Transcatheter Mitral Valve Repair
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about transcatheter mitral valve repair (TMVR):
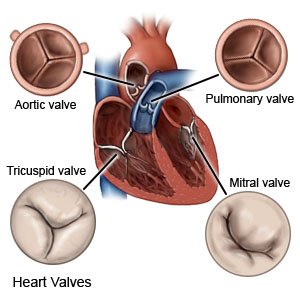
TMVR is a procedure to repair your mitral valve. The mitral valve normally opens and closes to let blood pass through the heart. If your mitral valve is damaged, blood may not flow as it should through your heart. TMVR is done if mitral valve replacement surgery is not safe for you. This procedure is also known as transcatheter edge-to-edge repair (TEER).
 |
How to prepare for your procedure:
- Your healthcare provider will tell you how to prepare. You may be told not to eat or drink anything after midnight on the day of your procedure. Arrange to have someone drive you home when you are discharged.
- Tell your provider about all medicines you currently take. Your provider will tell you if you need to stop any medicine for the surgery, and when to stop. Your provider will tell you which medicines to take or not take on the day of the procedure.
- Tell your provider about any allergies you have, including to anesthesia or medicines.
- You may need an echocardiogram (echo) before surgery. An echo is a type of ultrasound that uses sound waves to show the structure and function of your heart. This will help your provider plan your repair.
What will happen during your procedure:
- You will be given general anesthesia to keep you asleep and free from pain. Your healthcare provider will make an incision in your upper leg. A catheter will be put into a vein in your leg and guided to the left side of your heart.
- A clip or other repair device will be guided through the catheter to your mitral valve. Your provider will use fluoroscopy (continuous x-rays) and ultrasound imaging to help guide the device. The clip or other repair device will be placed so that it holds the middle of the mitral leaflets (flaps). This will reduce the amount of blood that flows back into your atrium. Your provider will do tests to make sure the clip or other repair device is in proper position..
- The catheter will then be removed and the incision in your leg will be closed.
What to expect after your procedure:
You will need to stay in the hospital for at least 1 day. Healthcare providers will monitor your heart functions.
Risks of a TMVR:
You may bleed more than expected. You may develop an infection. Damage to your vein or other blood vessels can occur. You may develop an abnormal or fast heartbeat. You may need medicine to correct your heartbeat. The clip or repair device may not reduce the back flow of blood enough. You may need different treatment.
Call your local emergency number (911 in the US) for any of the following:
- You have any of the following signs of a heart attack:
- Squeezing, pressure, or pain in your chest
- You may also have any of the following:
- Discomfort or pain in your back, neck, jaw, stomach, or arm
- Shortness of breath
- Nausea or vomiting
- Lightheadedness or a sudden cold sweat
- You have any of the following signs of a stroke:
- Numbness or drooping on one side of your face
- Weakness in an arm or leg
- Confusion or difficulty speaking
- Dizziness, a severe headache, or vision loss
- You feel lightheaded, short of breath, and have chest pain.
- You cough up blood.
- You have trouble breathing.
Seek care immediately if:
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.
- Your heart is beating faster or slower than usual.
- Your leg feels numb, cool, or looks pale.
- You feel weak or dizzy.
- Your incision site is red, swollen, or draining pus.
- Your incision site looks more bruised or there is new bruising near it.
Call your cardiologist or doctor if:
- Your symptoms return.
- You have new pain.
- You have a fever or chills.
- You have nausea or are vomiting.
- Your skin is itchy, swollen, or you have a rash.
- You have questions or concerns about your condition or care.
Medicines:
- Blood thinners help prevent blood clots. Clots can cause strokes, heart attacks, and death. Many types of blood thinners are available. Your healthcare provider will give you specific instructions for the type you are given. The following are general safety guidelines to follow while you are taking a blood thinner:
- Watch for bleeding and bruising. Watch for bleeding from your gums or nose. Watch for blood in your urine and bowel movements. Use a soft washcloth on your skin, and a soft toothbrush to brush your teeth. This can keep your skin and gums from bleeding. If you shave, use an electric shaver. Do not play contact sports.
- Tell your dentist and other healthcare providers that you take a blood thinner. Wear a bracelet or necklace that says you take this medicine.
- Do not start or stop any other medicines or supplements unless your healthcare provider tells you to. Many medicines and supplements cannot be used with blood thinners.
- Take your blood thinner exactly as prescribed by your healthcare provider. Do not skip a dose or take less than prescribed. Tell your provider right away if you forget to take your blood thinner, or if you take too much.
- Acetaminophen decreases pain and fever. It is available without a doctor's order. Ask how much to take and how often to take it. Follow directions. Read the labels of all other medicines you are using to see if they also contain acetaminophen, or ask your doctor or pharmacist. Acetaminophen can cause liver damage if not taken correctly.
Care for your incision site:
Ask your healthcare provider when your site can get wet. Carefully wash around the site with soap and water. Do not scrub the area. You can let soap and water gently run over your incision site. Gently pat dry the area and put on new, clean bandages as directed. Check your site every day for signs of infection. Do not put lotions or powders on the site. Do not take a bath or swim until your provider says it is okay. These activities can increase your risk for an infection.
Go to cardiac rehabilitation (rehab), if directed:
Cardiac rehab is a program supervised by healthcare providers. A cardiac rehab team includes doctors, nurses, exercise specialists, physical and occupational therapists, dietitians, and mental health providers. The providers will teach you ways to strengthen your heart and prevent future heart problems. The program can help you recover from your surgery and manage your heart condition. Cardiac rehab may last for several weeks or months, depending on your condition.
Activity:
Your healthcare provider will give you specific instructions. You may also get instructions if you go to cardiac rehab. The following is a general guideline to help reduce your risk for problems after your procedure:
- Do not lift objects heavier than 5 pounds.
- Do not do activities that cause you to hold your breath, grunt, or strain.
- Take short walks around the house several times a day. This will help prevent blood clots.
- Ask your provider what other activities are safe for you to do. Also ask when you can return to your normal activities.
Self-care:
- Carry your device identification card with you at all times. Inform healthcare providers that you have a mitral valve repair device. The device may be metal. Healthcare providers need to know before you have an MRI and other medical or dental treatment. You may need to take antibiotics before medical or dental treatments.
- Eat heart-healthy foods. You may need to eat foods that are low in salt, fat, or cholesterol. Healthy foods include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Ask your healthcare provider for more information about a heart healthy diet.

- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause heart and lung damage. Nicotine can also slow healing. Ask your provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your provider before you use these products.
- Do not drink alcohol. Ask your provider if it is okay for you to drink alcohol. Alcohol can increase your risk for high blood pressure, diabetes, and coronary artery disease.
- Maintain a healthy weight. Ask your provider what a healthy weight is for you. Extra weight can increase the stress on your heart. Your provider can help you create a weight loss plan, if needed.
- Be physically active as directed after you recover. Your provider can help you create an activity plan that is right for you. Physical activity will help keep your heart healthy.
Follow up with your cardiologist or doctor as directed:
You will need to have tests to make sure the device is working properly. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
