Seizures after Traumatic Brain Injury
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
AMBULATORY CARE:
What you need to know about seizures after a traumatic brain injury (TBI):
You are at higher risk for a seizure after a TBI. A seizure is an episode of abnormal brain activity. A seizure may happen within hours after your TBI or weeks to years later. A seizure within a week of a TBI is called an early posttraumatic seizure. This may be caused by bleeding between your brain and skull. Brain swelling can also cause a seizure. Seizures that happen at least 1 week after the TBI is called a late posttraumatic seizure. This may be caused by permanent damage to your brain. Late posttraumatic seizures increase your risk for developing epilepsy. Epilepsy is a brain disorder that causes repeated seizures. Epilepsy is a brain disorder that causes recurrent seizures.
Call 911 or have someone else call for any of the following:
- Your seizure lasts longer than 5 minutes.
- You have a second seizure within 24 hours of the first.
- You have trouble breathing after a seizure.
- You cannot be woken after your seizure.
- You have more than 1 seizure before you are fully awake or aware.
Seek care immediately if:
- You are injured during a seizure.
Contact your healthcare provider if:
- You have a fever.
- You start to have seizures more often.
- You have questions or concerns about your condition or care.
Common signs and symptoms of a seizure:
Your seizure may be defined as one type of a seizure or a combination. Each type of seizure may have different symptoms. You may have symptoms before the seizure starts. This is called an aura. Examples include dizziness, anxiety, or flashing bright lights. You may have any of the following:
- A generalized seizure may affect both sides of the brain. After you have a generalized seizure, you may have a headache or feel irritable. The following are different types of generalized seizures:
- A tonic, clonic, or tonic-clonic seizure usually involves the whole body. A clonic seizure involves jerking body movements. A tonic seizure involves stiffening of the body. A tonic-clonic seizure is a combination of clonic and tonic seizures. It is also called a grand mal seizure. During any of these types of seizures, you may lose consciousness. Your eyes may roll up and back into your head, and you may sweat all over your body.
- A myoclonic seizure involves a sudden jerk of all or part of the body.
- An atonic seizure is usually brief and causes a sudden loss of posture. You may fall suddenly to the ground.
- An absence seizure is also known as a petit mal seizure. You may stare blankly into space, and will not pay attention to anything happening around you. Your eyes may flutter or blink repeatedly, and you may smack your lips. You may have several absence seizures throughout a day.
- An atypical absence seizure looks like an absence seizure but with repetitive behaviors such as eye opening and closing, eyes rolling outward or inward, and body stiffening.
- A partial seizure may affect one part of the brain. The symptoms may depend on where in the brain the abnormal activity is happening. It may be simple or complex. A simple partial seizure may not cause a loss of consciousness. A complex partial seizure may cause you to be less awake or alert. Both types of partial seizures may cause jerky muscle movements, confusion, hallucinations, sweating, or repetitive behaviors.
Treatment:
Medicine may be given to prevent a seizure. Medicine may also be given during a seizure to stop it. You may be given seizure medicine through your IV or as a pill.
What you can do to manage or prevent seizures:
- Keep a seizure diary. Include when the seizure started and how long it lasted. Also include what you were doing before the seizure started and if you had an aura. Ask anyone who saw you have the seizure what you did during and after the seizure. Bring the seizure diary with you to all follow-up visits.
- Set a regular sleep schedule. A lack of sleep can trigger a seizure. Try to go to sleep and wake up at the same times every day. Keep your bedroom quiet and dark. Talk to your healthcare provider if you are having trouble sleeping.
- Limit or do not drink alcohol as directed. Alcohol can trigger a seizure, especially if you drink a large amount at one time. A drink of alcohol is 12 ounces of beer, 1½ ounces of liquor, or 5 ounces of wine. Talk to your healthcare provider about a safe amount of alcohol for you. Your provider may recommend that you do not drink any alcohol. Tell him or her if you need help to quit drinking.
- Ask what safety precautions you should take. Talk with your healthcare provider about driving. You may not be able to drive until you are seizure-free for a period of time. You will need to check the law where you live. Also talk to your healthcare provider about swimming and bathing. You may drown or develop life-threatening heart or lung damage if you have a seizure in water.
- Tell your friends, family members, and coworkers that you had a seizure. Give them written instructions to follow if you have another seizure.
What others can do to keep you safe during a seizure:
Give the following instructions to family, friends, and coworkers:
- Do not panic.
- Gently guide me to the floor or a soft surface.
- Do not hold me down or put anything in my mouth.
- Place me on my side to help prevent me from swallowing saliva or vomit.
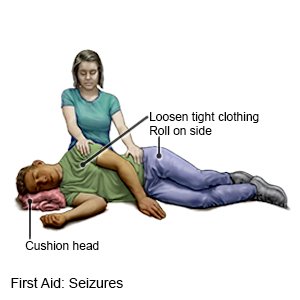
- Protect me from injury. Remove sharp or hard objects from the area surrounding me, or cushion my head.
- Loosen the clothing around my head and neck.
- Time how long my seizure lasts. Call 911 if my seizure lasts longer than 5 minutes or if I have a second seizure.
- Stay with me until my seizure ends. Let me rest until I am fully awake.
- Perform CPR if I stop breathing or you cannot feel my pulse.
- Do not give me anything to eat or drink until I am fully awake.
Follow up with your healthcare provider or neurologist as directed:
You may need tests to check the level of antiseizure medicine in your blood. Your neurologist may need to change or adjust your medicine. Write down your questions so you remember to ask them during your visits.
© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.
Learn more about Seizures after Traumatic Brain Injury
Care guides
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
