Tracheostomy Care for Children
Medically reviewed by Drugs.com. Last updated on Sep 23, 2025.
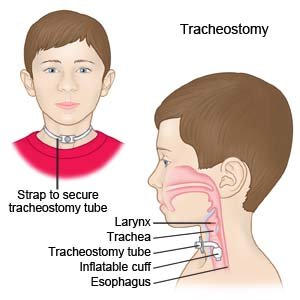
What is tracheostomy (trach) care?
Trach care is done to keep your child's trach tube clean. This helps prevent a clogged tube and decreases your child's risk for infection. Trach care includes suctioning and cleaning your child's skin and parts of the tube. Your child's healthcare provider will show you how to care for your child's tube, and what to do in an emergency.
 |
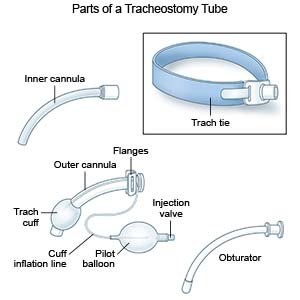
What are the parts of a trach tube?
Ask your child's healthcare provider the type, size, and length of your child's trach tube.
- An outer cannula is the tube that sits in your child's airway. There are different sizes of outer cannulas.
- Flanges are the curved wings on each side of the trach tube. The flanges can be connected to trach ties to hold the trach tube in place.
- Trach ties go around your child's neck and help keep the trach tube in place.
- A cuff fills with air and helps hold the tube in your child's airway. A thin tube that hangs from the outer cannula can be used to remove or insert air into the cuff. Your child's trach may not have a cuff.
- An inner cannula is a smaller tube that sits inside the outer cannula. The inner cannula can be removed for cleaning. There are different sizes of inner cannulas. Your child's trach tube may not have an inner cannula.
- An obturator is a small device used to insert a new trach tube.
- A speaking valve is a cap that fits over the opening of your child's trach tube. There are many different types of speaking valves. Ask your child's healthcare provider if your child can use a speaking valve and which one is right for him or her.
-
What supplies do I need for trach care?
Keep spare supplies with your child at all times . You may need to suction or change the tube if it gets clogged or needs to be replaced quickly.
- One trach tube the same size as the current tube and 1 trach tube that is 1 size smaller
- Obturator for each trach tube and an empty syringe
- One set of trach ties or a trach holder
- Portable suction machine with battery backup and tubing that connects to the suction machine
- Suction catheters
- Sterile saline and water-based lubricant
- Rescue breathing bag and mask
- Emergency phone numbers
How can I prevent infections in my child?
- Wash your hands. Always wash your hands before and after you care for your child's trach. Have your child wash his or her hands before and after he or she touches his or her trach.
- Clean your child's trach equipment as directed. Use clean or sterile trach care methods to clean your child's equipment.
- Use a trach cover over your child's trach as directed. Do not put a trach cover over your child's tube unless his or her healthcare provider says it is okay. This will protect your child's airway from dust and other foreign bodies.
- Clean the area around your child's trach as directed. The area around your child's trach is called the stoma.
- Keep your child's mouth clean. Saliva and mucus contain germs that cause infection if they enter your child's airway. Help your child brush his or her teeth twice a day. Suction your child's mouth as needed. Have your child use a mouth rinse as directed.
- Have your child take deep breaths and cough 10 times each hour. This will decrease your child's risk for a lung infection. Your child will not be able to do this if he or she is on a ventilator. Have your child take a deep breath and hold it for as long as he or she can. Tell your child to let the air out and then cough strongly. Deep breaths help open his or her airway.
How do I suction my child's trach tube?
Your child's healthcare provider will tell you when you need to suction his or her trach tube. Ask your child to take a deep breath and cough strongly before you suction his or her trach. This may be all that is needed to clear his or her airway.
- Watch for signs that your child needs his or her tube suctioned. Suction when your child cannot cough up his or her secretions. Your child may seem restless or scared, and his or her breathing may be louder or faster than usual. You may see mucus in your child's trach tube or coming from the sides of his or her trach tube. Your child's skin may look gray or blue.
- Do not suction your child's trach tube soon after he or she has eaten. He or she may cough or vomit if you suction too soon. Ask your child's healthcare provider how long you should wait to suction.
