Tetanus in Children
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
Tetanus
is a disease caused by a bacterial infection. The bacteria are usually found in soil, dust, and the bowel movements of some animals and humans. The bacteria may enter your child's body through a skin wound. A mother can also pass the bacteria to her baby during a vaginal birth. The bacteria produce a toxin that damages nerves. This causes severe muscle spasms. Left untreated, tetanus can be life-threatening.
Common signs and symptoms:
Your child may have stiff and weak muscles only in the area of the wound. This is called localized tetanus. Symptoms may go away without treatment. Your newborn may start to have signs 3 to 14 days after birth. Your older child may develop signs or symptoms within days or months of the infection. The following are common signs and symptoms of tetanus:
- In newborns, trouble sucking and constant crying
- Lockjaw (a muscle spasm in the jaw and neck that locks your child's jaw closed)
- Muscle spasms that are severely painful, often triggered by noise, light, or touch
- Rigid facial muscles, or raised eyebrows with lips pulled into a grin
- Rigid abdomen, arm, and leg muscles
- Trouble breathing or swallowing
- Feeling restless or irritable, or a fast heartbeat or breathing
- A headache or seizures
- Sweating, trouble urinating, or a low fever
Call your local emergency number (911 in the US) if:
- Your child has trouble breathing or swallowing.
Call your child's pediatrician if:
- Your child's heartbeat is very fast or not regular.
- Your child has muscle spasms in his or her face.
- Your child starts to feel muscle cramps or spasms near a wound.
- Your child has a wound that is large or cannot be cleaned.
- Your child has an open wound or a puncture wound.
- You do not know if your child's tetanus vaccines are current.
- You have questions or concerns about your child's condition or care.
Treatment:
If the infection becomes generalized, your child will need to be treated in a hospital. He or she will be kept in a dark, quiet room to prevent muscle spasms. He or she may also need the following:
- Medicines may be given to stop or prevent seizures and muscle spasms. Antitoxin may also be given to stop the toxin from spreading in your child's body. Medicine may be given to fight a bacterial infection or to control pain. Your child's healthcare provider may also give your child a dose of the tetanus vaccine.
- Surgery may be used to remove tissue affected by tetanus. Debridement is a type of surgery used to clean a wound and remove dead tissue. Objects such as dirt or glass will also be removed.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
Prevent tetanus:
- Clean every wound immediately. Apply pressure to your child's wound to stop any bleeding. Clean the wound with soap and water. Remove dirt or other objects from the wound. Change the bandage every day and if it gets wet or dirty.
- Clean your baby's cord stump as directed. Always wash your hands before you care for your baby's cord stump. Gently wash the stump and the skin around it with mild soap and warm water during every bath. Gently pat the stump dry after your baby's bath. If the stump gets dirty from urine or bowel movement, wash it off right away. Your baby's healthcare provider may suggest you use rubbing alcohol or water and a cotton swab to clean the stump. Gently wipe from the base to the top of the stump. Clean the stump with each diaper change.
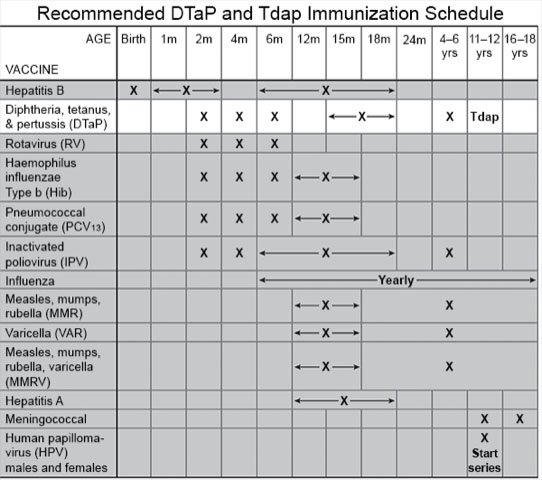
- Talk to your child's healthcare provider about vaccines. A tetanus infection will not make your child immune from another infection. The DTaP, Tdap, and Td vaccines help protect against tetanus. The vaccines are given to children in several doses. Your child's provider can help you create a schedule so you know when to bring your child in. If your adolescent is pregnant, she should receive 1 dose of Tdap during weeks 27 to 36.
Follow up with your child's pediatrician as directed:
Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Tetanus
Treatment options
Care guides
Symptoms and treatments
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
