Varicose Veins
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What are varicose veins?
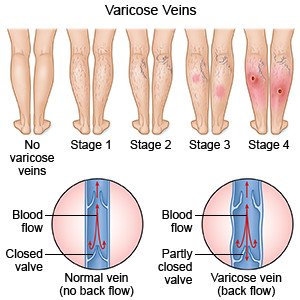
Varicose veins are veins that become large, twisted, and swollen. They are common on the back of the calves, knees, and thighs. Varicose veins are caused by valves in your veins that do not work properly. This causes blood to collect and increase pressure in the veins of your legs. The increased pressure causes your veins to stretch, get larger, swell, and twist.
 |
What increases my risk for varicose veins?
- Age 50 or older
- Being female
- Pregnancy
- A condition such as diabetes or high blood pressure
- A family history of varicose veins
- Excess body weight or obesity
- Sitting or standing for long periods of time
What are the signs and symptoms of varicose veins?
- Blue or purple bulging veins in your legs
- Pain, swelling, or muscle cramps in your legs
- Feeling of tiredness or heaviness in your legs
How are varicose veins diagnosed?
Your healthcare provider will examine your legs and ask about your medical history. You may need tests, such as a Doppler or duplex ultrasound scan. These scans show your veins and valves, and how your blood is flowing through them. The scans may also show if you have a blockage or blood clot in a vein.
How are varicose veins treated?
The goal of treatment is to decrease symptoms, improve appearance, and prevent further problems. Treatment will depend on which veins are affected and how severe your symptoms are. You may need a procedure to treat or remove your varicose veins. For example, your provider may inject a solution or use a laser to close the varicose veins. Surgery to remove long veins may also be done. Ask your provider for more information about procedures used to treat varicose veins.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage my symptoms?
- Maintain a healthy weight. Excess weight or obesity can make your varicose veins worse. Ask your provider what a healthy weight is for you. Ask your provider to help you create a weight loss plan, if needed.
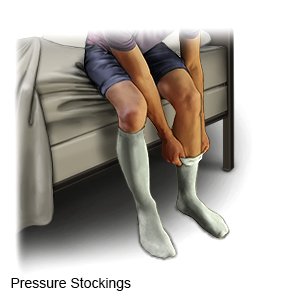
- Wear pressure stockings as directed. The stockings are tight and put pressure on your legs. This improves blood flow and helps prevent clots.
- Elevate your legs. Keep them above the level of your heart as often as you can. Prop your legs on pillows or blankets to keep them elevated comfortably. This will help blood flow back to your heart and decrease pain and swelling.

- Get regular exercise. Talk to your provider about the best exercise plan for you. Exercise can improve blood flow to your legs and feet.

How can I prevent my varicose veins from getting worse?
- Do not sit or stand for long periods of time, if possible. This can cause the blood to collect in your legs and make your symptoms worse. Bend or rotate your ankles several times every hour. Walk around for a few minutes every hour to get blood moving in your legs.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause lung damage. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Do not wear tight clothes or high-heeled shoes. Avoid clothes that are tight around your waist and knees. Wear clothes that fit well to help blood flow in your legs. Your symptoms may get worse if you wear high-heeled shoes.
- Do not cross your legs when you sit. This decreases blood flow to your feet and can make your symptoms worse. Make sure your feet can reach the chair's footrest or ground when you sit.
When should I seek immediate care?
- You have an injury that has broken your skin and caused your varicose veins to bleed.
- Your leg is swollen and hard.
- Your legs or feet are turning blue or black.
- Your leg feels warm, tender, and painful. It may look swollen and red.
- You have a wound on your leg that does not heal or is infected.
When should I call my doctor?
- You have pain in your leg that does not go away or gets worse.
- You have large bruising on your legs.
- You have a rash on your leg.
- Your symptoms keep you from doing your daily activities.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Varicose Veins
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
