Spontaneous Pneumothorax
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is a spontaneous pneumothorax?
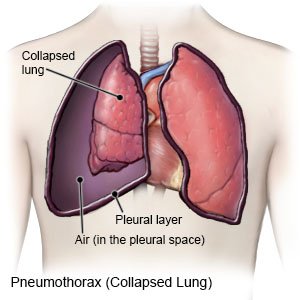
A spontaneous pneumothorax is a collapsed lung. Part or all of the lung may collapse. Air collects in the pleural space (the space between the lungs and chest wall). The trapped air prevents your lung from filling, and the lung collapses. A spontaneous pneumothorax can happen in one or both lungs. A primary spontaneous pneumothorax occurs in a person with no known lung problems. A secondary spontaneous pneumothorax occurs in a person who has a known lung disease or medical condition.
 |
What causes a spontaneous pneumothorax?
A spontaneous pneumothorax has no clear cause. It may occur when an air pocket in the lung breaks open. This allows air to leak out and become trapped in the pleural space. Air may also enter the pleural space if your lung tissue is damaged.
What increases my risk for a spontaneous pneumothorax?
- Being a tall, thin male
- Scuba diving, flying, or climbing to high altitudes
- Smoking
- Lung conditions such as cystic fibrosis, COPD, emphysema, pulmonary fibrosis, or severe asthma
- A lung infection, such as pneumonia or TB
- A tumor, such as cancer
- An autoimmune disorder, such as ankylosing spondylitis, rheumatoid arthritis, scleroderma, or sarcoidosis
- Catamenial, a condition that causes a pneumothorax 1 to 3 days after a woman's monthly period begins
What are the signs and symptoms of a spontaneous pneumothorax?
- Shortness of breath
- Chest pain
- Chest movement that is not even when you breathe
- A fast heartbeat
How is a spontaneous pneumothorax diagnosed?
Your healthcare provider will ask about your signs and symptoms and examine you. He or she will listen to your lungs. You may also need any of the following:
- Blood tests are used to check your oxygen and carbon dioxide levels. The results can tell healthcare providers how well your lungs are working.
- A heart monitor is used to record your heart's electrical activity.
- X-ray pictures of the bones, lungs, and other tissues in your chest will show if you have broken ribs. The pictures may also show the size of the pneumothorax and if you have fluid around your heart and lungs.
- CT scan or ultrasound pictures may be used to check for a pneumothorax that did not show up on a chest x-ray. You may be given contrast liquid to help your lungs show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
How is a spontaneous pneumothorax treated?
Treatment will depend on the size of your pneumothorax. If your pneumothorax is small, it may get better on its own. The goal of treatment is to remove the air from your pleural space. When your lung is able to fill with air, you will be able to breathe easier. You may need any of the following:
- Extra oxygen may be given if your oxygen level is too low. Oxygen may help the pneumothorax get better faster.
- Antibiotics may be given to prevent or treat a bacterial infection.
- Prescription pain medicine may be given. Ask your healthcare provider how to take this medicine safely. Some prescription pain medicines contain acetaminophen. Do not take other medicines that contain acetaminophen without talking to your healthcare provider. Too much acetaminophen may cause liver damage. Prescription pain medicine may cause constipation. Ask your healthcare provider how to prevent or treat constipation.
- Needle aspiration is used to pull the air out of your pleural space through a needle.
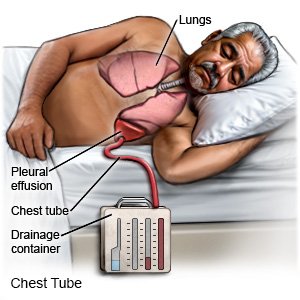
- A chest tube may be placed to remove air, blood, or fluid from around your collapsed lung. This allows your lung to fill with air when you breathe, and helps your heart beat normally. The chest tube is attached to a container to remove air and collect any blood or fluid.
- Pleurodesis is a procedure used to irritate the walls of your pleural space. This causes the walls to close so air can no longer be trapped.
- Surgery may be used to repair your lung.
What safety precautions should I follow?
A change of pressure could cause another pneumothorax. Follow these and other safety precautions from your healthcare provider:
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase your risk for another pneumothorax. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes and smokeless tobacco still contain nicotine. Talk to a healthcare provider before you use these products.
- Do not dive under water or climb to high altitudes.
- Do not fly until your provider says it is okay.
- Do not play sports until your provider says it is okay.
Call your local emergency number (911 in the US), or have someone call if:
- You have new or increased shortness of breath or chest pain.
- Your throat or the front of your neck is pushed to one side.
- You are sweating and feel like you are going to pass out.
- Your fingernails, toenails, or lips begin to turn blue.
- You have trouble thinking clearly.
When should I call my doctor?
- You have a fever.
- You hear a crackling noise or feel popping when you touch your skin.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