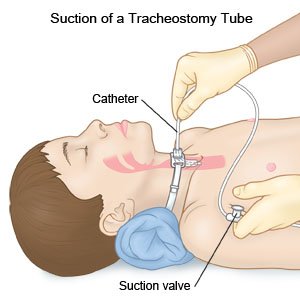
- Prepare your child's suction machine. Each suction machine has a pressure gauge. Your child's healthcare provider will tell you how much pressure to use when you suction his or her trach tube. Test the pressure before you suction. Do this by covering the suction valve on the catheter with your thumb.
- Suction your child's trach tube. Insert the catheter until it is just past the end of the tube. Your child's healthcare provider will show you how far to insert the catheter. The catheter may have measurements marked on it for you to follow. You can mark the catheter so you do not put it in too far. Cover the suction valve as you remove the catheter. It should take you less than 15 seconds to remove the suction catheter.
- Suction your child's trach tube a second time if needed. If your child uses oxygen, replace his or her oxygen for 30 seconds before you try to suction his or her trach again.
- Suction your child's stoma. Mucus and blood may leak from the sides of your child's tube. Gently suction this area with the suction catheter.
- Throw away the suction catheter or clean as directed. Disposable suction catheters should be thrown away. Reusable catheters can be cleaned and reused. To clean a reusable catheter, suction sterile water and air through the catheter as directed. Wipe the outside with alcohol or hydrogen peroxide as directed. Allow the catheter to air dry.
How do I care for my child's trach tube?
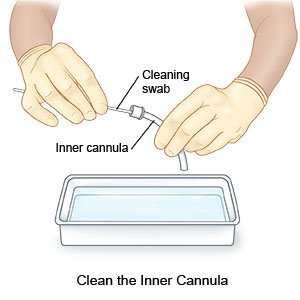
- Clean the inner cannula at least once every day. You do not need to do this if you child does not have an inner cannula.
- Wash your hands and put on gloves.
- Suction your child's trach.
- Remove the inner cannula. Clean the inside and outside of the cannula. Use hydrogen peroxide and a soft brush or pipe cleaner as directed. Make sure you remove all blood and dried mucus.
- Rinse the inner cannula with sterile saline and replace it into the outer cannula. It should snap into place.
- If you cannot clean the cannula well, throw it away and use a new inner cannula.
- Check the cuff pressure at least once each day. Your child's healthcare provider will show you how to check his or her cuff pressure. Ask your child's provider how much air should be in his or her cuff. You may need to add or remove air from your child's cuff. It is important that your child's cuff contains the correct amount of air. This will prevent breathing problems or damage to his or her airway.
- Keep water and other materials out of your child's trach tube. Do not let your child swim. Place a shower shield or trach cap over your child's trach while he or she bathes. This will prevent water from entering his or her airway. Do not use powders or sprays near your child's trach tube.
How do I care for my child's skin around his or her trach tube?
Clean your child's skin at least once every day or as directed. You may need to clean it more often if he or she coughs up a lot of thick mucus.
- Wash your hands and put on gloves. This will prevent infection.
- Suction the area around your child's stoma. This will help remove mucus.
- Clean your child's skin around the stoma. Use the following steps to clean the skin around his or her trach tube:
- You may be told to use soap and water or hydrogen peroxide to clean your child's skin. Mix hydrogen peroxide with an equal amount of sterile water. Pour this mixture onto clean gauze. The gauze should be damp but not soaked.
- Gently wipe around your child's stoma. Start closest to your child's stoma and move outward. Use a new gauze every time you wipe a new area of his or her skin. This will prevent infection. Dip clean cotton tips in the hydrogen peroxide mixture. Use the cotton tips to clean under the flanges.
- Pour sterile water onto clean gauze. Use sterile water to wash off the hydrogen peroxide. Start closest to your child's stoma and move outward. Use a new gauze every time you wipe a new area of his or her skin.
- Use a dry, clean, gauze to gently pat dry the area around his or her stoma.
- Apply antibacterial ointment only if directed by his or her healthcare provider.
- Clean the tube flanges. Dampen clean gauze with the hydrogen peroxide and water mixture. Gently scrub the flanges to remove mucus or crust.
- Change wet or dirty trach ties. Hold, your child's trach tube while you change the ties. Cut or peel the ties from the flanges. Wrap a new tie around your child's neck. Attach the ends of the tie to the flanges. Make sure you can fit 2 fingers between his or her neck and the tie. Ties that are too tight can make it difficult for your child to breath. Ties that are too lose can cause the tube to move out of place.
