reduce pain or swelling.
- Manual reduction of your hernia may be needed. Manual reduction means your provider uses his or her hands to put firm, steady pressure on your hernia. Pressure is applied until the hernia disappears inside your abdominal wall. You may need to wear a belt that holds the tissue in place.
- Surgery is usually done to place the hernia back inside the abdominal wall. You may need immediate surgery if the hernia stops blood flow to any of your organs. You may also need immediate surgery if your intestines or an organ get trapped inside the hernia.
How can I manage my symptoms and prevent another hernia?
- Do not lift heavy objects. Heavy lifting can increase pressure on your abdominal muscles and make your hernia bigger or cause another hernia. Ask your healthcare provider how much is safe for you to lift.
- Drink liquids as directed. Liquids may prevent constipation and straining during a bowel movement. Ask how much liquid to drink each day and which liquids are best for you.
- Eat foods high in fiber. Fiber may prevent constipation and straining during a bowel movement. Foods that contain fiber include fruits, vegetables, legumes, and whole grains.
.
- Do not put pressure on your hernia. Do not push on the hernia or place tape or a coin over it.
- Maintain a healthy weight. If your body weight is higher than recommended, weight loss may help relieve your symptoms. Your healthcare provider will tell you what a healthy weight is for you. Your provider can help you create a safe weight loss plan, if needed.
- Wear an abdominal belt, if needed. An abdominal belt can provide support, reduce discomfort, and prevent your hernia from worsening. An abdominal belt may be used to hold your hernia in the correct place after manual reduction. Ask your provider for instructions on how to apply and use an abdominal belt safely.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can weaken the abdominal wall. This may increase your risk for another hernia. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
When should I seek immediate care?
- Your hernia gets bigger, feels firm, or turns blue or purple.
- You have severe abdominal pain with nausea or vomiting.
- Your abdomen is larger than usual.
- You are unable to have a bowel movement or pass gas.
When should I call my doctor?
- You have a fever.
- You have nausea or are vomiting.
- You are constipated.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
