Finger Laceration
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a finger laceration?
A finger laceration is an injury to your skin and the soft tissue under it. Your blood vessels, bones, joints, tendons, or nerves may also be injured.
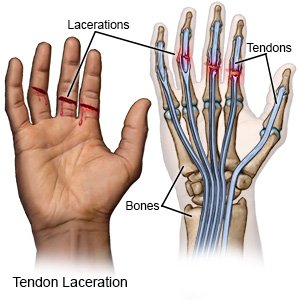 |
What are the signs and symptoms of a finger laceration?
Your symptoms may depend on whether nerves, tendons, or deeper tissues were injured. You may have any of the following:
- A cut, tear, or gash in your finger
- Bleeding, swelling, or pain
- Numbness or tingling in your finger
- Trouble moving your finger
How is a finger laceration diagnosed?
- Tell your healthcare provider how you got your laceration. Your provider will examine your wound and decide what treatment you need. An x-ray, ultrasound, or CT may show foreign objects in the wound. Foreign objects include metal, gravel, and glass. The tests may also show damage to deeper tissues.
- You may be given contrast liquid to help the injured area show up better in the pictures. Tell the provider if you have ever had an allergic reaction to contrast liquid.
How is a finger laceration treated?
Treatment depends on how large and deep the laceration is. It also depends on whether you have damage to deeper tissues. You may need any of the following:
- Pressure may be applied to stop bleeding.
- Wound cleaning may help remove dirt or debris. This will decrease the risk for infection. Your healthcare provider may need to look inside your wound for foreign objects or damage to deeper tissues. Your provider may give you medicine to numb the area and decrease pain. You may also be given medicine to help you relax.
- Wound closure with stitches, staples, tissue glue, or medical strips may be needed. These may help the wound heal and prevent infection. Your provider may give you medicine to numb the area and decrease pain. You may also be given medicine to help you relax. Stitches may decrease the amount of scarring you have. Some lacerations may heal better without stitches.
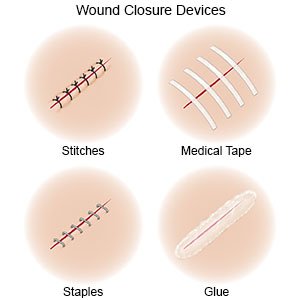
- Medicine may be given to treat pain or decrease your risk for infection. You may also be given a tetanus shot. Your provider will decide if you need a tetanus shot. Wounds at high risk for tetanus infection include wounds with dirt or saliva in them. You should get a tetanus shot within 72 hours of getting a laceration or wound. Tell your provider if you have had the tetanus vaccine or a booster within the last 5 years.
- Surgery may be needed to clean your wound and remove foreign objects. Surgery may also be needed to repair injuries to tendons, nerves, or bones.
How can I manage my symptoms?
- Apply ice to the wound for 15 to 20 minutes every hour or as directed. Use an ice pack, or put crushed ice in a plastic bag. Cover the bag with a towel before you apply it to your skin. Ice helps decrease swelling and pain.
- Elevate your hand above the level of your heart as often as you can. This will help decrease swelling and pain. Prop your hand on pillows or blankets to keep it elevated comfortably.

- Use a splint as directed. A splint will decrease movement and stress on your wound. The splint may help your wound heal faster. Ask your healthcare provider how to apply and remove a splint.
- Decrease wound scarring. You may need to apply ointments to your wound or the area around it. Ask which ointment to buy and how often to use it. You may need to wait until your wound is healed. After your wound is healed, use sunscreen over the area when you are out in the sun. The skin around your wound may turn a different color if it is exposed to direct sunlight. You should do this for at least 6 months to 1 year after your injury.
When should I seek immediate care?
- Your wound reopens.
- You have heavy bleeding or bleeding that does not stop after 10 minutes of holding firm, direct pressure over the wound.
- Your finger is pale and cold.
- You have new tingling, weakness, or numbness near the wound.
- You have trouble moving your finger.
- You have red streaks on your skin coming from your wound.
When should I call my doctor or hand specialist?
- You have a fever or chills.
- You have pain in your finger or hand that gets worse, even after treatment.
- Your wound is red, warm, or swollen.
- You have white or yellow drainage from the wound that smells bad.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
