Tendon Laceration
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a tendon laceration?
A tendon laceration is a tear or break in your tendon. A tendon is a string of tissue that connects muscle to bone. Tendons help muscles make bones move. A tendon laceration may be caused by too much pressure or force to a joint or body part. It may also be caused by deep cut. A tendon laceration is most commonly caused by deep cut to your hand, finger, wrist, foot, or toes.
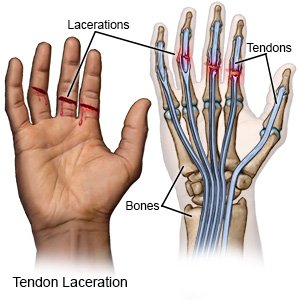 |
What are the signs and symptoms of a tendon laceration?
The location of signs and symptoms may depend on where in your body your tendon is lacerated. You may have any of the following:
- A deep cut or wound in the skin that covers the tendon
- Trouble straightening or bending the body part with the tendon laceration
- Pain
- Swelling or bruising
How is a tendon laceration diagnosed?
Your healthcare provider will examine you and ask about your symptoms. You may need an MRI, x-ray, or ultrasound to look for a break or tear in your tendon.
How is a tendon laceration treated?
If your tendon laceration was caused by a cut in your skin, you may need wound care. Your skin and tissue will be cleaned. The edges of your skin will be stitched together. You may also need any of the following:
- Medicines may be given to decrease pain or swelling. You may also need antibiotics or a tetanus shot to prevent infection.
- A splint or cast may be needed to help your tendon heal. These devices will keep your tendon straight and prevent movement.
- Tendon repair surgery may be needed. During a tendon repair the edges of your tendon will be stitched back together. Your healthcare provider may use a tendon from another part of your body to fix your tendon.
How can I manage my symptoms?
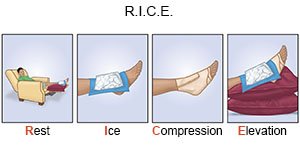 |
- Rest your arm or leg to help it heal.
- Apply ice on your arm or leg for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover it with a towel. Ice helps prevent tissue damage and decreases swelling and pain.
- Elevate your arm or leg above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your injured body part on pillows or blankets to keep it elevated comfortably.
- Wear your splint as directed. A splint will keep your tendon straight and prevent movement. This will help your tendon heal. Check your skin under your splint for redness, swelling or open skin. You may need to change your splint when it gets wet or dirty. Ask your healthcare provider how to change your splint.
- Perform range of motion exercises (ROM) as directed. ROM exercises are gentle movements of your joint. ROM exercises will prevent stiffness in your arm or leg and help build strength. Do not do ROM exercises unless your healthcare provider says it is okay.
When should I seek immediate care?
- Blood soaks through your bandage.
- Your stitches come apart.
- Your hand, fingers, foot, or toes closest to your injury are pale, numb, or cold.
- You hear or feel a sudden snap, pop, or crack where your tendon is lacerated.
- You have sudden severe pain where your tendon is lacerated.
When should I call my doctor?
- You have a fever.
- Your wound is swollen, red, or draining pus.
- Your pain does not get better after you take your medicine or gets worse.
- Your splint or cast falls off.
- Your skin under the splint is red, swollen, or open.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Learn more about Tendon Laceration
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