- Place a gauze between your child's skin and the flanges. Gauze will keep his or her skin clean and dry. You may not need to use gauze if your child does not have secretions. Do not cut the gauze. Fold the gauze instead so your child does not breathe in the cut fibers.
- Check your child's skin every day for signs of infection. Look for redness or swelling of the skin around his or her tube. Also look for pus, bleeding, or a rash.
How do I change my child's trach tube?
Change the trach tube as often as your child's healthcare provider directs. You may need to change the trach tube if it moves out of place. You may also need to change the tube if your child says that it feels uncomfortable.
- Prepare the new trach tube. Insert the obturator into the new tube. Test the cuff if your child's trach has one. Inflate the cuff with air to make sure it works, and then let the air out. Place a small amount of water-based lubricant on the lower end of the tube. Do not use petroleum jelly as a lubricant.
- Lay your child flat. Place a pillow or rolled up towel behind his or her neck. This will help tilt your child's head back and open his or her airway. Older children can sit up for tube changes.
- Deflate the cuff on your child's current trach tube if he or she has one. You can damage your child's airway or stoma if you do not deflate the cuff before you remove the tube. Your child's healthcare provider will show you how to deflate the cuff. Attach a syringe to the end of the cuff. Slowly pull back on the syringe to remove air.
- Remove your child's trach tube as he or she breathes out. Gently pull his or her trach tube up and out.
- Insert the new trach tube at a 90° angle. Point the tube in and then down. Remove the obturator immediately after the trach tube is in place. Insert a new or clean inner cannula if your child uses one.
- Inflate the cuff as directed if your child's trach has one. Your child's healthcare provider will show you how much air to put into the cuff. A cuff with too much air can leak, break, or harm your child's airway.
- Secure your child's trach tube with trach ties. Make sure that your child's trach ties are not too tight. You should be able to fit 2 fingers between the ties and his or her neck. Apply clean gauze between your child's skin and the flanges as directed.
How do I keep my child's secretions thin?
Help keep your child's secretions thin to help prevent his or her trach from becoming clogged. Thin secretions will make it easier for him or her to cough up fluid or mucus.
- Have your child drink plenty of liquids. Ask how much liquid your child needs to drink each day and which liquids are best for him or her.
- Put a warm humidifier in your child's room. Follow directions for cleaning the humidifier.
- Use devices that add moisture to your child's airway. Your child's healthcare provider will tell you if you need to use these devices. Use a heat moisture exchanger (HME), a trach collar, or fabric stoma covers as directed. An HME attaches to your child's trach tube and prevents moisture loss. A trach collar connects to a machine that supplies humidified air to his or her trach. Fabric stoma covers are moistened and worn over your child's trach tube.
What steps do I follow if my child is having trouble breathing?
- Have your child take deep breaths and cough. A strong cough may help move mucus, water, or irritants out of his or her airway.
- Suction your child's trach tube as directed. This will help remove things that are blocking his or her airway.
- Remove your child's inner cannula. Look for fluids or mucus inside the inner cannula. Remove and clean the inner cannula if it has mucus in it. You can also replace the inner cannula with a new one.
- Gently move your child's trach tube. Your child's tube opening may be against his or her airway. Gently reposition the tube to make sure it sits in the center of his or her airway.
- Replace your child's trach tube. Insert a new trach tube. Insert a smaller size if a regular sized tube will not go in properly.
- Call 911 if your child still has trouble breathing. Use a bag-mask over your child's stoma to give him or her breaths while you wait for help.
Call 911 for any of the following:
- Your child has trouble breathing even after you suction, clean, or change his or her trach tube.
- Your child coughs up bright red blood.
- You cannot insert a new trach tube.
- Your child stops breathing.
- Your child's lips turn blue.
When should I seek immediate care?
- You see food or liquids coming from your child's trach.
- Your child's breathing is faster than usual.
- Your child has blood coming from the trach or stoma.
When should I contact my child's healthcare provider?
- Your child has a fever.
- Your child has increased or thicker secretions than usual.
- Your child's secretions are yellow or green.
- Your child's skin around the tube is red, swollen, or draining foul-smelling fluid.
- Your child tells you that it hurts to swallow.
Care Agreement
You have the right to help plan your child's care. Learn about your child's health condition and how it may be treated. Discuss treatment options with your child's healthcare providers to decide what care you want for your child. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
