Pulmonary Fibrosis
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is pulmonary fibrosis?
Pulmonary fibrosis is the scarring of your lung tissues over time. It is also called interstitial lung disease. The air sacs and tissues in your lungs swell, scars form, and the tissues become thick and stiff. This affects how much oxygen you get and makes it hard to breathe.
 |
What increases my risk for pulmonary fibrosis?
The cause of pulmonary fibrosis may not be known. The following may increase your risk:
- Family history of pulmonary fibrosis or other lung disease
- Chemicals, such as asbestos, silica, or pesticides
- Tobacco smoke
- Medical conditions, such as acid reflux, arthritis, or diabetes
- Medicines, such as antibiotics and antidepressants
- Treatment for medical conditions, such as radiation
What are the signs and symptoms of pulmonary fibrosis?
- Trouble breathing that gets worse over time
- Dry cough
- Fast heartbeat
- Clubbing of fingertips and nails (become large, blunt, and rounded)
- Tiredness and weakness
How is pulmonary fibrosis diagnosed?
Your healthcare provider will examine you and ask about your symptoms. You may also need any of the following:
- Blood tests may show damage to your organs from a lack of oxygen. The amounts of oxygen and carbon dioxide in your blood will be checked. The results can tell healthcare providers how well your lungs are working. Blood tests may also be used to check for signs of an allergic reaction. Your body may be creating inflammation as a response to something you are allergic to.
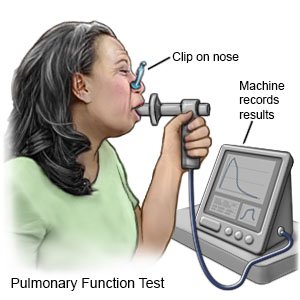
- Pulmonary function tests (PFTs) will show how much oxygen your body is getting. You breathe into a mouthpiece connected to a machine. The machine measures how much air you breathe in and out over a certain amount of time.
- CT scan pictures of your lungs may show tissue damage. You may be given contrast liquid before the pictures are taken to help healthcare providers see your lungs better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- An echocardiogram is a type of ultrasound used to check for high blood pressure in your lungs and heart. It may also show damage to your heart tissue.
- A bronchoscopy is a procedure to look inside your airway. A bronchoscope (thin tube with a light) is inserted into your mouth and moved down your throat to your airway.
- A sample of lung tissue may be sent to a lab for tests. The sample may be taken during a bronchoscopy, through surgery, or frozen and removed through a procedure called cryobiopsy.
How is pulmonary fibrosis treated?
There is no cure for pulmonary fibrosis. The goal of treatment is to slow the progress of the disease and treat your symptoms. You may need any of the following:
- Extra oxygen may be needed if your blood oxygen level is lower than it should be. You may get oxygen through a mask placed over your nose and mouth or through small tubes placed in your nostrils.
- Medicines may be given to decrease lung tissue swelling and help prevent scarring.
- Surgery may be needed if you have severe trouble breathing. You may need part of your lung removed or a lung transplant.
Treatment options
The following list of medications are related to or used in the treatment of this condition.
How can I manage pulmonary fibrosis?
- Use oxygen at home as directed. Oxygen is usually given through a nasal cannula. This is a pair of short, thin tubes that rest just inside your nose. Tell your healthcare provider if your nose gets dry or if the skin gets red or sore. Never smoke or let anyone else smoke in the same room while your oxygen is on.
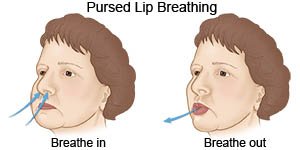
- Do breathing exercises as directed. Breathe out with pursed or puckered lips. Use your diaphragm to breathe. Put one hand on your abdomen and breathe in, causing your hand to move outward or upward. This helps make more room so your lungs can take in more air.
- Go to pulmonary rehab as directed. Specialists will help you safely strengthen your lungs and prevent more tissue damage. The plan includes education about your condition, exercise, breathing strategies, and ways to conserve energy. Pulmonary rehab may help decrease your breathing problems and help you function better in your daily activities.
- Get the flu vaccine. The flu can become serious in anyone who has a lung condition. Get the flu vaccine as soon as recommended each year, usually in September or October. You may also need the pneumococcal vaccine to prevent pneumonia.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can increase the damage to your lung tissue. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
Where can I find more information?
- American Lung Association
1301 Pennsylvania Ave. NW
Washington , DC 20004
Phone: 1- 202 - 785-3355
Phone: 1- 800 - 548-8252
Web Address: www.lung.org
- Pulmonary Fibrosis Foundation
230 East Ohio Street
Chicago , IL 60611-3201
Phone: 1- 888 - 733-6741
Web Address: www.pulmonaryfibrosis.org
Call your local emergency number (911 in the US) if:
- You have sudden severe trouble breathing.
- You have a fast heartbeat or chest pain.
- Your shortness of breath gets worse.
- You feel so dizzy that you cannot stand up.
When should I call my doctor?
- You have a fever.
- You cough up bloody mucus.
- You are wheezing.
- Your lips or fingernails turn blue.
- You have swelling in your legs or feet.
- You need more oxygen than you used to.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
