Pleural Mesothelioma
Medically reviewed by Drugs.com. Last updated on Aug 4, 2025.
What is pleural mesothelioma?
Pleural mesothelioma is a rare type of cancer that develops in a protective covering for your lungs called the pleura. The pleura is piece of tissue with 2 layers. One layer lines your chest cavity and the other covers your lungs.
 |
What causes mesothelioma?
- Asbestos is the most common cause. Asbestos is a mineral. It may be found in older homes and buildings, and it forms naturally in many areas. Asbestos breaks easily into small threads when it is disturbed. For example, when an older building is torn down, the dust from the building contains asbestos threads. You may breathe in the threads without realizing it. Asbestos can stay in your lungs for over 40 years, irritating and inflaming the tissues. This causes changes that lead to cancer.
- You may also develop mesothelioma tumors if you are exposed to talc, erionite, or mica.
- Familial Mediterranean fever or diffuse lymphocytic leukemia can also cause these tumors to form.
What increases my risk for pleural mesothelioma?
- Being male or having a family history of mesothelioma
- Working as a miner or miller of fibers
- Work with textiles, cement, friction materials, insulation, or shipbuilding
- Renovation or destruction of a building that contains asbestos
- Being exposed to or handling the clothing of a person who works with asbestos
- Living with a person who handles or works near asbestos
What are the signs and symptoms of pleural mesothelioma?
The following will develop slowly, over a long period of time:
- Shortness of breath
- A cough that continues
- Chest pain under your rib cage
- Lumps on your chest, under the skin
- Weight loss without trying, or loss of appetite
- Tiredness most of the day
- Fever or sweating
How is pleural mesothelioma diagnosed?
Your healthcare provider will examine you and ask about your symptoms. Tell your provider if you have ever worked around or been exposed to asbestos or a chemical that can cause pleural mesothelioma. Tell your provider how long ago this happened, and how long you were exposed. You may also need any of the following:
- X-ray or CT scan pictures can help show if you have pleural mesothelioma. You may need to have pictures taken again to help your provider find the stage of the cancer. This means your provider will be looking to see if the cancer has spread. Ultrasound pictures may also be used for staging. You may be given contrast liquid before some of these tests to help the cancer cells show up better in the pictures. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- A biopsy is a procedure used to take a sample of tissue to be tested for mesothelioma cells.
- Thoracoscopy or thoracotomy are procedures that may be done to check inside your chest for signs of mesothelioma. An incision will be made between two of your ribs. If you have a thoracoscopy, a scope will be guided into your chest. The scope will help your healthcare provider see inside your chest more easily.
- A pulmonary function test is used to check how well your lungs are working. This test measures the amount of air your lungs can hold and how quickly air moves into and out of your lungs. The amount of oxygen used and carbon dioxide given off while you breathe are also measured.
How is pleural mesothelioma treated?
- Surgery may be used to remove the mesothelioma cells. Part of the pleura may also be removed. A whole lung may be removed, along with part of the lining of the chest.
- Radiation is used to kill cancer cells or keep them from growing. You may also need radiation after surgery to prevent the cancer from coming back.
- Chemotherapy uses drugs to stop cancer cells from growing. You may also need chemotherapy before surgery to make the tumor smaller. You may need it after surgery to prevent the cancer from coming back.
- Targeted therapy is used to kill only cancer cells but leave healthy tissue. Medicines may be used to help your immune system recognize and destroy mesothelioma cells. Medicines may bind to the mesothelioma cells and kill them or prevent them from dividing. Some medicines may be used to destroy blood vessels that are connected to the tumor. This prevents the tumor from getting oxygen and nutrients it needs to grow.
What can I do to manage or prevent pleural mesothelioma?
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can irritate your lungs and make breathing more difficult. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
- Ask about vaccines you may need. Pleural mesothelioma increases your risk for pneumonia, influenza (the flu), and COVID-19. Vaccines are available to help protect you. Your provider can tell you if also need vaccines not listed below:
- Ask your healthcare provider about the flu and pneumonia vaccines. All adults should get the flu (influenza) vaccine as soon as recommended each year, usually in September or October. The pneumonia vaccine is recommended for all adults aged 50 or older to prevent pneumococcal disease, such as pneumonia. Adults aged 19 to 49 years who are at high risk for pneumococcal disease should also receive the vaccine. You may need 1 dose or 2. The number depends on the vaccine used and your risk factors.
- COVID-19 vaccines are given to adults as a shot. At least 1 dose of an updated vaccine is recommended for all adults. COVID-19 vaccines are updated throughout the year. Adults 65 or older need a second dose of updated vaccine at least 4 months after the first dose. Your healthcare provider can help you schedule all needed doses as updated vaccines become available.
- Have your home tested for asbestos. You can decrease your exposure to asbestos by having your home tested and treated, if needed. Ask your healthcare provider how to get your home tested. If asbestos is found in your home, do not try to remove it yourself. Have a professional remove it.
- Limit your exposure to harmful chemicals in the workplace. Asbestos and other harmful chemicals can be found in mines, mills, textile plants, and shipyards. Follow procedures and policies to protect yourself at work. Use protective equipment such as masks to decrease your risk of inhaling harmful chemicals.
What can I do to manage my symptoms?
- Sit near a running fan when you have shortness of breath. This can help relieve the feeling that you are not getting enough air.
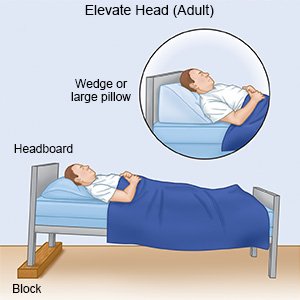
- Keep your head elevated. You may be able to breathe better if you lie down with the head of your bed up.
- Use exercises to clear your airway clearance as directed. The exercises help remove mucus so you can breathe more easily. Your healthcare provider will show you how to do the exercises.
- Drink liquids as directed. Ask how much liquid to drink each day and which liquids are best for you. Liquids help thin your mucus, which may make it easier for you to cough it up.
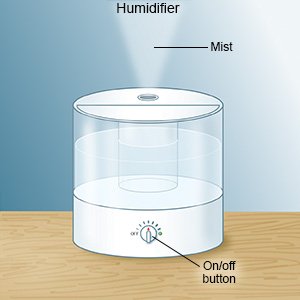
- Use a cool mist humidifier. A humidifier will help increase air moisture in your home. This may make it easier for you to breathe and help decrease your cough.
- Ask about ways to help relieve pain. Your provider may recommend medicines to prevent or relieve pain. He or she may also recommend ways to control pain without medicine. Examples include a heat or ice pack, or listening to music. Ask for more information on ways to control your pain.
When should I seek immediate care?
- You have severe pain and it is not time to take your pain medicine yet.
- You have chest pain when you take a deep breath or cough.
- You cough up blood.
- You cannot think clearly.
- Your lips or nails look blue or pale.
When should I call my doctor?
- You have moderate pain and it is not time to take your pain medicine yet.
- You have pain even after you take your pain medicine.
- You have a new pain or the pain seems different than before.
- You have a fever.
- You have questions or concerns about your condition or care.
Care Agreement
You have the right to help plan your care. Learn about your health condition and how it may be treated. Discuss treatment options with your healthcare providers to decide what care you want to receive. You always have the right to refuse treatment. The above information is an educational aid only. It is not intended as medical advice for individual conditions or treatments. Talk to your doctor, nurse or pharmacist before following any medical regimen to see if it is safe and effective for you.© Copyright Merative 2025 Information is for End User's use only and may not be sold, redistributed or otherwise used for commercial purposes.
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
